Mariona Ribo
Few pharmacists have experience handling advanced therapy medicinal products (ATMPs) — medicines based on genes, cells or tissue engineering — but the field is likely to grow and presents special challenges for pharmacists, according to Lenka Taylor, head of clinical trials at University Hospital in Heidelberg, Germany.
Two tissue-engineered ATMPs are currently approved by the European Medicines Agency: characterised viable autologous cartilage cells (ChondroCelect; TiGenix), used to repair damaged cartilage in the knee; and limbal stem cells (from the cornea) (Holoclar; Chiesi Farmaceutici) for the treatment of limbal stem cell deficiency (LSCD), a condition that can cause blindness.
ATMPs also include gene therapy medicines, such as Glybera (alipogene tiparvovec), a virus-derived protein vector used to treat patients with lipoprotein lipase deficiency; or somatic cell therapy medicines, such as Provenge, a treatment for prostate cancer prepared from patients’ peripheral blood mononuclear cells, which was withdrawn for commercial reasons in 2015.
Speaking at the 2016 congress of the European Association of Hospital Pharmacists, held in Vienna from 16–18 March 2016, Taylor told delegates that ATMPs are governed not only by medicines’ regulations but also by a number of other EU instruments covering tissue cells and viability, blood products and genetically modified organisms.

Source: Mariona Ribo
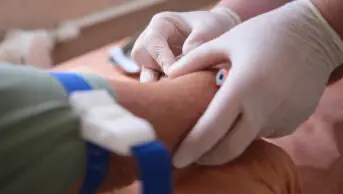
Pharmacists need to understand how to handle advanced therapy medicinal products safely, said Anne Black, assistant director of pharmacy at Newcastle-upon-Tyne Hospitals NHS Foundation Trust
“It is a largely uncomfortable area for pharmacists,” said Anne Black, assistant director of pharmacy at Newcastle-upon-Tyne Hospitals NHS Foundation Trust, who was also speaking at the event and described her first contact with ATMPs when she encountered the harvesting of limbal cells from a patient’s cornea for ocular surface reconstruction to treat LSCD. “However, ATMPs are often injectable and they are medicines and so pharmacists need to understand how to handle them safely.”
Pharmacists are most likely to encounter ATMPs in a clinical trial setting and may be called upon to reconstitute them.
Some 650 trials of investigational ATMPs have been registered in Europe, 187 of which involve tissue-engineered products, 160 involve gene therapy products and 307 involve somatic cell products.
Black outlined several scenarios in which pharmacists could encounter ATMPs. The first was in-house manufacturing of an ATMP, for which a manufacturing licence would be required. An example of this is Black’s experience at Newcastle with the manufacture of tolerogenic dendritic cells for treatment of rheumatoid arthritis, where blood was taken from the patient and CD14-positive monocytes were then expanded in preparation for injection back into the patient.
She gave LSCD treatment as another example, in which limbal stem cells are harvested from a patient’s good eye, seeded onto human amniotic membrane and grown in a laboratory for seven days. The cultured cells are then transplanted to the damaged eye.
More commonly, raw material is procured on-site and then sent away for manufacture, with the final product returned to the hospital for administration to the patient. Pharmacists’ understanding of ‘good practice’ guidance is an asset here, commented Black, because these processes require the application of good tissue practice, good manufacturing practice and good clinical practice.
When ATMPs are made off-site, they are often either stored in a freezer or in liquid nitrogen and have to be defrosted before administration. Black explained that these products commonly have to be prepared in clinical areas for immediate administration, with no time to prepare them in an aseptic facility. It is possible that the whole process – manufacture, release, transportation and administration – takes place within 24 hours and as a result hospital procedures need to be established to make this possible, she said.