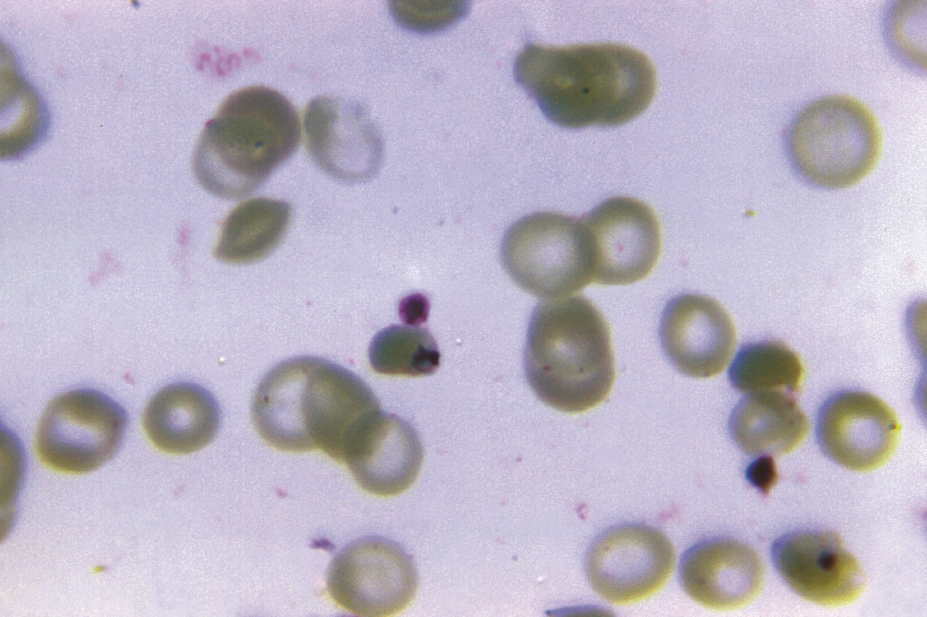
CDC / Neva Gleason
Artemether-lumefantrine, the most widely used antimalaria treatment in Africa and the one recommended for treating imported cases of the disease in the UK, is starting to fail, possibly because the parasite responsible for most cases of malaria in Africa is becoming resistant to it, experts have warned.
The warning has come after four patients who visited Angola, Uganda or Liberia were treated for Plasmodium falciparum malaria when they returned to the UK. At first, they responded to treatment with the artemisinin-based combination therapy (ACT), but in all cases, which occurred between October 2015 and February 2016, malaria symptoms returned within six weeks. The patients’ conditions improved with alternative treatment.
Researchers from the London School of Hygiene and Tropical Medicine describe the cases in Antimicrobial Agents and Chemotherapy
[1]
(online, 30 January 2017), and say: “Vigilance for signs of unsatisfactory antimalarial efficacy among imported cases of malaria is recommended.”
They concede that “treatment failure cannot be unequivocally” attributed to parasite resistance in these patients and point out that artemisinin-based drugs are quickly metabolised and cleared from circulation. This means only a single full parasite lifecycle is exposed to the compounds.
“The current practice of three days of treatment may therefore be insufficient to guarantee [parasite] clearance,” the researchers say, adding that patients should be given two sequential artemisinin-based therapies, such as artemether-lumefantrine followed by three days of either artesunate-amodiaquine or dihydroartemisinin-piperaquine.
This treatment strategy would provide six days of artemisinin with two longer half-life “partner drugs”.
“This approach should also be considered as a potential strategy should increasing numbers of treatment failures be observed after standard ACT regimens for imported malaria cases in non-endemic countries,” they add.
“In the majority of cases, ACT retains its efficacy against P.
falciparum of African origin, but the cases presented here suggest this favourable situation may deteriorate in the future.”
References
[1] Sutherland CJ, Lansdell P, Sanders M et al. Pfk13 -independent treatment failure in four imported cases of Plasmodium falciparum malaria given artemether-lumefantrine in the UK. 30 January 2017. Antimicrobial Agents and Chemotherapy. doi: 10.1128/AAC.02382-16
You may also be interested in

Recognition and management of whooping cough
Everything you need to know about meningitis B
