Shutterstock.com
Source: Shutterstock.com
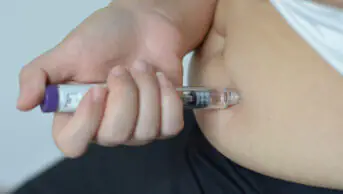
FDA approves new heart failure combination therapy
The US Food and Drug Administration (FDA) has approved a new drug for heart failure that has “overwhelming benefit” for patients, according to the researchers who trialled the medicine.
Entresto is a combination of the angiotensin receptor blocker valsartan and the novel neprilysin inhibitor sacubitril. In a trial of more than 8,000 patients (called PARADIGM-HF and published in The New England Journal of Medicine in 2014) the drug combination was more effective than the current gold standard treatment. Entresto reduced deaths and hospital admissions by 20% compared with enalapril and the trial was stopped seven months early. However, the new combination increases the risk of angioedema.
The FDA reviewed the medicine under its priority review programme and granted it fast-track designation, processes reserved for drugs that treat a serious illness and either provide a significant benefit over current medication or meet an unmet medical need, respectively.
The medicine is currently being assessed for a licence by the European Medicines Agency.

Source: Shutterstock.com
MPharm degree fails to equip pharmacists for future roles
The existing Master of Pharmacy (MPharm) degree offered by British universities fails to equip pharmacists with the skills needed to deliver the care and the services that will be expected of them in the future, according to the profession’s regulator.
The current MPharm degree and pre-registration training year needs to be integrated so that would-be pharmacists are capable of delivering patient-centred care, have exemplary communication and people skills and naturally fit into a multidisciplinary team working in different care settings, the General Pharmaceutical Council (GPhC) says.
Integration is essential to meet political expectations of the pharmacy team, the GPhC says in its discussion paper on the future training and education of pharmacists, pharmacy technicians and pharmacy-support staff published on 16 June 2015.
The discussion paper, entitled ‘Tomorrow’s pharmacy team: future standards for initial education and training of pharmacists, pharmacy technicians and pharmacy support staff’ and an accompanying survey, which runs until 14 August 2015, are on the GPhC website.
NHS England launches pilot to employ pharmacists in GP practices
GP practices in England will employ around 300 pharmacists to provide clinical care in a £15m pilot, NHS England has announced.
NHS England will subsidise practices to employ pharmacists in patient-facing roles, with responsibilities including monitoring patients with long-term conditions, creating medicine plans and providing advice and expertise on day-to-day medicines issues.
The pilot will start in 2015 and run until 2018. Pharmacists will be recruited in areas where GPs are under the greatest pressure because of workload.
NHS England will fund 60% of pharmacists’ salary costs in year one, 40% in year two and 20% in year three.
European Medicines Agency starts safety review of HPV vaccines
A safety review of human papillomavirus vaccines has been launched by the European Medicines Agency (EMA).
The review will look at rare reports of complex regional pain syndrome (CRPS) or postural orthostatic tachycardia syndrome (POTS) associated with the vaccines to try to determine whether there is a causal link. The review will not question whether the benefits of the vaccines outweigh their risks.
Both conditions can occur in non-vaccinated individuals and the EMA wants to discover whether the number of reports of CRPS and POTS among women who receive the vaccines matches the number expected among the general population.

Source: Shutterstock.com
Community pharmacists to access the summary care record
All community pharmacists in England are being given access to the summary care record (SCR) from autumn 2015, health minister Alistair Burt announced on 23 June 2015. The SCR contains clinical information about a patient, obtained from the record maintained by the patient’s GP.
The decision follows the success of a pilot project involving 140 pharmacies in England given access to the SCR.
An analysis of the pilot’s findings suggests that by accessing information contained within the SCR, pharmacists were able to avoid having to refer the patient to another health service in 92% of cases. In 18% of cases, having access to the SCR meant a prescribing error was avoided, says a report of the findings.
The announcement from Burt, who describes the profession as an “untapped resource in the health service”, follows a promise of £7.5m to help fund training and resources for pharmacists to help GPs in England deliver a seven-day-a-week service.
Source: Shutterstock.com
Scotland brings in medicine card to avoid AKI after dehydration
Information cards that warn patients to temporarily stop taking specific medicines if they have a dehydrating illness are being introduced across Scotland.
The roll out of ‘Medicine sick day rules’ cards follows the success of the scheme first launched in NHS Highland in 2013.
The credit card-sized cards advise patients to stop taking named medicines if they develop a dehydrating illness because they could be at risk of developing acute kidney injury (AKI).
The medicines to avoid are ACE inhibitors, anti-inflammatory painkillers, diuretics and metformin.
Since the cards were introduced in the Highlands there has been a small fall in the number of patients admitted to hospital with AKI, according to an evaluation published in April 2015. Patients followed the advice on the card and restarted their medicines within 48 hours of recovering from the dehydrating illness, it found.
A similar scheme is running in parts of Wales and the cards are being tested in Salford in an NHS England pilot.
Cystic fibrosis therapy approved by FDA
A combination therapy of two drugs that target the most common genetic mutation responsible for cystic fibrosis (CF) has been given a licence in the United States.
Vertex Pharmaceuticals’s lumacaftor 200mg/ivacaftor 125mg (Orkambi) was given breakthrough designation status by the US Food and Drug Administration (FDA), which means its approval was fast-tracked in recognition of the substantial impact it could have for patients.
The approval significantly broadens the treatment options for CF patients with specific genetic defects, says the FDA.
The product — which has orphan drug status in both Europe and the United States — is designed for patients who have the F508del mutation.
Nivolumab granted positive opinion under early access scheme
The Medicines and Healthcare products Regulatory Agency (MHRA) has given nivolumab a positive scientific opinion under its Early Access to Medicines Scheme (EAMS) as a treatment for locally advanced or metastatic squamous non-small cell lung cancer (NSCLC).
The decision means that doctors have access to benefit and risk information about the drug, a programmed death-1 immune checkpoint inhibitor, which they can choose to prescribe under their own responsibility.
The MHRA decision comes just a month after the European Medicines Agency (EMA) recommended that the drug should be granted a marketing authorisation for the same condition across Europe.
Source: Shutterstock.com
Study finds favour in self-monitoring for oral anticoagulants
People using oral blood thinning therapy such as warfarin can successfully monitor and manage their own international normalised ratio (INR) using commercially available devices, research shows.
An impressive 90% of 296 patients were still self-monitoring 12 months after buying a device, with eight adverse events reported by GPs, including two deaths, four bleeding events, a thrombosis and a transient ischaemic attack.
Two studies published in the British Journal of General Practice were based on interviews and assessments of individuals who purchased a point-of-care INR monitor (Roche’s CoaguChek) in England over a 12-month period.
In all, 45% of patients self-monitored their INR but received assistance with dose adjustment, and 40% both self-monitored and adjusted their own medication. Nearly all participants said they had used the information that came with the monitor, but only 46% had received in-person training.
Mean time in the therapeutic range (TTR), indicating optimal anticoagulation control, was 75.3%, with older age being associated with a greater TTR.

Source: Shutterstock.com
Inappropriate prescribing putting asthma patients’ lives at risk
Thousands of patients with asthma in the UK are not being prescribed the right medication to keep their condition under control, finds an audit of GP practice records by the charity Asthma UK.
The National Review of Asthma Deaths, published in May 2014, highlighted prescribing errors in nearly half of the 195 asthma deaths in primary care in 2012 and 2013. The two most common were use of long-acting reliever inhalers alone and excessive use of short-acting relievers.
To identify how often these two prescribing errors occurred in routine care, Asthma UK analysed 94,955 patient records from over 500 UK GP practices between 2010 and 2013. The results of the audit show that 5,032 patients had been prescribed more than 12 reliever inhalers over a 12-month period, 1,965 of them without being reviewed by a nurse or doctor. A further 402 patients had been prescribed long-acting reliever medicines without a corticosteroid preventer, or not as a combination inhaler.