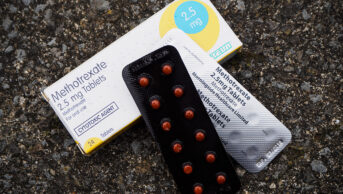
Shutterstock.com
A coroner has raised concerns about outdated methotrexate guidance and a lack of clarity around the role of community pharmacists under the Pharmacy First scheme, following the death of a patient.
In a prevention of future deaths report, published on 20 February 2026, Elizabeth Wheeler, assistant coroner for Cheshire, said there is a risk of future deaths unless action is taken, after a patient died after developing methotrexate-induced pancytopenia and pneumonia.
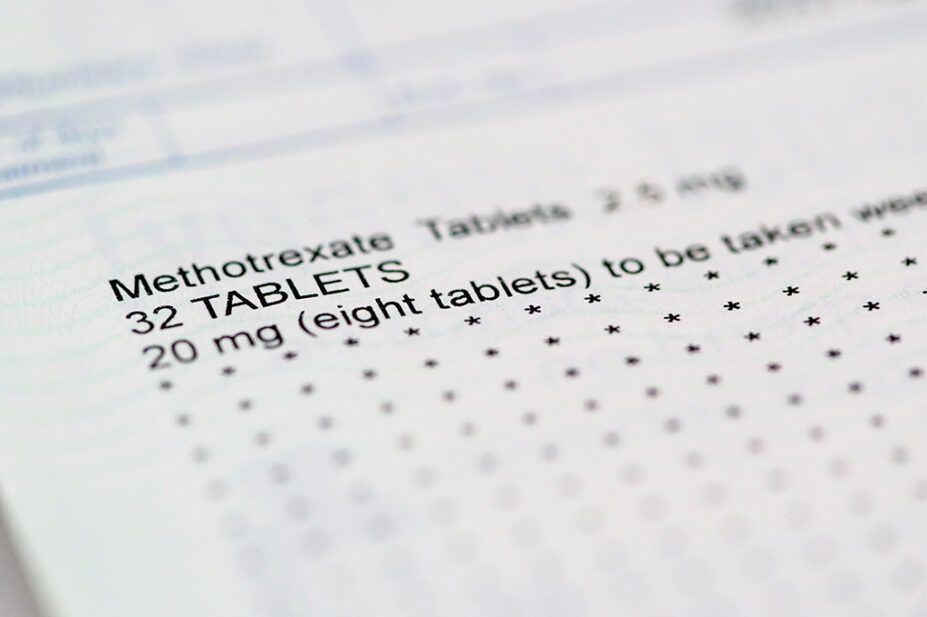
The report stated that Alan Crabtree, aged 84 years, was prescribed methotrexate on 3 February 2025 for ongoing rheumatoid issues. He then developed idiosyncratic side effects, including rapid pancytopenia and, as a result, was admitted to Macclesfield Hospital on 18 February 2025.
Crabtree died on 1 March 2025 after developing pneumonia. The inquest concluded with a finding of “misadventure”.
During the inquest into the patient’s death, the coroner explored the guidance provided to patients on what action to take if they develop signs of methotrexate toxicity, including a sore throat, mouth ulcers and difficulty swallowing, and who they should seek advice from.
This included the ‘Shared care guideline for oral methotrexate in rheumatological conditions in adults’ — produced in September 2017 by the Greater Manchester Medicines Management Group, a cross-organisational body that supports appropriate use of medicines across Greater Manchester — which was due for renewal in October 2020 but had not yet been updated at the time of going to press.
The coroner said the dose range outlined in the guidelines — 5–15mg initially, titrated to 20–25mg — “does not reflect current practice”.
The report stated that a low dose of 5mg “is not routinely prescribed” and rarely used in rheumatology as it may be sub-therapeutic.
The guideline does also not provide guidance on when doses should be adjusted or what factors support clinical decision-making.
In Crabtree’s case, the family sought advice from a community pharmacist and treatment was provided through the Pharmacy First scheme. The inquest noted the guideline’s instruction for patients to seek “medical attention” may be ambiguous because the guidance predates the introduction of Pharmacy First and the expanded role of community pharmacists.
The coroner said the guidance does not clearly state which healthcare professional patients should consult and does not reflect changes in responsibilities between secondary care, GPs and community pharmacists, potentially leading to delays in stopping methotrexate or starting treatment for toxicity.
“This is also not in line with the Arthritis UK patient information leaflet, which states patients should inform their ‘doctor or nurse specialist’ if they have signs of a sore throat and/or sores in the mouth,” the report said.
The coroner sent the report to the Greater Manchester Medicines Management Group, which must respond within 56 days, detailing any action taken or proposed with a clear timeline.
The Pharmaceutical Journal has approached Greater Manchester Medicines Management Group for comment.
In December 2025, Roz Gittins, chief pharmacy officer at the General Pharmaceutical Council, wrote to pharmacy teams to remind them to supply the methotrexate in line with a drug safety update, after the regulator received concerns that the drug had been dispensed with a label instructing a patient to take the medication once daily rather than once weekly.