Simon Webster / Alamy Stock Photo
Opioid dependence services are likely to face “serious financial pressures” in the long term after the price of one of the most common treatments they use soared for the second time in a year, public health chiefs have warned.
Public Health England (PHE) wrote to all directors of public health on 24 October 2018 telling them that although an original supply issue with buprenorphine had been resolved, supplies were still “limited” and that it was “impossible to predict” when the price of the drug would fall. PHE recommended that public health directors should immediately reflect on their budget for services going into the future.
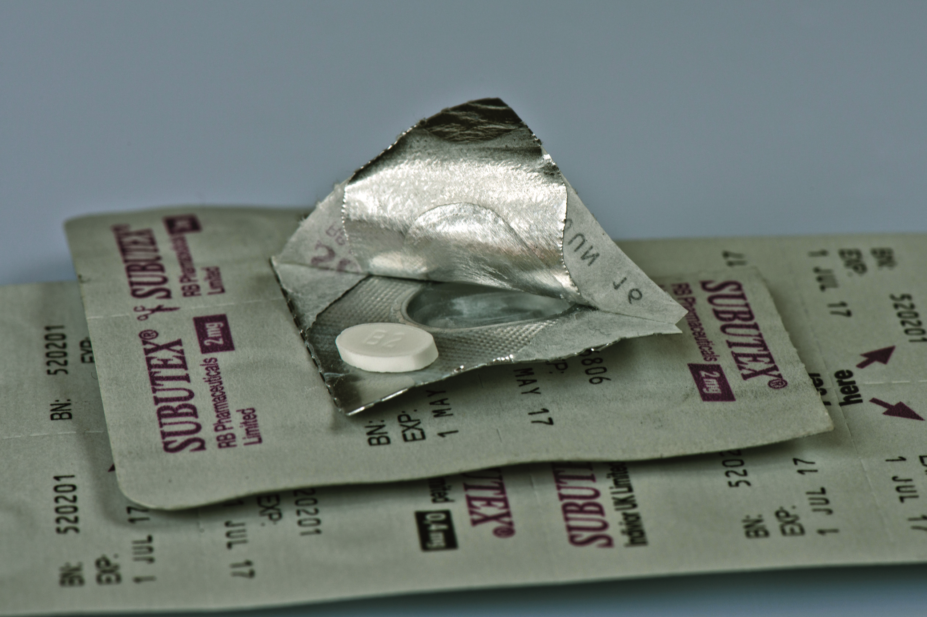
The National Institute for Health and Care Excellence recommends that oral formulations of methadone and buprenorphine are used for maintenance therapy in the management of opioid dependence, but the price of a packet of buprenorphine 8mg tablets reached £15.40 in October 2018, a 540% rise on the price of £2.38 in April 2018. Similarly, the buprenorphine 2mg tablets cost £5.25 per packet in October 2018, an almost 300% rise from £1.33 over the same period.
PHE admitted the pricing situation is putting massive pressure on local authority budgets, particularly as there is no agreed clinical guidance on which alternatives can be offered if a patient is stable on buprenorphine. It said shortages meant “pharmacists have had to rely on obtaining and supplying branded buprenorphine”.
The letter states: “These price increases mean that drug treatment services and their commissioners will see increased drugs bills for most, if not all, of 2018 and potentially beyond that. This is already creating some serious financial pressures.”
It added that the cost of buprenorphine would not likely come down in the near future. “It is impossible to predict for how long a higher concessionary price will continue to be paid. Eventually concessionary prices will no longer be required, either because the reimbursement prices listed in the Drug Tariff will catch up with the increased selling prices or because selling prices will decrease to the original level.
“Previous experience suggests that it is usually the former rather than the latter. Now and looking to the future, local authorities may need to reflect on the medicines element in their budgets for drug treatment.”
In October 2018, a
response to a question in the House of Commons about the supply shortages prompted health minister Steve Brine to assure that prices would level out in a matter of weeks. “The market for buprenorphine has generally been competitive and we expect the supply situation to improve over the coming weeks, which is likely to result in an increasingly competitive market,” he said.
But Lord Adebowale, chief executive of the health and social care organisation Turning Point, which provides opioid dependence services, said that this had not happened and the high drug price has “severely affected the operations of substance misuse providers”.
He added: “Our conversations with a range of national bodies have not provided us with robust assurance that this is a short-term problem, although we note that the original predictions for this issue being resolved by the end of October 2018 have not come to fruition.
“With price rises of over 700% [on the drug tariff price] in some months, this is clearly not sustainable for any provider and decisions, made with all clinical considerations, have to be made as a consequence.”
A spokesperson for the Department of Health and Social Care said it had been working closely with suppliers of buprenorphine to mitigate any supply issue. “As the supply situation of buprenorphine improves, we expect to see an increasingly competitive market with prices going down,” they said.
“However, the level and the speed of price decrease will depend on the level of competitiveness in the market. We will continue to monitor the situation closely.”