Shutterstock.com
Testing individuals with any risk factor for the hepatitis C virus (HCV) is more cost effective than restricting screening to people with a history of injecting drugs, a study based in the Isle of Wight has found.
Overall, the cost of targeted testing for hepatitis C in community pharmacies was found to fall below “willingness to pay” thresholds used by the National Institute for Health and Care Excellence (NICE), the study’s authors concluded.
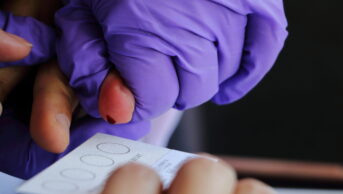
Dry blood spot testing for HCV took place between September 2014 and September 2016 in 20 community pharmacies in the Isle of Wight. Over the two-year period, 186 tests were carried out and the intervention identified 13 new cases of HCV in people disclosing a range of risk factors for HCV. Six of these cases went on to achieve an effective cure for HCV during the study period.
The researchers calculated that the total cost of the intervention was £242,183, which broke down as £56.88 for each individual tested, £755.54 for everyone undergoing further investigations following a positive test for HCV antibody, and £36,964 per person treated (assuming directly acting antiviral therapy was available at list prices).
When compared with a control population, the intervention incurred additional healthcare costs. However, when this was considered against the associated gain in quality of life, the incremental cost-effectiveness ratio was £3,689 per quality adjusted life year (QALY) gained – well below the NICE willingness to pay threshold of £20,000 per QALY.
When compared with their respective control populations, targeted testing in anyone with a risk factor for HCV led consistently to a greater gain in QALYs than if testing had been restricted to people disclosing a history of injecting drug use, the study found.
The introduction of a HCV testing service — to be funded for at least two years from 2019/2020 — for individuals using needle and syringe programmes in community pharmacy was announced in the ‘Community pharmacy contractual framework’ in July 2019.
Ryan Buchanan, an academic clinical lecturer in hepatology at the University of Southampton and lead author on the study, welcomed the plan but told The Pharmaceutical Journal that offering the service just to those using needle and syringe programmes was “missing a trick”.
“On the Isle of Wight we made HCV testing available to everyone with a risk factor, including [individuals who may have had] medical treatment in high risk areas,” he said.
“Community pharmacy [could be] tremendously powerful in terms of eliminating HCV. It is accessed by very at-risk individuals but is also a walk-in service for people who, for example, might have injected years ago.”
You may also be interested in
Genomics surveillance programme for hepatitis C launched by UK Health Security Agency

How we treated more than 100 hepatitis C patients at pharmacist-led clinics in North Wales