Phanie / Alamy Stock Photo
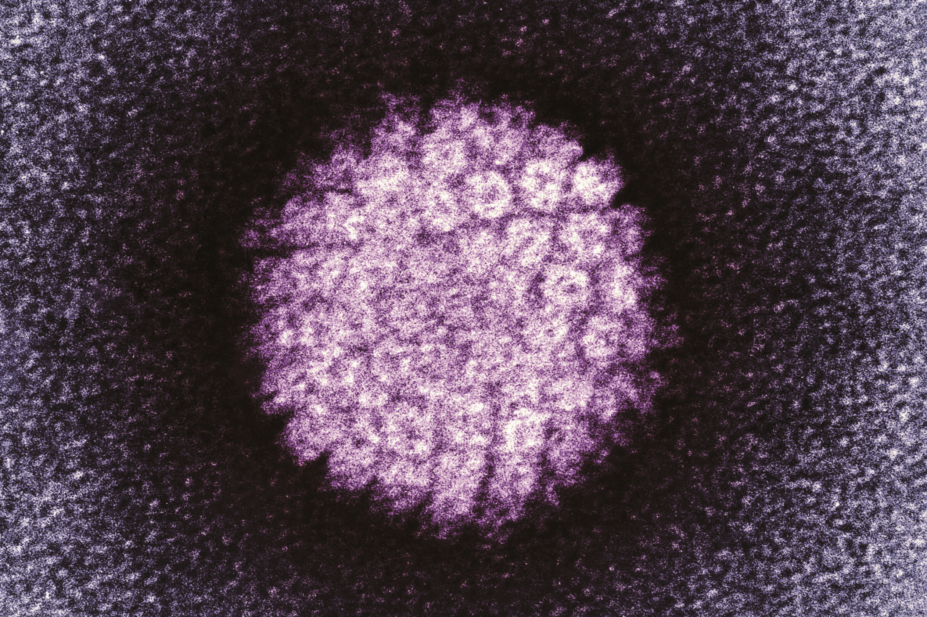
Women with high-risk human papillomavirus (HPV) infection are more likely to develop cardiovascular disease (CVD) than those without, the results of a study published in Circulation Research suggest (7 February 2019)[1]
.
Researchers looked at data from 63,411 healthy Korean women aged 30 years and over who were tested for HPV and followed-up every one or two years between 2011 and 2016. In total, 7.6% had high-risk HPV infection when first tested, with 1,122 new cases of CVD detected during follow-up.
Overall, after adjustment for confounding factors, the analysis revealed that the risk of CVD was 25% higher in those with high-risk HPV infection compared with those without HPV.
The authors found that the association between high-risk HPV and CVD was stronger in obese individuals than non-obese; the adjusted risk of CVD was 73% in obese participants with HPV compared with 10% in non-obese participants with HPV. A similar pattern was found in those with metabolic syndrome compared with those without.
The researchers said the findings suggested that high-risk HPV infection may act additively or synergistically with obesity and metabolic syndrome to increase cardiovascular disease risk, potentially related to effects on inflammation.
The authors concluded: “Further studies are required to identify the specific high-risk HPV genotypes that may contribute to CVD and implement vaccine strategies as a modifiable risk factor for the reduction of CVD, in addition to prevention of anogenital cancers.”
References
[1] Joo E-J, Chang Y, Kwon M-J et al. High-risk human papillomavirus infection and the risk of cardiovascular disease in Korean women: a cohort study. Circ Res 2019;124(5):747–756. doi: 10.1161/CIRCRESAHA.118.313779