Science Photo Library
Open access article
The Royal Pharmaceutical Society has made this article free to access in order to help healthcare professionals stay informed about an issue of national importance.
To learn more about coronavirus, please visit: https://www.rpharms.com/resources/pharmacy-guides/wuhan-novel-coronavirus
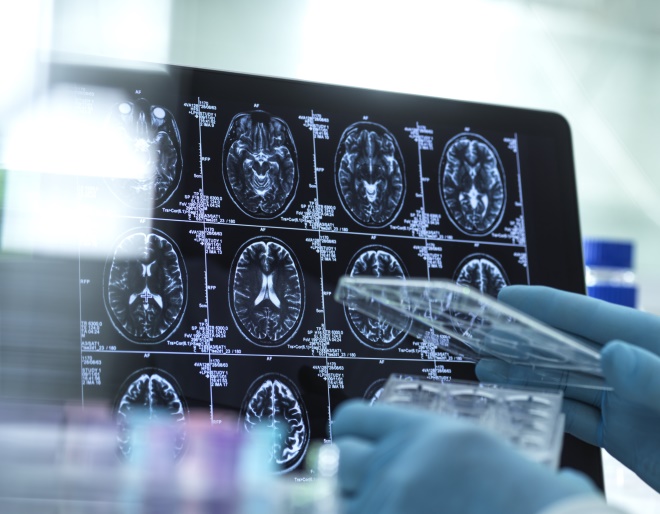
Source: Science Photo Library
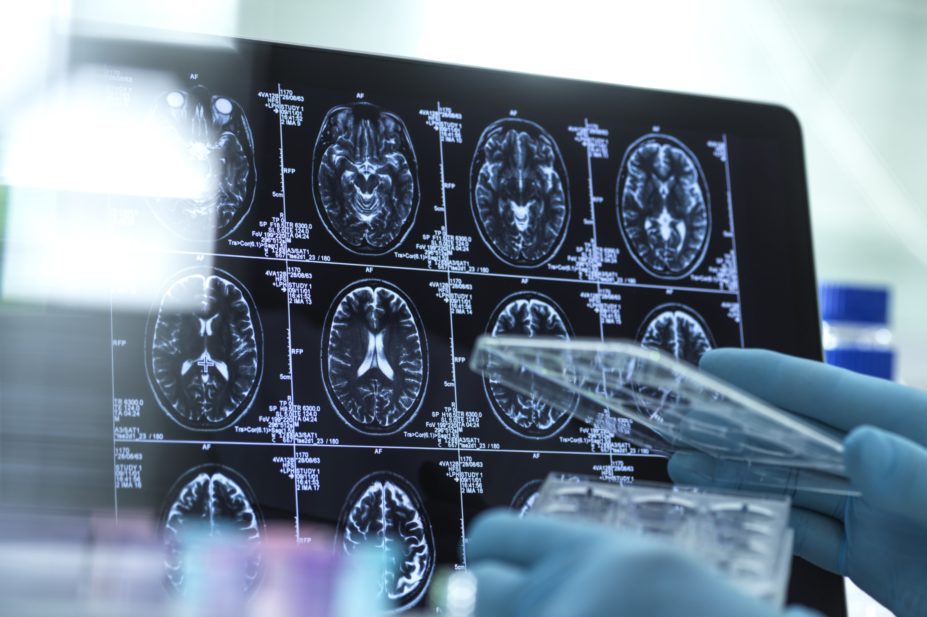
Patients with COVID-19 commonly experience neurological conditions, such as dizziness, headache, and impaired taste and smell
Neurological symptoms are common in patients with COVID-19, particularly if they have a severe infection, research published in JAMA Neurology suggests (10 April 2020)[1]
.
The team used data on 214 patients with confirmed COVID-19 treated at one of three specialist care centres in Wuhan, China, between 16 January 2020 and 19 February 2020.
Overall, 78 patients (36.4%) had neurological manifestations, involving the central nervous system (e.g. dizziness, headache, impaired consciousness), peripheral nervous system (e.g. taste, smell or vision impairment, and nerve pain), or skeletal muscles. Among the 88 patients with severe infection, neurological symptoms were significantly more common than in those with non-severe infection (45.5% vs. 30.2%). They included acute cerebrovascular disease, impaired consciousness and skeletal muscle injury.
The team said that the findings suggested that COVID-19 could affect the nervous system as well as the respiratory system, and that the receptor for the SARS-CoV-2 virus, ACE2, is expressed in neural and skeletal tissues. They noted that in some patients, their only symptoms were neurological in nature.
“During the epidemic period of COVID-19, when seeing patients with these neurologic manifestations, physicians should consider SARS-CoV-2 infection as a differential diagnosis to avoid delayed diagnosis or misdiagnosis and prevention of transmission,” the authors concluded.
References
[1] Mao L, Jin H, Wang M et al. JAMA Neurol 2020. doi: 10.1001/jamaneurol.2020.1127