Science Photo Library
The NHS Health Check programme is an effective way of identifying patients who would benefit from statins, and those who attend a health check are more likely to begin treatment with statins, according to a study published in the British Journal of General Practice.
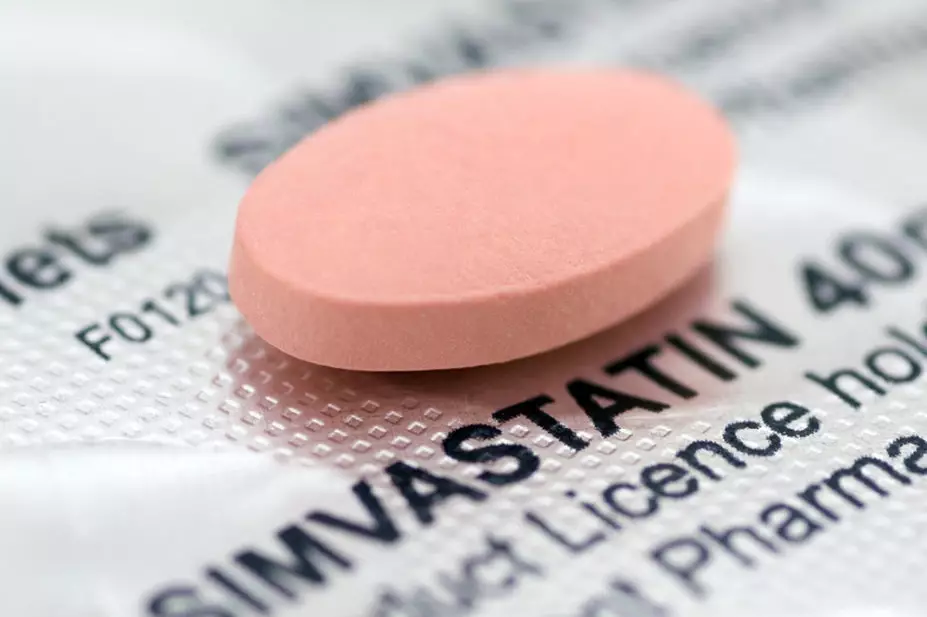
The study, published on 15 June 2021, said that, of eligible patients who attended a health check, 26 in every 1000 were prescribed statins, compared to 8 in every 1,000 of those who did not attend.
However, the same study showed that 91% of attendees eligible for statins were not prescribed them in the 12 months following the check.
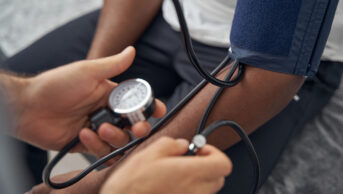
The study found that a new diagnosis of hypertension was made in 25 in 1,000 attendees (1 in 40), compared to 9 in 1,000 for non-attendees). Type 2 diabetes was found in 8 in 1,000 attendees, compared to 3 in 1,000 non-attendees, and non-diabetic hyperglycaemia was identified in 4 in 1,000 attendees, compared to 1 in 1,000 non-attendees.
The study looked at eligible NHS Health Check attendees between 1 April 2013 and 31 March 2017. The authors noted that uptake of the heath check was low, with just 16.9% of eligible people taking up the opportunity.
The authors, from the University of London, University of Oxford and University of Nottingham, said that there is “a policy decision to be made about whether it is more effective to improve persistently low attendance or target those at increased CVD [cardiovascular disease] risk”. They noted that half of attendees are aged 50 years or younger and at low CVD risk. More targeted approaches could “improve effectiveness and cost effectiveness”, the authors added, noting that the increased shift to online engagement could “free up resources to improve targeting of people at higher CVD risk”.
Paul Wright, lead cardiac pharmacist at Barts Health NHS Trust, said that while the paper reported a low uptake in health checks from 2013–2017, “it should be noted that this was a significant increase from the previous five years where only 8.9% attended”.
Wright also said that while it was “surprising to see that prescriptions for statins in those with CVD risk of >10% was only noted in a relatively small proportion of those deemed eligible” in the 12-month period following the health check, this figure was still “three times more likely than in those that did not attend”.
He added that study found a “marked variation in equity of attendance, with it being more likely in South Asian and less likely in black African, black Caribbean, and Chinese ethnic groups than white ethnic groups, and lower in males compared to females”.
“In order for schemes such as the NHS Health Checks to deliver, further work is required to understand barriers to attendance and focus resources on selected populations with higher baseline cardiovascular risk,” he said.
The study is also the first to report increased diagnosis of atrial fibrillation (AF) and dementia through the NHS Health Check, the authors said. AF was observed in 5 in 1000 attendees, and 3 in 1000 non-attendees; dementia was diagnosed in 2 in 1,000 attendees and 1 in 1,000 non-attendees.