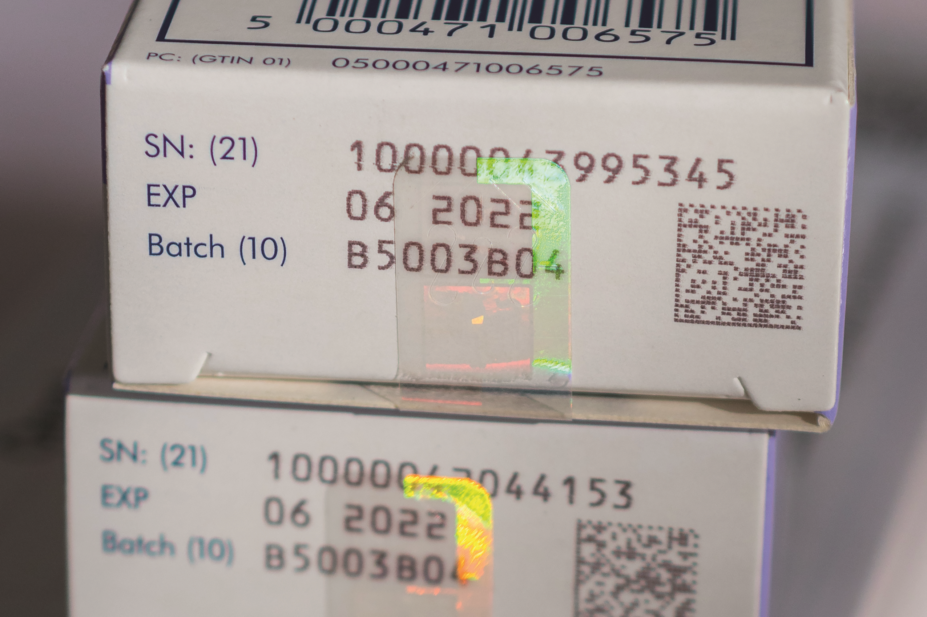
Courtesy of Jonathan Buisson
Proposals for a no-deal Brexit put forward by the Medicines and Healthcare products Regulatory Agency (MHRA) would put patients in the EU at risk, the Association of the British Pharmaceutical Industry (ABPI) and the UK Bioindustry Association (BIA) have said.
In a joint response to the MHRA’s consultation on contingency plans for the regulation of medicines and medical devices in case of a no-deal Brexit, published on 1 November 2018 to coincide with the closing of the consultation, the two bodies also warned that the plans could increase the risk of falsified medicines entering the UK.
A no-deal Brexit is likely to see the UK’s access to EU databases revoked — including the European Medicines Verification System (EMVS), the heart of EU-wide compliance to the Falsified Medicines Directive (FMD).
The EMVS is a central EU database that will store details of FMD-compliant medicine packs. If access is revoked under no-deal terms, UK pharmacists and suppliers will be unable to decommission medicines when they are dispensed.
The MHRA has therefore proposed that the legal requirement to decommission medicines would be removed in the UK, along with the requirement to verify the authenticity of packs. But the ABPI and BIA warn that this would “introduce a security risk to all other national systems”: if a pack is not decommissioned, the EMVS will be unaware that it has been dispensed, and its details could be duplicated on a falsified pack.
The proposals present a risk to UK patients too, as unilaterally revoking FMD legislation in the UK would make the country a target for counterfeiters, the two bodies say.
The ABPI and BIA also warn that the UK’s national medicines verification database may become “entirely redundant” if implementation of FMD ‘safety features’ legislation is revoked in the UK. In such a scenario, they say, financial compensation should be given to marketing authorisation holders, manufacturers and other stakeholders for the “significant time and investment” they have already contributed to the system.


