Science Photo Library
Open access article
The Royal Pharmaceutical Society has made this article free to access in order to help healthcare professionals stay informed about an issue of national importance.
To learn more about coronavirus, please visit: https://www.rpharms.com/resources/pharmacy-guides/wuhan-novel-coronavirus
Source: Science Photo Library
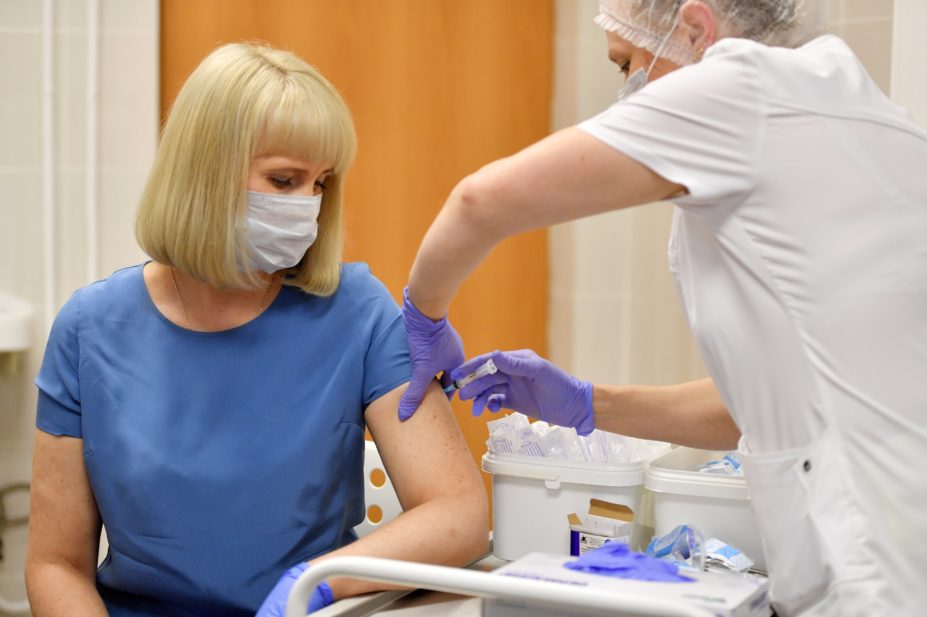
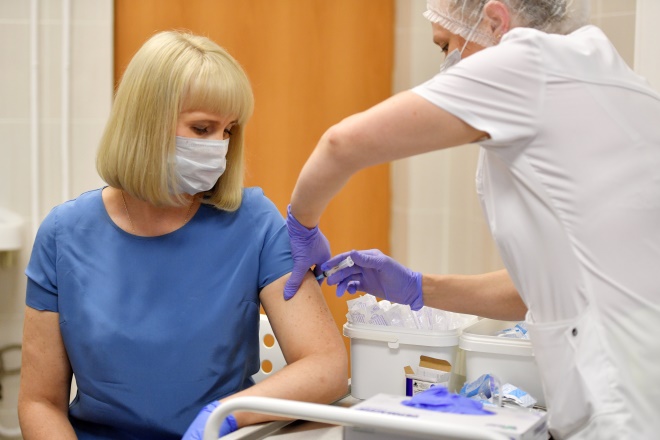
The regulator also advised that vaccine recipients should now be monitored for 15 minutes after vaccination
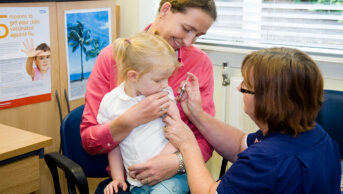
Patients with a history of anaphylaxis to a vaccine, medicine or food should not receive the Pfizer/BioNTech vaccine for COVID-19, the Medicines and Healthcare products Regulatory Agency (MHRA) has said.
Vaccine recipients should also now be monitored for 15 minutes after vaccination, according to revised advice from the regulator.
Healthcare professionals administering the vaccines in hospital hubs and vaccination centres had previously been told that observation would only be required if the patient was driving.
June Raine, chief executive of the MHRA, said that the regulator had decided to issue the revised advice after “two reports of anaphylaxis and one report of a possible allergic reaction following immunisation”.
The reports were reviewed by an expert group of the Commission on Human Medicines (CHM), attended by experts in allergy and clinical immunology.
Raine said in a statement that patients should not be given a second dose if they have experienced “anaphylaxis following administration of the first dose of this vaccine”.
“Anaphylaxis is a known, although very rare, side effect with any vaccine. Most people will not get anaphylaxis and the benefits in protecting people against COVID-19 outweigh the risks,” she said.
“We have in place a robust and proactive safety monitoring strategy for COVID-19 vaccines which allows for rapid, real-time safety monitoring at population level,” Raine continued. “The fact that these incidents were picked up and reviewed shows that to be the case.”
Raine told the House of Commons Health and Social Care Select Committee earlier, on 9 December 2020, that the MHRA was “looking at two case reports of allergic reactions — we know from the very extensive clinical trials that this wasn’t a feature”.
According to trial data provided by Pfizer and published by the US Food and Drug Administration, only one incident of anaphylactic reaction had occurred between the first dose of the vaccine and one month after the second dose in phase 2/3 of the trial.
In total, 18,801 people were administered the vaccine as part of phase 2/3 of the trial.
Fifty hospital hubs began administering the vaccine on 8 December 2020, with ‘wave 1’ of primary care network-led vaccination services expected to start vaccinations on 15 and 16 December 2020.