Courtesy Pharmacy Voice

Source: Courtesy Pharmacy Voice
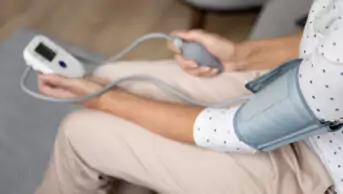
Rob Darracott, chief executive officer, Pharmacy Voice, says one of the intentions behind the report is to start getting people to talk about whether we could do better in terms of monitoring blood pressure treatment
Community pharmacies in England can enhance the ‘huge volume of work’ they do in the management of hypertension, according to a report by the community pharmacy representative body Pharmacy Voice.
The report, which is backed by Public Health England (PHE), was launched on 27 February 2017 and sets out 12 recommendations, including the extension of community pharmacy blood pressure (BP) services and the introduction of measures that will help embed and sustain the commissioning of public health services to tackle high BP.
Rob Darracott, chief executive officer of Pharmacy Voice, an association of three community pharmacy trade bodies, told The Pharmaceutical Journal at a meeting in London where the report was launched that it was not recommending that a new hypertension management service be introduced.
“There are already lots of pharmacists that offer a blood pressure service,” said Darracott. Instead, Pharmacy Voice is highlighting what pharmacy does “to other parts of the system”, he said.
The intention behind the report was also to “start getting people to talk about whether we could do better in terms of monitoring treatment”.
Pharmacists should be allowed access to patient records in order to make direct referrals to GPs and other healthcare professionals as necessary as part of the move to increase their role in blood pressure services, the report recommends. Better coordination between GPs and community pharmacists around the support and advice offered to patients taking antihypertensive medicines was also crucial, it says.
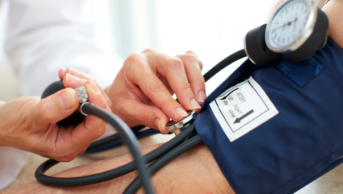
The report also recommends that every community pharmacy should have an approved blood pressure monitoring machine, with staff trained to screen customers. And more community pharmacies should be contracted to deliver the existing NHS health-checks service – which includes hypertension screening; currently only 30% of pharmacies offer the checks, the report points out.
Kevin Fenton, director of health and wellbeing at PHE, who is leaving his post shortly, told the meeting that he was an advocate of pharmacy, but that the sector could not continue to rely on serendipity. “You are not an afterthought but a core part of [public health],” he said.
“Now the report is out, move to activation and make it a live and productive document,” he said. But he warned that there is less money available and a need to provide more public health activities.

Source: Courtesy Pharmacy Voice
Elizabeth Wade, director of policy and communications at Pharmacy Voice, says there is still a lack of integration between community pharmacy and GP practices
Elizabeth Wade, director of policy and communications at Pharmacy Voice, says the report “consolidates our thinking on BP”. She said that a huge volume of work was being done on BP in community pharmacy but there was a lack of integration between community pharmacy and GP practices and that more integrated commissioning, integrated care pathways and integrated IT systems were needed.
Matt Kearney, national clinical director for cardiovascular disease prevention at NHS England, says he is “encouraged by the ambition shown in this report”. “I look forward to seeing the recommendations from this report implemented,” he adds.
Responding to the report, Sandra Gidley, chair of the Royal Pharmaceutical Society’s English Pharmacy Board, says: “Local commissioners can create better patient outcomes through inclusion of community pharmacies within their primary care strategy as a centre for health promotion and diagnostics alongside medicines advice.”
The report was also welcomed by Sotiris Antoniou, consultant pharmacist in cardiovascular medicine at Barts Health NHS Trust.
He says: “Patients often visit the same community pharmacy for repeat medicines or prescriptions so the pharmacists would be able to support the on-going review to optimise their blood pressure medicines.
This accessibility and ability to reach a population, often missed within the traditional pathways, makes community pharmacy an integral partner in improving public health.”
The report highlights examples from across England where community pharmacies are already taking a lead in delivering hypertension services. The high street chains Lloydsphamacy and Rowlands have established free blood pressure monitoring services while the Healthy Living Pharmacy model is ideally placed to take a key role in the care of patients with hypertension, the report says.
“As a profession, we need to work collaboratively across the traditional boundaries and ensure our findings are published in peer-review journals to ensure the good work can be applied more consistently nationally,” says Antoniou. “This report, I hope, is just the start of making this happen.”
The report is the community pharmacy sector’s response to the 2014 report by the National Blood Pressure Systems Leadership Board, which outlined how the prevention, early detection and management of blood pressure could be improved in England. Pharmacy Voice is a member of that board.
It is estimated that six out of 10 cases of high blood pressure remain undiagnosed while hypertension services cost the NHS in England around £2.7bn a year.