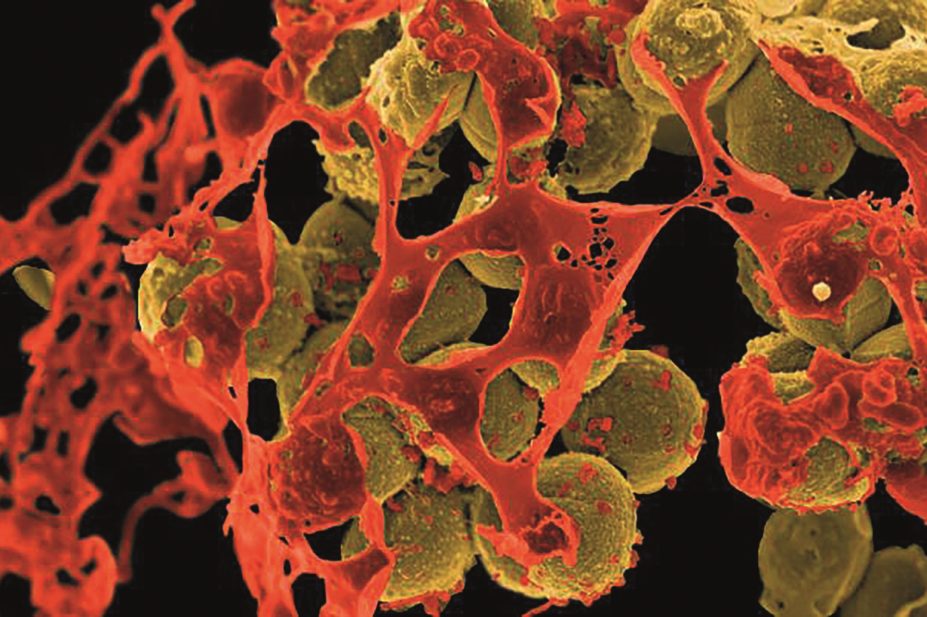
BSIP SA / Alamy
Researchers using an innovative process that employs bacteria grown in soil rather than cultured under laboratory conditions have discovered a new antibiotic with properties that appear to prevent the development of resistance.
The research team — which includes investigators from Northeastern University in Boston, Massachusetts, the University of Bonn in Germany and NovoBiotic Pharmaceuticals based in Cambridge, Massachusetts — identified the compound, known as teixobactin, after screening 10,000 different isolates for antimicrobial activity.
The discovery, reported in Nature on 7 January 2015[1]
, could help address one of the most challenging problems facing global health systems: the diminishing number of effective compounds for treating pathogens that are already resistant to many existing therapies.
“This is a promising source in general for antibiotics and has a good chance of helping to revive the field of antibiotic discovery,” Kim Lewis, a professor of biochemistry and director of Northeastern’s Antimicrobial Discovery Center told a telephone press briefing.
Teixobactin works against microbes by inhibiting cell wall biosynthesis, explained co-author Tanja Schneider from the University of Bonn. By simultaneously binding to multiple, highly conserved cell building blocks — including lipid II molecules, which Schneider described as the “Achilles heel for antibiotic attack” — the compound disrupts the entire cell building cycle. Teixobactin targets Gram-positive organisms without protective membranes, and its distinctive properties help explain both its effectiveness and the fact that it appears to be unreceptive to bacterial mutation.
“The straightforward way for bacteria to develop resistance is by mutation, but the targets of teixobactin are not proteins so there is nothing to mutate,” Lewis said.
Schneider added that the energy required for a cell to modify this process makes it unlikely that resistance would develop in this way.
Screening of soil microorganisms that can be cultivated, a process that peaked in the early 1960s, produced most antibiotics currently in use. Since then, synthetic approaches to producing antibiotics have been much less successful.
The research team discovered teixobactin through the use of an innovative platform developed in the Northeastern lab. The platform consists of mini-diffusion chambers, each of which contains a single bacterial cell, soil and an overlay of two semi-permeable membranes. The process allows researchers to isolate and grow bacteria in their natural environment.
The team has developed 25 compounds using the technique and, although most did not meet validation criteria due to poor solubility, instability or “substantial toxicity”, the researchers are looking at three other potentially interesting antibiotics. One, lassomycin[2]
, shows promise in treating multi-drug resistant tuberculosis and two unnamed compounds are being tested as potential anti-cancer agents, Lewis said.
Teixobactin has been tested in mice models and is “exquisitely active” against Gram-positive pathogens, including drug-resistant strains of Meticillin-resistant Staphylococcus aureus, enterococci and tuberculosis, Lewis said. The compound is also effective against Clostridium difficile and Bacillus anthracus. In the case of S aureus, teixobactin was more efficient than vancomycin, an antibiotic with similar properties for which resistance did not develop for nearly 40 years. The researchers said they expect it would take a similar period of time for any resistance to teixobactin to develop.
The researchers are conducting additional testing of teixobactin to improve its pharmacological properties, including efforts to increase the compound’s solubility and enable it to be delivered at a higher therapeutic dose, Lewis said. He added that it should be possible to begin clinical trials of teixobactin within two years.
References
[1] Ling LL, Schneider T, Peoples AJ et al. A new antibiotic kills pathogens without detectable resistance. Nature 2015. doi:10.1038/nature14098.
[2] Gavrish E, Sit CS, Cao S et al. Lassomycin, a ribosomally synthesized cyclic peptide, kills mycobacterium tuberculosis by targeting the ATP-dependent protease ClpC1P1P2. Chemistry & Biology 2014. doi:10.1016/j.chembiol.2014.01.014.