Shutterstock.com
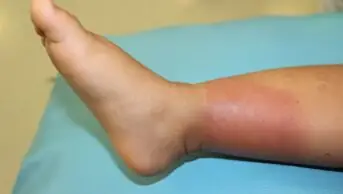
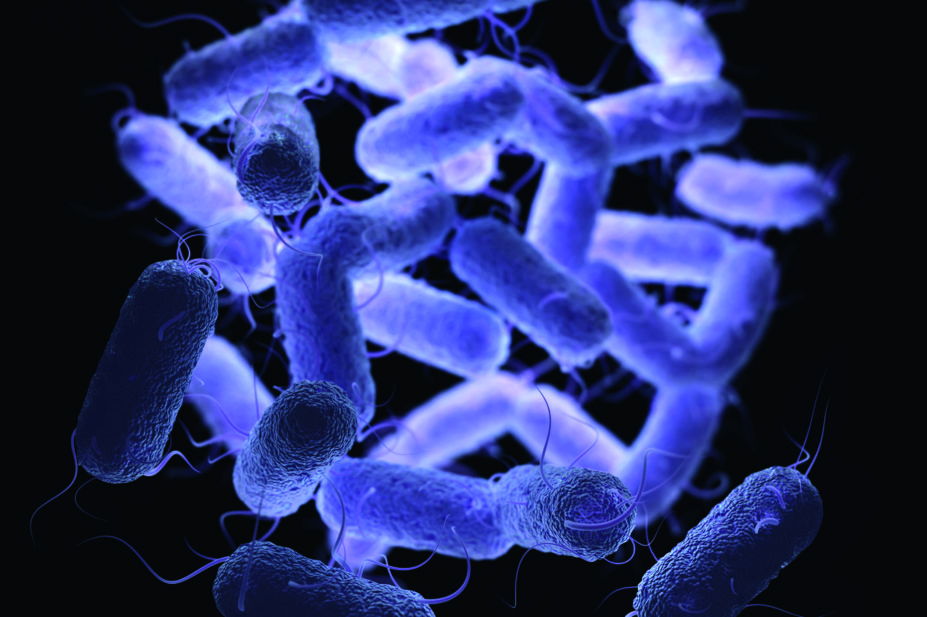
People who have been exposed to Enterobacteriaceae (EPE), a family of drug-resistant bacteria, are known to have an increased risk of subsequent sepsis. However, little is known about how this risk changes over time.
Swedish researchers analysed national data to compare 22,702 individuals who had documented EPE in their faeces or urine with a control cohort with no known EPE exposure.
Over a maximum follow-up of six years, people were 57 (hazard ratio [HR] 57.43, 95% confidence interval [CI] 17.41–189.42) and 113 (HR 113.11, 95% CI 35.93–356.10) times more likely to develop an EPE bloodstream infection when EPE was detected in the faeces and urine, respectively, compared with controls. The risk declined exponentially in the first six months after EPE detection, but was still elevated after three years.
The researchers, who presented their findings at the European Congress of Clinical Microbiology and Infectious Diseases in Vienna[1]
, say they could help doctors diagnose drug-resistant sepsis and inform antibiotic selection.
References
[1] Isendahl J, Giske CG, Tegmark-Wisell K et al. Temporal dynamics and risk factors for bloodstream infection with extended spectrum beta-lactamase producing bacteria in previously colonized patients: nationwide register-based study. Presented at: European Congress of Clinical Microbiology and Infectious Diseases; 22-25 April 2017; Vienna. Abstract available here