Alamy Stock Photo
Scotland’s first heroin-assisted treatment service has launched in Glasgow city centre. But a pharmacist involved in designing the service has said a drug consumption room is ”urgently needed” to run alongside it.
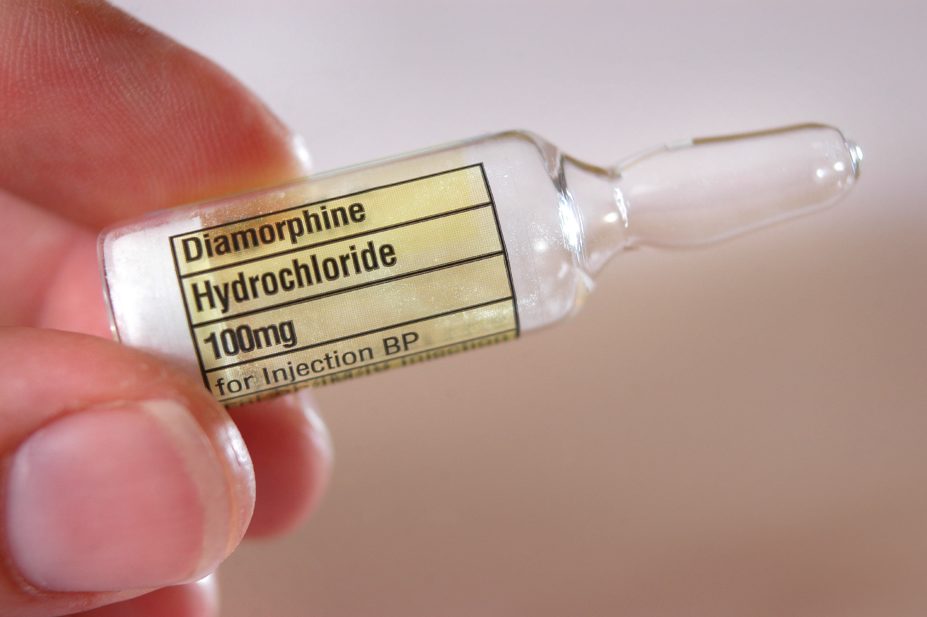
The Enhanced Drug Treatment Service (EDTR), which is licensed by the Home Office, will provide diamorphine to patients with heroin addiction who have not responded to other forms of treatment.
Patients are currently being recruited to the service, which is expected to be fully operational by the end of December 2019. Patients will administer the drug themselves, on-site, under supervision from clinical staff, and must commit to attending the clinic twice a day, seven days a week. Up to 50 patients will be able to use the service at any one time.
In addition to receiving diamorphine, service users will be offered addiction counselling and support with social welfare issues including housing and benefits advice.
Scotland has the highest level of drug-related deaths in the EU, and the nation’s drug-related death rate per head of population is almost three times that of the UK as a whole. Recent data from National Records for Scotland show that in 2018, 1,187 drug-related deaths were recorded in the country. A third of those deaths (33%) were in the Greater Glasgow & Clyde NHS Board area.
Carole Hunter, lead pharmacist in addiction services at NHS Greater Glasgow and Clyde, was involved in designing the service.
She said pharmacists had a “a key role in the development of the service”, and were “an essential part of the Enhanced Drug Treatment staff”. Stuart Notman, advanced pharmacist in addictions at NHS Greater Glasgow and Clyde, is the service’s implementation manager, and the EDTR’s staff includes pharmacists Regina O’Hara and Roddy Duncan, alongside two pharmacy support staff.
Hunter said the original plan, based on recommendations in ‘Taking Back the Chaos: the health needs of people who inject drugs in public spaces in Glasgow city centre’, published in 2016 by NHS Greater Glasgow and Clyde, was for “a co-located drug consumption room and a heroin-assisted treatment service housed in the same building”. However, to date Home Office permission for a drug consumption room has not been granted.
“A drug consumption facility offers a safe injecting space for hundreds of people on a daily basis. This facility is still urgently required in Glasgow and we will continue to pursue the evidence-based case to lobby for the necessary legal permissions or changes to enable this to be piloted in Glasgow,” Hunter said.
“One element on its own is not sufficient to address all of the drug related harms experienced by this population. A comprehensive harm reduction approach that includes the full range of harm reduction interventions, including a drug consumption room, is required”.
Catriona Matheson, chair of the Scottish Drug Deaths Taskforce, said she was “very supportive” of the Glasgow EDTR, and would support similar services elsewhere if there was considered to be sufficient need.
“As numbers are small in this one clinic, it will not have a significant impact given the scale of the problem we have in Scotland — but there is potential for considerable reduction of harm to the individuals involved”, Matheson said, adding “An evaluation is taking place and we await the findings with interest.”
“However, the evidence for heroin assisted treatment is already strong. So I do not think it is necessary to wait for these findings before starting to assess the need for similar services elsewhere,” she said.