Shutterstock / sfam_photo
Specialist critical care pharmacists can make a “substantial” contribution to resolving medication errors and helping achieve the best use of medicines for patients cared for in hospital critical care units, according to the results of the first study of its kind in the UK, published in the Journal of Critical Care
[1]
(2015;30:808–813).
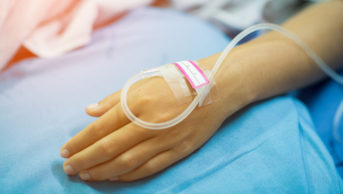
Researchers found that specialist critical care pharmacists frequently intervene in the care of their patients, who are particularly vulnerable to medicines’ side effects, and that their actions had a “high” impact in up to 24% of cases; in 0.5% of cases their advice had the potential to save a life.
Researchers analysed the contribution of pharmacists to the care of patients at 21 adult critical care units over 14 days in November 2012 — the first UK multi-centre study that has looked at the specific contribution of clinical pharmacists and the care of critically ill patients.
Rob Shulman, one of the researchers and lead critical care pharmacist at University College London Hospital, says the findings are particularly significant because most of the centres provided a five-day-a-week pharmacy service with only skeletal pharmacist cover at weekends.
“There was a spike in the number of pharmacist interventions that occurred on a Monday,” says Shulman, adding that the study’s findings support the introduction of a seven-day-a-week pharmacy service in critical care.
Pharmacists at the 21 units made 3,294 interventions in the 14-day period, including reviews of 20,517 prescriptions.
Some 6.8% of the interventions were linked to medication errors, 8.3% related to medicines optimisation, whereby the pharmacist made a proactive contribution to enhance patient care, and in 1% of cases the pharmacist was consulted by another clinician for professional advice.
Pharmacists were asked to classify the impact of their intervention as high, moderate or low.
Some 19.0% of medication error interventions were ranked as having a “high” impact and 42.6% “moderate”. The figures were similar for cases involving medicines optimisation — 19.0% were ranked “high” and 48.3% were classified as “moderate”.
In cases where the pharmacist was consulted by another professional, the impact of the intervention was ranked as “high” in 24.0% of cases and “moderate” in 60.6% of cases. In 0.5% of cases the advice was potentially life-saving, the researchers report.
“Overall, clinical pharmacists made interventions in almost one (16.1% of prescribed items) in six prescribed medications; and more than 60% of the interventions were of at least moderate impact.”
The researchers say their study shows the “high frequency and clinical importance of medication interventions made by clinical pharmacists”.
References
[1] Shulman R, McKenzie C.A, Landa J et al. Pharmacist’s review and outcomes: Treatment-enhancing contributions tallied, evaluated, and documented (PROTECTED-UK). Journal of Critical Care 2015;30:808–813. doi:http://dx.doi.org/10.1016/j.jcrc.2015.04.008.