shutterstock.com
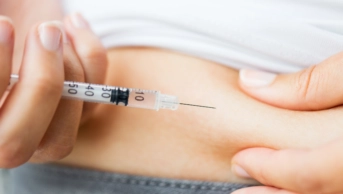
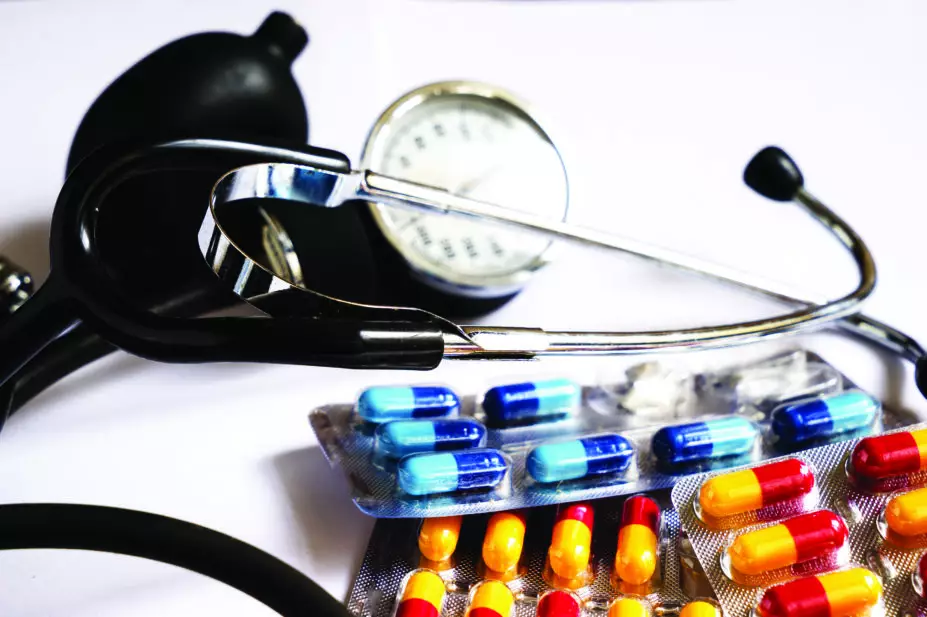
Non-adherence to antihypertensive treatment is common in the United Kingdom and Czech Republic, according to a new study.
Researchers analysed urine samples from 1,400 patients to reveal whether they were taking their antihypertensive drugs as prescribed, and found that non-adherence for UK patients was 41.6% and 31.5% in the Czech Republic cohort.
They also found that non-adherence was linked to the number of hypertensive medicines prescribed. Non-adherence risk increased by 85% with each additional drug in the UK cohort and by 77% in Czech Republic patients (P <0.001).
Writing in the latest edition of the journal Hypertension
[1]
(June 2017), they say: “Although non-adherence among those who were prescribed only one antihypertensive was minimal, the majority (79.3%) of UK patients prescribed ≥6 BP-lowering medications were non-adherent to antihypertensive treatment.”
They also discovered that 14.5% of the UK patients took none of their prescribed medicines compared to 12% of the Czech Republic patients.
In the 676 UK-patient cohort the rates of any, partial, and total non-adherence were 41.6%, 27.1%, and 14.5%, respectively. And out of the 2,562 drugs prescribed to them 815 (31.8%) were not detected in the urine sample.
The prevalence of any, partial, and total non-adherence was 31.5%, 19.5%, and 12.1%, respectively, among the 672 Czech Republic patients. The overall percentage of prescribed antihypertensive medications undetected was 24.1%.
Younger patients and women were more likely not to take their hypertensive medications compared to any other groups of patients, they found.
The findings were based on the results of urine samples at the National Centre for Adherence Testing (NCAT) established by the University Hospitals of Leicester.
The researchers say their data reveal a widespread prevalence of non-adherence, irrespective of the country or region of recruitment.
“We show that both the number and the class of prescribed antihypertensives are strong independent risk factors for biochemically confirmed non-adherence to antihypertensive treatment.”
They add: “Further development of discriminatory models incorporating these parameters might prove clinically useful in assessment of non-adherence in countries where biochemical analysis is unavailable.”
Prashanth Patel, lead researcher, told The Pharmaceutical Journal that he thinks the urine test is too technical to be routinely offered by community pharmacists and is also expensive — the equipment costs around £500,000.
He also thinks that the cost of prescriptions might be a factor in non-adherence, because costs go up each time a UK patient is prescribed another hypertensive drug.
Commenting on the study, Sotiris Antoniou, consultant pharmacist, cardiovascular medicine at Barts Health NHS Trust, says that the use of a urine test to assess adherence is becoming more widespread in clinical practice especially for patients taking multiple drugs for uncontrolled blood pressure.
He says: “The study findings, like others, show that the number of medications prescribed is inversely proportional to adherence. This may be due to the pill burden or the increased likelihood of experiencing a side effect with more medicines and the difficulty for the individual to associate the side effect with an individual medicine and hence stopping all medicines.”
He says that community pharmacists can support patients with their medication and this study “supports the need for appropriate questioning when an additional agent has been added for the management of blood pressure through the use of enablers such as the New Medicines Service as to whether the individual has experienced any difficulty or complications with their current therapy to identify whether non-adherence is a potential cause of uncontrolled blood pressure.”

Source: MAG / The Pharmaceutical Journal
Mahendra Patel, a member of the Royal Pharmaceutical Society English Pharmacy Board, who was also a member of the NICE guideline development group on medicines adherence, says: “While the non-adherence figures are high, hypertension is asymptomatic and often people may not understand the full value and importance of taking their medicines.
He adds: “The patient demographic is also important. In black minority ethnic groups this non-adherence figure could potentially be much higher.”
References
[1] Gupta P, Patel P, Å trauch B et al. Risk Factors for nonadherence to antihypertensive treatment. Hypertension 2017;69:1113-1120. doi: 10.1161/HYPERTENSIONAHA.116.08729