Scottish government
In 2020, the number of drug-related deaths in Scotland, the majority resulting from use of opioids or benzodiazepines, rose to more than 1,300 — its highest annual number since records began. It was a situation that Scottish first minister Nicola Sturgeon said was “unacceptable” and “shameful”, becoming something of a political football in Holyrood.
To find out more, The Pharmaceutical Journal caught up with Angela Constance, the Scottish government minister responsible for drugs policy, to see how she is planning to turn this situation around.
Constance has resources at hand to do this. In June 2021, the Scottish government announced that it would allocate £14.4m to frontline services in 2021/2022 to help reduce the number of drug-related deaths, funding that will come from a larger pot of £250m over the next five years.
The money includes £4m to implement new medication-assisted treatment (MAT) standards that will enable drug users to receive same-day treatment for drug-misuse, and a further £4m for the provision of long-lasting buprenorphine — an opioid substitution treatment — in prisons and the wider community.
Constance admits herself that that there is “a mountain to climb” and she is going to have to navigate road blocks put up by the UK government — such as their refusal to legalise drug consumption rooms — as well as needing help and support from the pharmacy profession to get help to those who need it.
Why are drug-related deaths continuing to rise in Scotland?
It’s complex. Since around 2009, we’ve seen an increase in benzodiazepines being implicated in drug-related deaths, in excess of 450%. We really need to be better at following people up; so, we’re now investing more in outreach services and better care pathways. When someone has a near-fatal overdose, we need to make sure that the services are in touch with them at that moment of crisis, because we know that more than half of the people that we lose have a history of overdose. It’s about supporting people and implementing all evidence-based interventions — and there is evidence from around the world that we need to implement these in Scotland.
In June 2021, the Scottish government announced funding of £14.4m to help reduce the number of drug-related deaths. Where will that be directed?
We have made an additional investment over the next five years [to 2026] of £250m. That includes £100m investment on residential rehabilitation, and a £13.5m uplift for alcohol and drug partnerships, organisations responsible for commissioning and developing local strategies for tackling problem alcohol and drug use and promoting recovery, based on local needs.
In terms of interventions around access to treatment and reducing harm, for the first time, we’ve published medication-assisted treatment (MAT) standards that need to be embedded by April 2022. These standards are about things like same-day prescribing and informed choice. Pharmacy has a really important role in ensuring people have knowledge of their medications.
On top of that, we’re investing in widening treatment options, with an additional £4m to support the expansion of, buvidal [slow-release buprenorphine] and £3m investment in outreach services. We also want to see more heroin-assisted projects in Glasgow, and we’ve allocated some resource to that and are discussing with other services and health boards about the level of interest and where to go next.
What work is being done to identify and address the underlying causes of drug-related deaths?
A key part of our national mission is to ensure that the emergency work — and this is a public health emergency — is connected to broader work to improve lives and life chances.
It needs to be joined at the hip with our work in mental health and with our work to make the criminal justice system more humane. It also needs to be connected with our work in education and primary prevention, and our work to tackle poverty and inequality.
This is a public health emergency
We know that people in the poorest communities in Scotland are 18 times more likely to die of a drug-related death, and so tackling poverty and inequality is absolutely at the core — it has to be an all-government, all-Scotland approach to turn the tide on drug-related deaths.
Stigma towards drug users and drug services is still widespread. What needs to be done to challenge this?
Stigma is a huge barrier. People who use drugs and their families are among the most marginalised folk in our society.
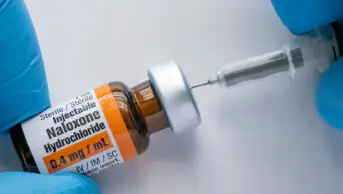
This week [31 August 2021] we launched a national campaign around naloxone to point people to the StopTheDeaths website so they can equip themselves to spot the signs of opioid overdose and know how to access training and naloxone kits. Part of that is about that wider engagement with the public, but it also has an important part in tackling stigma and explaining that these deaths are preventable and that these people should be saved.
The scale of the challenge is immense in Scotland, but we’re beginning to have a more honest discussion. We have a mountain to climb, but we should have hope that change is possible.
I understand that you are consulting on how to legally establish consumption rooms — have you made any progress with this?
We have a manifesto commitment to overcome the legal barriers to introduce safe consumption rooms in Scotland.
I will continue to engage the UK government on the evidence; and all the evidence shows that safe consumption rooms save lives and prevent people dying from an overdose. They also help connect people with other services that help them access treatment or go forward on their journey. There are at least 100 drug consumption rooms across Europe, Australia and parts of North America.
We want to have consumption rooms that are clinically and legally safe, both for those who use the service and those who work in the service. That work is continuing; it is progressing, It’s not there yet but we remain committed to finding the best ways to implement all evidence-based interventions.
I met with the Royal Pharmaceutical Society in early September 2021 and I’m really pleased that there is another expert voice supporting safe consumption rooms, as well as heroin-assisted treatment and the work in and around buvidal, naloxone and the MAT standards.
Why is there such a disparity between the Scottish government and the UK government when it comes to addressing the drug death crisis?
In Scotland, our situation is much more acute, so our focus on solutions will have a harder edge. We have the highest rate of drug-related deaths in Europe — that’s not a good place to be.
As well as reducing the supply of drugs, we need to be reducing the demand for drugs
We see this as a public health emergency, but the UK government is looking at this through a criminal justice lens. In Scotland, there is a recognition in the criminal justice system that we can’t arrest our way out of a public health emergency or a drugs death crisis — as well as reducing the supply of drugs, we need to be reducing the demand for drugs, because that’s the other side of the equation that, if I can say with respect, the UK government have less cognisance of.
What role are pharmacists playing?
I’ve been really encouraged by the appetite and the engagement of pharmacists in Scotland. I am a former social worker, so the concept of the multidisciplinary team is one that I embrace.
Pharmacists can help us with our work in tackling stigma and have a role in our ambitions to widen access to treatments. I know that they want to play a part in widening the distribution of naloxone and are supportive of evidence-led interventions in terms of heroin-assisted treatment and safe consumption rooms.
The Drug Deaths Taskforce has funded projects to support community pharmacies to provide buvidal; to support specialist pharmacy services, particularly in areas of higher need; and work in relation to the supply of naloxone projects around overdose prevention.
You may also be interested in

Study results raise concern about naloxone efficacy against some synthetic opioids

Community pharmacies urged to plan ahead for Easter bank holidays with methadone safety resources