Wes Mountain/The Pharmaceutical Journal
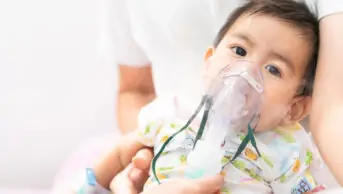
According to Asthma+Lung UK, the UK has the worst death rate for lung conditions, such as asthma and chronic obstructive pulmonary disease (COPD), in Western Europe. The same data show that the UK’s mortality rate for asthma is twice as high as that of the next worst country in Europe, which is unacceptable given that the National Review of Asthma Deaths (NRAD) reports that two-thirds of these deaths are preventable.
So, why is this the case? Delays in diagnosis, poor housing, high pollution levels, overuse of short-acting beta-agonist (SABA) and underuse of personalised action plans are some of the reasons given. But — surprisingly — the NRAD’s primary finding was complacency among both healthcare professionals and patients. Asthma is just not taken seriously enough.
Community diagnostics centres
Early and accurate diagnosis of respiratory illness is essential to starting patients on the right treatment pathway, but reduced access to healthcare during the COVID-19 pandemic and subsequent backlogs have resulted in plummeting diagnosis rates, according to the ‘COPD in the UK‘ survey report, published by Asthma+Lung UK in November 2022.
Community diagnostics centres have been touted by the government to help bust COVID-19 backlogs and diagnose patients more quickly without the need to see a specialist. GPs will be able to refer patients with symptoms of heart and respiratory problems for various checks at their local community diagnostics centre, which aim to provide a one-stop shop for scans and tests.
The ‘COPD in the UK’ survey revealed that almost a quarter of people across the UK were waiting five years or more for a diagnosis, while one in eight people waited more than a decade
However, the reality is that community diagnostics centres will not be replacing the role of primary care anytime soon and practices are in urgent need of funding to provide quality-assured testing. For most GP practices, the only route currently available is referral to secondary care, but waiting times for diagnostic testing are far too long; locally, we have waiting times of 6–12 months just for routine spirometry. This leads to unacceptable delays in diagnosis and initiation of treatment. The ‘COPD in the UK’ survey also revealed that almost a quarter of people across the UK were waiting five years or more for a diagnosis, while one in eight people waited more than a decade.
Time for action
Poor respiratory health has been closely related to deprivation and the Black Country has some of the most deprived neighbourhoods in the UK. Respiratory indicators, such as patients taking six or more SABA inhalers, are higher than the national average in Dudley, West Midlands, providing motivation for action.
Having been accredited by the Royal Pharmaceutical Society as a ‘Pharmacist with a special interest in respiratory care’ in 2011, I launched a pharmacist-led specialist respiratory clinic in primary care in January 2022 for the diagnosis and management of asthma and COPD, aimed at being a one-stop service that incorporates quality assured spirometry and FeNO testing, which measures airway inflammation, offered across GP practices in Dudley.
Patient outcomes
The clinic runs for two days per week, rotating between two new GP practices every quarter. Practices are prioritised based on a risk stratification approach using available respiratory health data and case-finding patients in each practice. Searches were created to identify patients who were at highest risk, including frequent hospital attenders, high SABA inhaler users, frequent oral prednisolone users and patients on inhalers without a diagnosis.
The clinic also takes direct referrals from clinicians in each practice for suspected asthma/COPD and the management of difficult cases before referral to secondary care.
Between November 2022 and November 2023, 374 patients were reviewed in the clinic. Of these, 74 were direct referrals from practice clinicians.
Some 83 patients were diagnosed with asthma and 29 patients with COPD, and started on optimal treatment. A total of 31 diagnoses of asthma/COPD were excluded and 8 patients were identified as being previously misdiagnosed with asthma/COPD. The clinic also identified 15 patients for referral to the secondary care ‘Difficult asthma clinic’ for consideration of biologic treatment and 7 patients who were stepped down from high-dose inhaled steroid treatment. The clinic also corrected poor inhaler technique in 137 patients.
More than 200 patients with poor asthma control or who were overusing SABA inhalers were reviewed and managed in the 12 months to November 2023, potentially avoiding a similar number of hospital admissions, emergency department visits or outpatient appointments.
Feedback from patients and clinicians using the service has been overwhelmingly positive.
Diagnosing asthma can be difficult and patients often suffer with symptoms for years, so it is a great feeling to finally give them a diagnosis and start them on the correct treatment in quick time. Assisting patients who overuse SABA inhalers is one of my specialities — I am always looking for ways to reduce their psychological reliance on these inhalers.
Pharmacists can play a crucial role in tackling health inequalities in respiratory care and I would encourage more pharmacists to upskill themselves and get involved in managing respiratory patients — an asthma and COPD diploma is a good start. Just remember: small behavioural changes can make a huge difference to the lives of respiratory patients.