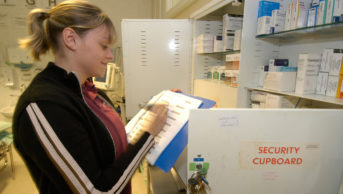
It is one year since the pharmacy regulator in Britain launched a prototype inspection model for pharmacy premises. The General Pharmaceutical Council (GPhC) system grades pharmacies on a scale of excellent, good, satisfactory or poor. To date, more than 2,300 pharmacies — around one in every six in Great Britain — have been assessed. A recent survey of some 703 of these pharmacies, conducted by community pharmacy lobbying group Pharmacy Voice, found that 96% had been rated as ‘satisfactory’, with only a handful of pharmacies awarded other grades.
Reading the GPhC’s 26 standards for registered pharmacies, which cover everything from staffing levels and equipment to risk management and delivery of services, it is understandable why the top two grades are so rarely awarded. Satisfactory, to the GPhC, means that a pharmacy meets the “vast majority” of individual standards, with any standards not met carrying a low risk of harm to patients. The regulator also advises that most pharmacies will fall within this category.
Tough grading is a welcome step. It drives up standards of care and makes high quality an aspiration that requires dedication and hard work from pharmacy teams.
Pharmacies’ inspection ratings are not currently available to the public, and so there is no risk of misinterpretation at this point. But the language used for the grades could have implications for the majority of pharmacies. We have become accustomed to expect more than a passing grade from service providers, choosing the products we buy or where we dine under the guidance of four or five star reviews. Would a patient want to visit a ‘satisfactory’ pharmacy only one step above ‘poor’? And, as the National Pharmacy Association has warned, might commissioners only wish to offer contracts to pharmacies that are ‘good’ or ‘excellent’? The Pharmaceutical Journal asked the GPhC for a top-level breakdown of how pharmacies have been graded, but the regulator declined to comment because the scheme is still in development. The GPhC will hold a consultation before finalising its model.
The GPhC’s willingness to listen to comments before finalising its inspection model is commendable, and it is crucial for pharmacists who have been through the inspection process to respond when the consultation launches.
Pharmacists should report back on the approach of the inspectors, the quality of feedback on how to make improvements, the time allowed to respond to recommendations, and how the process could be made fairer and more supportive.
The GPhC has indicated that it wants to make regulation fit for purpose. So the reputational implications of the new system ought to be considered by the GPhC, too.