Science Photo Library
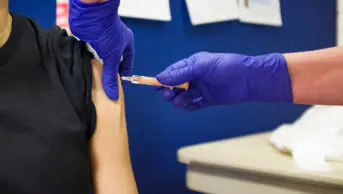
On 2 December 2020, the first-ever COVID-19 vaccine was approved for use in the UK — marking the start of a truly unprecedented vaccination programme. Unprecedented: a word used countless times throughout this pandemic, yet it’s hard to deny the outstanding success of this programme so far. This success, however, is not sustainable.
An ‘en-masse’ model was originally employed to deliver vaccines: an approach largely dictated by the storage needs of the Pfizer/BioNTech vaccine and the limited security of supply. Hospital hubs, primary care network (PCN) sites and community pharmacy contractors all organised mass vaccination centres across the UK. And there have been numerous examples of excellence from pharmacy contractors, who have provided vaccines from pharmacies, as well as temporary vaccine centres in village halls, religious buildings and other unusual locations.
The arguments for community pharmacy providing COVID-19 vaccinations (and indeed any vaccine) are well known. Easy access is one of community pharmacy’s greatest assets, owing to their location and opening hours. The huge success of the 2020–2021 influenza programme alone (2.6m vaccines have been given so far) demonstrates both the sector’s continued focus on vaccination, and the public’s growing acceptance of the role of pharmacists.
But despite these success stories from our sector, we have not all been enabled to dedicate ourselves to the national vaccine campaign. The initial requirements precluded many pharmacies from providing COVID-19 vaccinations: the requirement for pharmacies to provide at least 1,000 vaccines per week was impractical for the majority of pharmacies.
By 30 December 2020, however, the approval of the Oxford/AstraZeneca vaccine offered an opportunity for change. Coupled with the experience of nearly 200 first-wave vaccination centres, there was a chance to reflect on the current design and requirements, in light of the friendlier storage and use characteristics of the new vaccines.
It was then that the Company Chemists’ Association led a cross-sector group, comprising the National Pharmacy Association, the Association of Independent Multiple Pharmacies, the Royal Pharmaceutical Society and the Pharmaceutical Services Negotiating Committee, to engage with NHS England and NHS Improvement (NHSEI), as the bodies considered the operational requirements and the changes needed to allow many more contractors to provide this vital intervention.
On 16 February 2021, pharmacy had a victory — NHSEI issued a call for new applications from pharmacy contractors. This opportunity also recognised the value of sites distributing lower volumes of vaccines — smaller locations were permitted to apply to provide 400 vaccines per week. This fantastic move will bring COVID-19 vaccines closer to people’s homes, and make the most of experienced pharmacy teams across the country. Over the coming weeks, more and more pharmacies will start ‘filling the gaps’ and provide better access to vaccines for everyone.
But this approach cannot go on indefinitely. It seems likely that seasonal coronavirus vaccines will be around for some time. New guidance on COVID-19 vaccines from the Medicines and Healthcare products Regulatory Agency is a clear indication of this, with it stating: “a regulatory approach like the seasonal updates for influenza vaccines can be taken”. It is likely that we will be re-vaccinating against coronavirus year on year and so, to this effect, the government is planning its revaccination programme for autumn/winter 2021.
So far, mass vaccination centres have been an effective way of vaccinating at scale and at pace. However, this approach has required many professionals to reduce existing work, pause projects or work additional hours. Similarly, many sites are at venues that are lying empty owing to lockdown restrictions; eventually, these sites will reopen. So neither the overall burden on the workforce, nor the use of these sites, can continue indefinitely. As the coronavirus vaccine programme moves from essential to routine healthcare, we need to adjust practice to incorporate it.
It should be community pharmacy that leads this ‘business as usual’ model. NHS leaders may initially look to replicate the successful influenza programme — with good reason, given its annual success. However, COVID-19 has created an enormous backlog of both unmet need and late diagnosis for mental and physical health conditions. Secondary care, general practice, PCNs and community teams are likely to be inundated with work for years to come. How will these settings manage an additional vaccine programme too?
Community pharmacy, on the other hand, has remained physically open to the public throughout the pandemic and managed ever-increasing volumes of patients accessing the services they could not access through more traditional routes.
Pharmacies have pivoted their businesses to meet the demands of mass vaccination services and have learnt, and demonstrated, how vaccination can be provided at scale in the community. There will always be patients who need or choose to be vaccinated by their GP, but the overall seasonal vaccination programme should be designed with community pharmacy as the primary provider.
The numbers are significant. Even accounting for lower uptake in the future, there are 10 million people likely to need vaccinating owing to their age alone, and another 7.5 million will be clinically indicated. With planning, community pharmacy could, and should, be tasked to vaccinate the 10 million age-eligible patients. The pharmacy sector can do it, but it needs support to enable it to truly lean into this clinical role.
Changes to automation of dispensing are already being introduced, and the roles of pharmacists and technicians are both evolving. For example, the national protocol for the vaccine currently allows pharmacy technicians (who could not normally operate under a patient group direction [PGD]) to administer vaccines. We must take this further: the law needs to change to allow pharmacy technicians to use PGDs.
These changes will help us to achieve one of our sector’s goals — to move away from a dispensing model, and towards a clinical one. Our vision for the coronavirus vaccine programme will encourage the sector to quickly make necessary changes in professional practice and new technologies.
Pharmacy is changing, and the vaccination programme should too. Simon Stevens, chief executive of the NHS, described the COVID-19 vaccination programme as “two sprints and a marathon”. The marathon starts when we build a programme for the new normal.
Community pharmacy has a ‘once-in-a-lifetime’ opportunity. This is not hyperbole. As a sector we can step forward and lead, or we can continue to just support other, better served parts of the system. Given the pressures everyone is under, I believe that we have an obligation to lead.
Nick Thayer, professional research and policy manager, the Company Chemists’ Association