Abstract
Aim
To ascertain whether successfully completing a supplementary prescribing (SP) course can empower pharmacists in terms of their extended roles.
Design
Postal questionnaire and telephone interview.
Subjects and setting
38 pharmacist supplementary prescribers, selected by purposive sampling, who completed a supplementary prescribing course in the UK between October 2004 and March 2005.
Outcome measures
Qualitative and quantitative analysis of respondents’ written comments, validated and enriched by telephone interview.
Results
Subjects undertook a course mainly for reasons of personal development and to benefit patients (>80%); most were positive about their course. Overall, subjects emerged from their courses in confident mood to start their new role and were engaged in SP for a wide range of therapeutic areas. A number of barriers to role development were identified, notably in community pharmacy, where time and lack of access to patient medical records were particular problems. A feeling of lack of support was prevalent among primary care trust pharmacists. Hospital pharmacists had written the most SP prescriptions in the previous month and appeared to be facing fewer obstacles. A clear majority (>80%) were in favour of progressing to independent prescribing and allowing greater prescribing powers for other health care professionals.
Conclusions
This study provides evidence that SP qualification can empower practising pharmacists, but that due consideration should be given to providing a supportive environment in which to practise.
The enactment of Section 63 of the Health and Social Care Act 2001 gave pharmacists the opportunity of becoming supplementary prescribers — that is pharmacists who, in a voluntary partnership with a clinician (the independent prescriber) and the patient, could implement an agreed, patient-specific clinical management plan
(CMP) under which they could prescribe medicines. This expansion in the traditional pharmacy role was prompted by three things:
- An acute shortage of GPs leading to work overload, particularly in the area of repeat prescribing for chronic conditions, where supplementary prescribing could provide patients with quicker and more efficient access to medicines
- An opportunity, through drawing up a CMP, to involve patients more directly in their own care
- An opportunity to make the best possible use of trained pharmacists in the prescribing team, which already included dentists and nurses
Supplementary prescribing by pharmacists was embraced enthusiastically by the Royal Pharmaceutical Society, which surmised that it would lead to an “improved patient experience” through “better access to care, better quality of care and improved patient safety”.1 In September 2002 the Medicines Commission and Committee of Safety of Medicines released plans for implementing supplementary prescribing and, shortly afterwards, the Royal Pharmaceutical Society finalised a syllabus for an accredited supplementary prescribing course and invited higher education providers to submit proposals.2 The keystone to pharmacist supplementary prescribing became successful completion of a Society-accredited course and subsequent certification. Training finally got under way in the spring of 2003. The outline course syllabus, course accreditation procedures, prerequisites for applicants and the competencies they are expected to achieve by undertaking the course are described in detail elsewhere.2–4 Up to January 2005, some 27 supplementary prescribing courses had been accredited5 — most at universities with established schools of pharmacy. The Portsmouth University supplementary prescribing course was accredited in December 2003 and took its first pharmacist cohort in spring 2004.
Successful completion of the supplementary prescribing course is rewarded by a “Practice certificate in pharmacist supplementary prescribing”. Although this is a prerequisite to supplementary prescribing, students must then formulate CMPs with an independent prescriber for each patient they intend to support. There are wide variations in the time over which the courses are spread (three to nine months) and delivery (mostly didactic to mostly distance learning), but the requirements for 12 days’ practical training under the auspices of a designated medical prescriber and subsequent registration with the Royal Pharmaceutical Society as a supplementary prescriber remain paramount.
At the start of this study (October 2004), some 240 pharmacists were reported to have qualified as supplementary prescribers6 and a number of largely anecdotal reports concerning supplementary prescribing implementation had emerged: all were small-scale and limited either to course implementation,7–10,13 one or two supplementary prescribing courses,12 one branch of the profession11 or expressed the viewpoint of a single practitioner.14–16 Although these studies highlight possible benefits, drawbacks and pharmacists’ preconceptions of their new role, many issues surrounding supplementary prescribing are still poorly understood. For example, how do supplementary prescribers see their new role?
What are their experiences so far? What doors have been opened to them and what barriers to further development have been placed in their way? Such information would be useful to policy makers and supplementary prescribing course providers alike. This study sought answers to these questions.
Methods
During November and December 2004, a piloted questionnaire (copy available from the authors) was administered to a sample of pharmacists known to have completed a supplementary prescribing course and to have achieved supplementary prescriber status in the previous year. Subjects were identified in two ways. First, the Practice and Quality Improvement Directorate at the Royal Pharmaceutical Society provided assistance by e-mailing 54 recently qualified supplementary prescribers held on its database. Subjects were given a brief explanation of the study and a copy of the questionnaire as a Microsoft Word document attachment. They were asked to e-mail their completed questionnaires back to the Society, which then forwarded hard copy to the investigators. Secondly, additional potential subjects were identified either through the course leader of the University of Portsmouth supplementary prescribing course (JP) or a recent supplementary prescribing graduate of the course at the London School of Pharmacy (MT).
The questionnaire contained both open and closed questions designed to elicit information on five main themes
- Demographics, including the specialty currently worked in
- Reasons for undertaking the supplementary prescribing course and any barriers that were presented to enrolment
- Evaluation of the course they had undertaken and how it had prepared them for the supplementary prescribing role
- The new supplementary prescribing role itself, including reflection on whether qualification had changed the respondent’s role significantly, eg, in terms of therapeutic area, workload and job satisfaction
- Respondents’ perceptions of their medium-to long-term future as a supplementary prescriber
In each case, the questionnaire was accompanied by a covering letter from the authors, stating the nature of the study, why the subject had been selected, and containing an assurance of anonymity unless the respondent wished to participate further in a telephone interview. Questionnaire data were processed and analysed using Snap Professional version 4 (Mercator). Individual comments provided by respondents were analysed for content and expressed under a number of themes.
Telephone interviews were designed to validate and expand upon respondents’ replies in the written questionnaire. Each question on the postal questionnaire was repeated seeking clarification where ambiguous replies had been given, followed by two additional questions covering respondents’ attitudes to their progression from supplementary to independent prescribing and the extension of supplementary prescribing to other health care professionals. One of us (SW) conducted the telephone interviews, which had a piloted, structured framework; transcripts were recorded manually. Each interview lasted, on average, about 20 minutes. The transcripts were analysed for correspondence to the original written replies and remarks cogent to the two additional questions asked.
Results
In all, 63 individuals were targeted with the written questionnaire and 38 (60.4 per cent) responded (31 of 54 from the Society’s database and seven of nine recruited by word of mouth). This represented 30 per cent of all new supplementary prescribers then on the Society’s database. Ten respondents volunteered to participate in telephone interviews.
Demographics
Eighteen women and 20 men responded; 20 (53 per cent) were working in a primary care trust environment, 12 (32 per cent) in hospital pharmacy, and eight (19 per cent) in community pharmacy; three (8 per cent) described themselves as practice pharmacists. Several respondents held more then one position. Twenty-three (61 per cent) had been qualified as pharmacists for more then 15 years, 10 (26 per cent) for 11 to 15 years, four (11 per cent) for six to 10 years and one (3 per cent) for less than six years.
Before course participation
The reasons cited for undertaking the supplementary prescribing course are shown in Table 1.
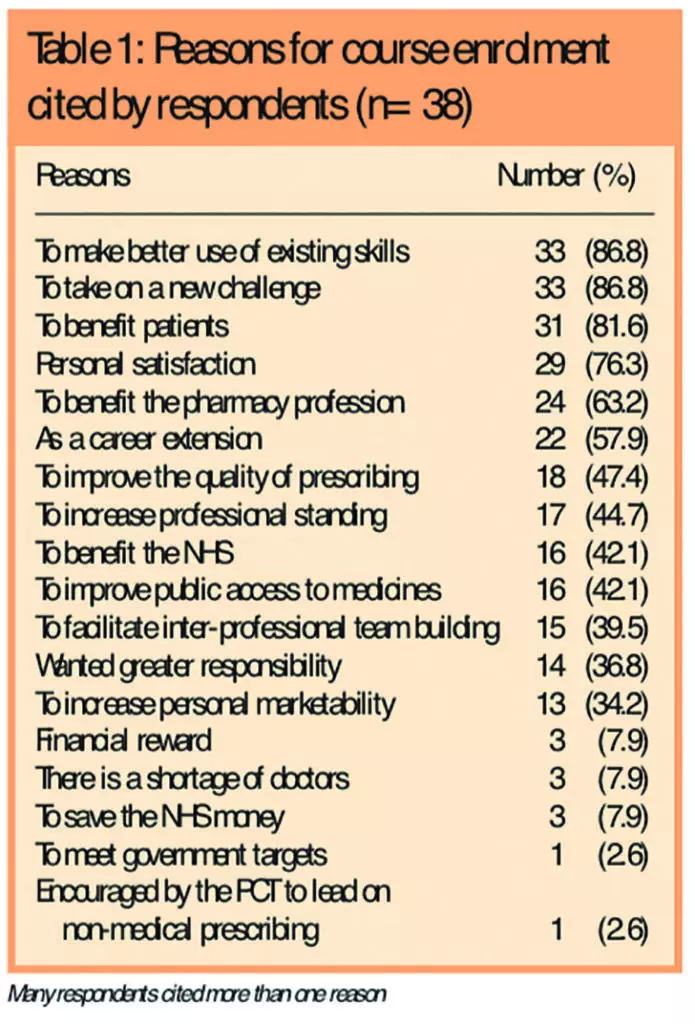
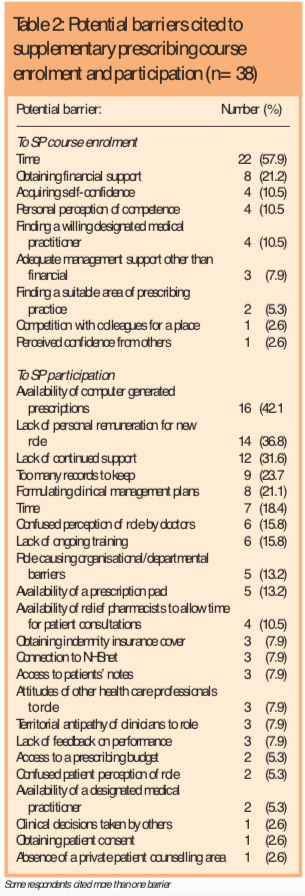
Potential barriers to enrolment, presumably overcome before participation, are shown in Table 2. Three respondents (7.9 per cent) replied that there were no barriers and a further 10 (26.3 per cent) left this question blank.

Course evaluation
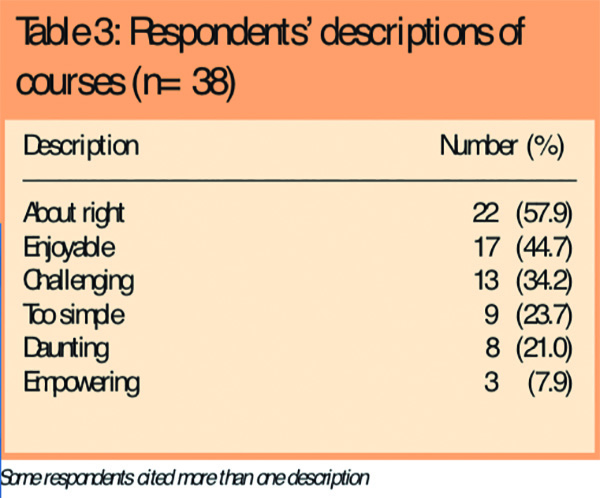
Subjects were presented with a list of descriptors of the course they had undertaken and were asked to tick any that applied. Responses are shown in Table 3. When asked “Would you recommend your course to a fellow pharmacist?” 31 (81.6 per cent) said yes. One respondent did not reply and six said no.
Effect of completing the course
Respondents’ feelings on successfully completing their supplementary prescribing course were described as confident (24, 63.2 per cent), liberated (nine, 23.7 per cent), nervous (eight, 21 per cent), inadequate (three, 7.8 per cent) and confused (two, 5.3 per cent); some respondents expressed more than one feeling. Table 2 shows the barriers to supplementary prescribing participation encountered by respondents after qualifying. The questionnaire also asked respondents if they perceived that their area of expertise had changed since completing the supplementary prescribing course. Most (24, 63.2 per cent) believed that this remained the same. Thirteen respondents who indicated that their role had changed cited the following reasons: the course had stimulated interest in other areas (five respondents), they had been asked by their trust to focus on a new area (four), and they had more to offer in this new area (four).
Respondents were asked to indicate in which area(s) they were currently prescribing and these are shown in Table 4.
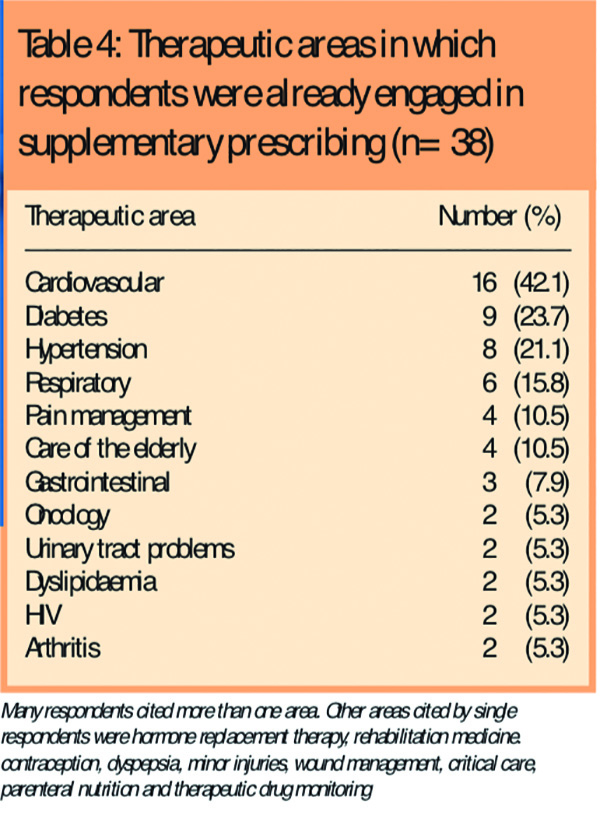
The most common fields cited were cardiovascular, respiratory and diabetes, with many respondents prescribing in more than one field. One respondent who had cited seven therapeutic areas subsequently took part in a telephone interview and stated: “If I can make a CMP and take responsibility for prescribing, I will.” It appears that some supplementary prescribing pharmacists are happy to prescribe across several areas of medicine given the chance.
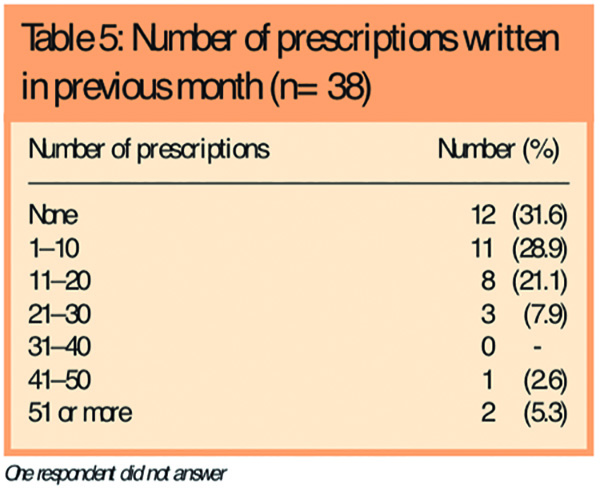
Table 5 shows the numbers of prescriptions written in the past month. This indicates that respondents’ involvement with supplementary prescribing was patchy at the time of the study, with almost one third not having produced a prescription in the previous month. These respondents gave the following reasons: they had not yet started (four respondents); the opportunity had not yet arisen (two); problems had been encountered in obtaining prescription pads and a prescribing number (one); and the PCT policy and infrastructure were not yet in operation (one). The overall impression was that more supplementary prescribing support was required before the role could be developed further.
Respondents were asked if they had dropped or delegated any of their current roles to make way for supplementary prescribing. Just over half (20, 52.6 per cent) stated that they had not. Relevant comments included “None — perhaps I should! There never seems to be enough time” and “None — I have reduced time available for the new role; I have to juggle my workload”. These remarks have resonance with the barriers to supplementary prescribing cited in Table 2, where seven respondents cited lack of time.
Four respondents had managed to make more time for supplementary prescribing by changing their work patterns, one by reducing the number of practices with which they worked and another by decreasing the amount of locum work undertaken.
The future
Respondents were asked how they saw their role developing in the next five years; the results are shown in Table 6. Most intended to develop the role as the opportunity arose and, eventually, to become independent prescribers. Almost half saw themselves teaching supplementary prescribing to others. Respondents were asked how supplementary prescribing should be taught in the future. Eleven (28.9 per cent) said they thought it should be taught as at present, 12 (31.6 per cent) as part of the undergraduate degree and six (15.8 per cent) as part of a postgraduate master’s degree.

Telephone interviews
When asked a cross-section of closed questions from the questionnaire, all respondents gave the same answer they had given previously, thus helping to validate their earlier responses. Two additional topics were discussed. First, all subjects responded positively to the proposition that supplementary prescribing should be extended to other health care professionals, but only after rigorous training, similar to that which they themselves had undergone.
Secondly, interviewees were asked for their thoughts on independent prescribing. All respondents were in favour, some viewing it as a logical step from supplementary prescribing, while removing some of the barriers inherent in the supplementary prescribing system, notably the need for CMPs (Table 2). Three respondents used the phrase “bring it on” to underline their enthusiasm. However, some doubts were expressed about the acceptability to the medical profession of fully independent prescribing pharmacists, suggesting that such a bold move should be introduced tactfully by preserving the doctor’s role in preliminary diagnosis but allowing the pharmacist to prescribe the most appropriate treatment.
Discussion
Demographics
Respondents tended to be experienced pharmacists working in either a PCT or a hospital; there were no clear differences in terms of gender.
Before course participation
Table 1 shows a wide variety of reasons cited for undertaking supplementary prescribing courses in the first place; the main influence was a need of personal development and benefits to the individual or to patients. rather than perceived benefits to the health care system. Time was by far the most commonly perceived barrier to commencing a supplementary prescribing course and the only one cited by respondents working in secondary care; other reasons were much less common. No pharmacist cited lack of suitable patients or personal ability to make clinical decisions as barriers to supplementary prescribing (Table 2).
Course evaluation
Table 3 indicates that most respondents felt positively about the supplementary prescribing course they had undertaken. Although 13 respondents found their course challenging, no one described it as too complex. The “challenge” may therefore have come from other sources, exemplified by one comment:“Too much to learn in three months.” Several comments indicated that the respondent’s course had not allowed sufficient time to develop practical experience, typified by “Lack of time for examination skills. . . . We only spent 10 minutes learning how to use a [blood pressure] monitor, which is not long enough to be confident in using it” and “Lack of practice days”.
Nine respondents indicated that they believed their course to have been too simple. Others indicated that their course had concentrated on peripheral topics such as communication skills rather than “empowering prescribers to self-assess their learning needs” and that it was the responsibility of the participant, rather than the course to “make sure they have the requisite [communication] skills prior to commencement of the course”.
Although all supplementary prescribing courses are accredited by the Royal Pharmaceutical Society, there are differences in course delivery. It is not surprising that respondents had differing views on the course they had just completed. Some respondents expressed a jaundiced view of being taught with nurses, because the learning needs of pharmacists were different, typified by the following comment: “The course was run for nurses and adapted to take in pharmacists and was not tailored for the skills and knowledge of the pharmacists . . . so was oversimplified and not sufficiently challenging.”These views resonate with that of McRobbie’s argument17 that the two professions should be kept separate in supplementary prescribing training because of the differing levels of clinical knowledge and practical experience.
In contrast, some respondents said that shared learning helped their personal development, because nurses “brought other skills to the course that pharmacists do not have and can learn from” and “approach it from a different angle — they have more hands-on experience whereas pharmacists have a more therapeutic background”. In the light of these contrasting views, it seems right that there is a variation in course delivery so that pharmacists can choose the course best suited to their learning needs. Furthermore, course providers should adopt a pragmatic approach to supplementary prescribing courses that allow joint admissions, ensuring that the needs of pharmacists and nurses are met. Where shared learning helps mutual development, there should be joint teaching. This has been addressed on the Portsmouth supplementary prescribing course by providing separate training sessions with a profession-specific focus in particular areas, such as clinical evaluation skills for pharmacists and pharmacology and therapeutics for nurses, while providing co-disciplinary sessions on drawing up therapeutic frameworks, formulation of CMPs and case studies. As reported elsewhere,12 the importance of allowing sufficient time to train pharmacists in physical examination skills was highlighted by a number of respondents in the present study. Hence supplementary prescribing courses need to be flexible to account for the differing learning needs of pharmacists, nurses and perhaps other health care professional groups as supplementary prescribing is extended to them.
Effect of completing the course
In general, the supplementary prescribing courses undertaken provided a boost in the individual’s confidence, illustrated by comments that supplementary prescribing had provided them with a “greater role within the team”, that they were “better recognised in the team”, “proud” and “excited and proud to be part of a new initiative in pharmacy”.
Cross-referencing of replies showed that hospital pharmacists encountered the least problems in implementing supplementary prescribing, largely due to the availability of patient notes and a pre-existing supportive infrastructure, noted elsewhere also.18,19 One primary care respondent emphasised the fact that a lot of prescribing is for acute conditions and drawing up CMPs for such patients was impractical. One way of avoiding this problem was the development of true independent prescribing. Drawing up CMPs was a problem in both primary and secondary care, although other respondents did not elaborate on specifics. This would seem to represent a problem area in any setting.
Respondents cited a wide range of barriers to starting supplementary prescribing. Remuneration was a prominent worry among approximately half of the pharmacists working in primary care, both in terms of starting the course and supplementary prescribing participation. Availability of computer-generated prescriptions and lack of ongoing support were also features. Budgetary issues were underlined by two comments from PCT pharmacists. The first was: “The biggest barrier to supplementary prescribing in my PCT at the moment is lack of money. PCT is vastly overspent so may have to stop [prescribing] clinics to concentrate on cost-cutting work.”
The second was:“The PCT still has a lack of direction on supplementary prescribing by pharmacists. No budget has been set for us to use. Supplementary prescribing is a great advance for pharmacy, particularly in secondary care. In primary care, however, it has not been thought through. Roles are having to be developed ad hoc, resulting in a fragmented service. This means that, in many areas, patients do not have proper access to the advantages that supplementary prescribing can offer. We need a coordinated national promotion of supplementary prescribing to PCTs.”
The importance of providing a supportive environment in which supplementary prescribing can flourish has been noted previously.19,20 Without this, it is clear that some supplementary prescribing pharmacists may lose their initial enthusiasm and confidence, fall by the wayside and waste their training. It would be sensible for all supplementary prescribing course providers to ask if a supportive infrastructure is in place at an applicant’s workplace before they are accepted on the course.
It might be expected that community pharmacists face the most barriers to developing supplementary prescribing, as reflected in the results of this study. This stems principally from a lack of access to patient medical records (PMRs).9 In the present study, barriers to supplementary prescribing of access to patient notes and lack of connection to NHSnet were cited by community pharmacists.
The impression from the above is that supplementary prescribing courses had encouraged and empowered participants but that in some cases the infrastructure to take supplementary prescribing forward was lacking. Some problems encountered by respondents in this study are reminiscent of the initial experiences of nurse prescribers, where it was found that barely half of all those who had undertaken training used their new skills in their current job.21 This was explained in part by some health authorities and NHS trusts training nurses without due consideration to local service needs or the lack of opportunities for individuals to assume the new role. Lack of opportunity soon led to loss of enthusiasm and competence. Although these problems were rectified, those designing and recruiting for supplementary prescribing training courses should bear these possibilities in mind, ensure that they are fulfilling a genuine need and prepare students with a clear progression pathway in supplementary prescribing. Research has demonstrated that pharmacists who have an existing role within a clinical environment have found it easiest to establish a prescribing service to patients.20 Already there is evidence to suggest that in a secondary care setting, supplementary prescribing can be adapted to improve discharge planning, reduce medication errors and waiting times for discharge medication and minimise wastage.22
The future
Wilson has suggested23 that eventually, supplementary prescribing should be incorporated into the undergraduate MPharm degree and about a third of respondents thought that supplementary prescribing should be included there in the future. Current supplementary prescribing course accreditation requirements (notably the need to have at least 12 days’ learning in a practice environment and the availability of a designated medical practitioner to provide supervision, support and shadowing opportunities) preclude introduction into an already overcrowded undergraduate syllabus.
Telephone interviews indicated that respondents were aware of this, typified by the following comment that supplementary prescribing should be “kept separate from the undergraduate course — and with a minimum amount of experience required before you can apply (for certification), eg, a couple of years. It is a big responsibility to take on.” One respondent stated that he had “grave concerns about integrating this into the undergraduate course unless limitations are put on the time to start writing the first prescription, eg, two years post-qualification.
Undergraduates do not understand their clinical limitations, nor do they comprehend prescribing in multiple co-morbidity.” Another believed that some of the theory could be taught at undergraduate level, but that the practice and mentoring aspects should be left until after graduation. One respondent said that it takes four to six years to become sufficiently competent to begin supplementary prescribing in a therapeutic specialty and that incorporation of supplementary prescribing into a recognised award is more feasible at postgraduate level.
Many course providers, including the University of Portsmouth, allow academic credit for successful completion to count towards the award of a postgraduate diploma or MSc degree. Most respondents in this study thought that supplementary prescribing was best taught at postgraduate level. When discussing supplementary prescribing in secondary care, McRobbie.17 expressed a similar view: “The people who do most of the prescribing in hospitals are junior medical staff, who are not good at it. Should we be replacing them with junior pharmacy staff, who will not be good either? There are some real risks in this strategy.”
The Royal Pharmaceutical Society should think carefully about the practicalities and the necessary changes to its MPharm accreditation syllabus, not least of which would be a substantial increase in training devoted to developing and honing diagnostic skills, before sanctioning an undergraduate route to the supplementary prescribing qualification. There is no evidence that our nursing colleagues have considered a similar option.
Some telephone interviewees believed that the introduction of independent prescribing would sound the death knell of supplementary prescribing. But, as Bellingham has suggested,24 the co-existence of supplementary prescribing courses would allow pharmacists who do not want to become fully fledged independent prescribers the opportunity to extend their roles to a level with which they feel most comfortable at the time, for example, supplementary prescribing for a limited range of chronic conditions. As one respondent said in a telephone interview: “I think you need to be a supplementary prescriber for a few years before you can become an independent prescriber since you need to build up experience, confidence and competence.” Two other respondents echoed recent calls in the literature24,25 that as other healthcare professionals extend from supplementary prescribing to independent prescribing, so should pharmacists, to avoid losing out in the prescribing rights race. The prophecy has, of course, become reality, with the stated intent to extend independent prescribing rights to suitably trained pharmacists in the spring of 2006.26 The profession, and education and training providers in particular, should be ready to respond to this new challenge.
Conclusions
A wide variety of supplementary prescribing courses is currently available. Respondents in this study were prompted to undertake a supplementary prescribing course mainly for reasons of personal development and most were positive about their particular learning experiences. Overall, subjects emerged from their courses in confident mood to start their new role but encountered a range of barriers to its development, notably in community pharmacy, where time and lack of access to patient medical records were particular problems. A feeling of lack of support was prevalent among PCT pharmacists. Hospital and PCT pharmacists had written the most supplementary prescribing prescriptions in the past month and hospital pharmacists appeared to be facing fewer obstacles.
A clear majority were in favour of progressing to independent prescribing and allowing greater prescribing powers for other health care professionals. It is likely that the barriers to independent prescribing will be similar to those encountered for supplementary prescribing unless steps are taken to remove them. The Royal Pharmaceutical Society will be responsible for curriculum and accreditation criteria for independent prescribing education and training programmes developed by higher education institutions, and experience with supplementary prescribing programmes should inform these developments.
Independent prescribing training programmes should allow specialist training in the area(s) of expertise of the student and allow adequate time to develop diagnostic as well as therapeutic skills. Independent prescribing will allow much greater flexibility in prescribing; supplementary prescribing to independent prescribing conversion courses should be the favoured route with supplementary prescribing being perhaps a prerequisite. Whatever the course provided, supplementary prescribing to independent prescribing conversion courses should not be seen simply as a short cut for everybody. Careful consideration should be given to providing adequate time and facilities for candidates to develop the necessary skills, match training to local needs, integrate with other members of the health care team and target commissioned practice thereafter. While the need to draw up CMPs will be removed, access to patient medication records in primary care will be essential.
Acknowledgements
The authors thank all study participants. We also thank the head and secretary of the practice and quality improvement directorate at the Royal Pharmaceutical Society for handling the majority of the questionnaire mailing.
This paper was accepted for publication on 26 January 2006.
About the authors
Sarah Warchal, MPharm, is a preregistration pharmacy graduate,
David Brown, PhD, MRPharmS, is professor of pharmacy practice, and Jane Portlock, PhD, MRPharmS, is postgraduate course leader at the University of Portsmouth School of Pharmacy. Mark Tomlin, MSc, MRPharmS, is critical care pharmacist at Southampton General Hospital.
Correspondence to: David Brown, School of Pharmacy and Biomedical Science, University of Portsmouth, St Michael’s Building, White Swan Road, Portsmouth PO1 2DT
References
- Royal Pharmaceutical Society.Supplementary prescribing bypharmacists. London: The Society; 2003.
- Wilson P. The development of a curriculumfor supplementary prescribing.Pharmaceutical Journal 2003;270:21–22.
- National Prescribing Centre.Supplementary prescribing: a resource to help healthcare professionals to understand the framework and opportunities. Liverpool: NPC; 2003.
- Royal Pharmaceutical Society. Outline curriculum for training programmes to prepare pharmacist supplementary prescribers. London: The Society; 2002.
- National Prescribing Centre. Maintaining competence in prescribing — an outline framework to help pharmacist prescribers. Liverpool: NPC; 2003.
- Pharmacist prescribing: the reality. Pharmaceutical Journal 2004;273:483.
- Bellingham C. How supplementary prescribing is working for pharmacists in practice. Prescribing and Medicines Management 2004;(July):PM2–3.
- Edwards RM, Stewart DC, Cleland J, Cunningham ITS, Munro, K, McCaig DJ et al. The first wave of supplementary pharmacist prescribers: reflecting on the period of learning in practice. International Journal of Pharmacy Practice 2004; 12(Suppl):R47.
- Andalo D. Community pharmacists decide to “wait and see” before prescribing. Prescribing and Medicines Management 2003;3:5–7.
- While A, Mudaly M, Nathan A. Views of contemporary pharmacists regarding supplementary prescribing. International Journal of Pharmacy Practice 2004;12(Suppl): R43.
- Cassidy F, Hughes C, Adair C. Pharmacist supplementary prescribing: a preliminary qualitative exploration. International Journal of Pharmacy Practice 2004;12(Suppl): R87.
- Dawoud DM, Goodye LI, Lovejoy A, Greene RJ. Perceptions and perceived competencies of pharmacists on supplementary prescribing training courses in London and the South East. Journal of Pharmacy Practice 2004;12(Suppl):R40.
- Jones RE, John DN, Luscombe exploratory qualitative study of pharmacists’ views of supplementary prescribing. International Journal of Pharmacy Practice 2004;12(Suppl): R91.
- Lavender G. Opportunities in primary care: diary of a pharmacist prescriber. Pharmaceutical Journal 2005;274: 151–2.
- Smalley L. Supplementary prescribing in action — an example from primary care. Pharmaceutical Journal 2005; 274:213–4.
- Tomlin M. A year in the life of a supplementary prescriber. Hospital Pharmacist 2005;12:182–3.
- McRobbie D. Prescribing courses — one size fits all? Hospital Pharmacist 2003;10:480.
- Fitzpatrick R. Is it time we shared good practice in Supplementary Prescribing? Hospital Pharmacist 2004;11: 442.
- Latif S, Cantrill JA, Parker D, Tully MP. The changing views of pharmacists undergoing supplementary prescribing training. International Journal of Pharmacy Practice 2005; 13(Suppl):R50.
- Nicholls JS, Taylor B, Patel R. Early lessons learnt from supplementary prescribing for pharmacists. International Journal of Pharmacy Practice 2005;13(Suppl):R75.
- Granby T. Lessons learnt from the nurse prescribing experience. Pharmaceutical Journal 2003;270:24.
- Elfellah M, Hills G. Supplementary prescribing can be adapted to improve discharge planning. Pharmaceutical Journal 2005;274:338.
- Wilson P. What does the society think? Hospital Pharmacist 2003;10:479.
- Bellingham C. Independent prescribingdraws closer. Pharmaceutical Journal2005;274:8–9.
- Consultation on independent prescribing.Pharmaceutical Journal 2005;274:257.
- Connelly D. Independent prescribing:pharmacists are given flexibility of a full formulary. Pharmaceutical Journal 2005;275:627–8.

