
Courtesy of Peter Krykant
When The Pharmaceutical Journal speaks to Peter Krykant, it has been almost two weeks since he was charged by the police for obstruction. Krykant, a drug and alcohol worker and activist, was out in Glasgow operating a mobile drug consumption van, which has been set up with clean injecting equipment and medical supplies so that intravenous drug users can carry out supervised, safe injections.
People don’t want to die; that’s the simple reality of it
Krykant knew what he was doing could attract police attention. “We’ll be out again tomorrow,” he tells us, undeterred. As a former intravenous drug user, he is passionate about his project to provide a safe space for Glasgow’s estimated population of approximately 500 publicly injecting drug users. “People don’t want to die,” he says. “That’s the simple reality of it.”
In 2018, 1,187 people died from drug-related causes in Scotland, a 27% jump on the previous year’s figures[1]
. In 2017, the UK as a whole accounted for 34% of all drug deaths reported in the EU[2]
. Almost everyone agrees something needs to be done. And report after report over the years has recommended drug consumption rooms (DCRs) as one way to tackle the problem. In Glasgow, there is even a site earmarked for a DCR, next to an existing heroin-prescribing facility. So why is Krykant having to take matters into his own hands?
The answer is a political and legal minefield. The UK government drug strategy (decided in Westminster) is currently heavily focused on getting people off drugs, with a government spokesperson telling us that “we must prevent drug use in our communities [and] support people through treatment and recovery”. But, says Krykant, “the majority of people that we’re reaching out to with this injection facility, they’re not anywhere near that”.
By contrast, the Scottish National Party, which is the ruling party in Scotland, has an official policy of decriminalising the possession and consumption of controlled drugs, and moving to a public health approach. It has asked for drugs policy to be devolved to the Scottish Parliament, but has had no luck so far. Meanwhile, DCRs are caught in a tug of war between the two parliaments, with the Home Office so far refusing to grant permission for a Glasgow City Council-proposed trial of a DCR that has the backing of the Scottish government and the majority of Scots.
The proponents
There’s never been a death in one of these facilities from overdose
The first supervised DCR was set up in Bern, Switzerland, in 1986, and there are now more than 100 such facilities around the world (see Figure). Proponents say that they protect drug users from harm, while also reducing public nuisance through open drug use and unsafe disposal of needles. “There’s never been a death in one of these facilities from overdose,” points out Alex Stevens, a drugs policy expert at the University of Kent, who sits on the Advisory Council on the Misuse of Drugs (which has declared itself in favour of DCRs).
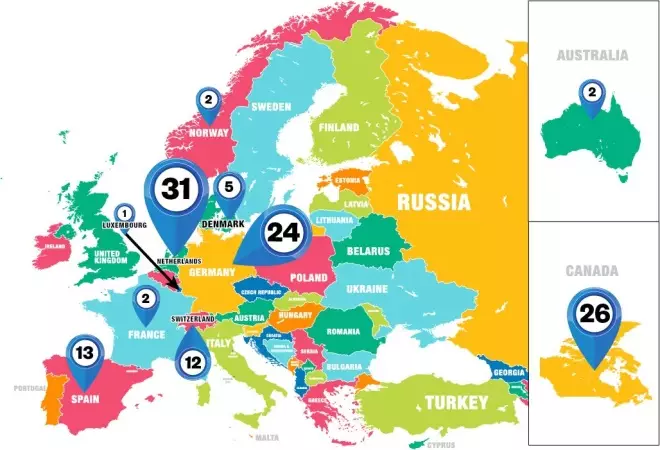
Figure: Global distribution of drug consumption rooms
Source: European Monitoring Centre for Drugs and Drug Addiction, Harm Reduction International.
The first official drug consumption room opened in Germany in 1986 and there are now more than 100 of them around the world, with further facilities planned in Belgium, Ireland, Portugal and Mexico
Stevens also says that people who use DCRs are “less likely to have wounds and infections where they’re injecting, and more likely to be referred on to other forms of treatment”. There are other benefits for drug users. “They’re obviously using clean equipment, so it reduces the transmission of blood-borne viruses, and in Glasgow we have an HIV outbreak within the population,” says Carole Hunter, a pharmacist who leads addiction services in the Glasgow area.
However, all of this is hard to quantify. As Stevens says, “One of the problems with drug consumption rooms is you can’t randomise them.”
What we do know is that DCRs target hard-to-reach populations who often have a long history of drug use, are or have been homeless, and have a history of incarceration. “People at that stage are probably not ready to move into treatment, but it’s making the initial engagement and linking them into treatment when the time is right,” says Hunter.
A study from a DCR in Germany in 2002 backs this up; it reported that one-third of interviewees had accessed treatment through the DCR[3]
. Although Krykant fears that the reach of his facility will be small, he does point users to treatment facilities and educate them about safe injection practices. “We’ve got a range of leaflets and booklets that we hand out to people.”
And the benefits go beyond helping drug users. DCRs can be beneficial for the general public. Hunter is on the receiving end of a lot of public complaints in Glasgow about discarded needles. “Some of the sites are quite incredible,” she acknowledges. “A drug consumption room can help to deal with a lot of that public nuisance.”
Furthermore, one study of the impact of a DCR in Sydney, Australia, showed that it significantly reduced ambulance callouts in the area in which it was set up, saving public money and reducing demand in hospitals[4]
. This result is perhaps not surprising given that, in the period of the study, more than 1,700 overdose cases were treated on site at the DCR.
The critics
Nonetheless, critics worry that DCRs are, at best, a “distraction” from treating drug addicts — as Kit Malthouse, UK government minister for crime, said in February 2020 — and, at worst, attractants for dealers and users, perhaps even increasing drug use. “The evidence doesn’t show that,” Hunter counters. “Injections are already happening.”
A lot of the arguments used against DCRs are familiar to Hunter from her experience setting up a needle exchange scheme in a pharmacy in Plean in the Forth Valley in 1992. “It was an old mining village and it had a significant drug problem,” she says. The needle exchange was “very successful”. Through it, the pharmacists were able to provide drug users with clean equipment, give them healthcare advice and link them into other services.
A drug consumption room is really an enhanced needle exchange
DCRs are seen as a step up from needle exchange schemes. “A drug consumption room is really an enhanced needle exchange,” Hunter says. “You get all the benefits of a needle exchange with the addition of a safe space.”
Krykant has this in mind when he takes his van out. “I park literally two-minutes’ walk from one of the busiest chemist needle exchanges in Glasgow, and another 30-second walk to a really well used public injecting site,” he says. The idea is that drug users who get their injecting equipment from the pharmacy will go to the van instead. “It’s cold, it’s wet, it’s horrible out there now in Glasgow.” It seems to be working. When we spoke to Krykant, he had supervised 14 injections the last time the van had been out.

Source: Courtesy of Peter Krykant
A drug consumption room, such as the one set up by Peter Krykant in a van (pictured), has the benefits of a needle exchange with the addition of a safe space
Both needle exchanges and DCRs can be a valuable source of data. “We collect information — housing status, what drugs they’re injecting, what they’re being supplied with, whether they’re in structured treatment,” Hunter says of needle exchanges. The plan for the official DCR in Glasgow was to use the same Neo data recording system there.
Krykant has noticed recently that a lot of drug users are injecting powdered cocaine. This can be a real problem. “Somebody may be injecting heroin one or two or three times a day, but with cocaine they’re injecting nine or ten plus times a day,” he says.
Stevens is also worried about the rise of cocaine injections in Glasgow. “It increases the risk of overdose and of disease transmission, which makes it increasingly important to have places where people can go to reduce the risks of those injections,” he says.
Lessons from overseas
There is a lot to learn from the experience of other countries with DCRs. Michael Olsen, a drugs activist and social entrepreneur, opened a mobile drug consumption van in Copenhagen in 2011 after making several previous attempts to open fixed facilities, including in a basement. “That was closed the day before we were due to open, by the authorities.”
When Olsen started his van, he was in a similar legal position to Krykant. The law was confusing. There was nothing explicitly banning the kind of facility he wanted to set up, but it was illegal to sell and buy illicit drugs or to possess them. Consequently, he expected that his van would be closed by the authorities “and then we wanted to make a test trial to see if it was legal or not”. But that day never came. “We were allowed to run for a year before the parliament made a new law,” he tells us. That law made it legal for municipalities to set up DCRs — Olsen had won the argument.
Now, Denmark has five DCRs, including the biggest DCR in the world, plus Olsen’s van, which he recently restarted to deal with some underserved neighbourhoods.
Krykant is hoping for a similar outcome, although the charges he faces (should they be pursued, which is still not clear) do not directly call into question the legality of his facility, which is what he would like for a test case.
There’s no law to stop you running a site where people inject heroin
In the UK, the piece of legislation Krykant wants to challenge is the Misuse of Drugs Act, which was passed in 1971. It is a product of its time, banning the running of premises where people smoked cannabis or opium. “There’s no law to stop you running a site where people inject heroin,” Stevens says. “Probably because they hadn’t thought about such a thing occurring.” But, as Krykant found, there are other offences that can be committed around a DCR, making it a legal “grey area”.
The UK government denies that the law around DCRs is a grey area, saying it is clear: “Anyone running [a DCR] would be committing a range of offences, including possession of a controlled drug and being concerned in the supply of a controlled drug.”
Olsen says there are other lessons that the UK could learn from Denmark. He cautions against going big and suggests that smaller units are better, especially if you can locate them in areas where there is already a service for people who use drugs.
The site that has been earmarked in Glasgow is next to an existing heroin-assisted treatment (HAT) facility, which has also been controversial. Hunter was involved in a 2015 public health needs assessment of the Glasgow public-injecting population. “The two recommendations that have had a lot of publicity are heroin prescribing, and the drug consumption rooms,” she says. HAT provides prescription heroin to dependent users for whom other opioid substitution treatment has not worked. Users come to a clinic once or twice a day and inject a prescribed dose of heroin under supervision. There is evidence that HAT reduces use of illicit heroin, thus decreasing demand and undermining the illegal drugs market, and reduces criminal activities used to fund drug use[5]
. “A lot of the people that would use a drug consumption room would be ideal candidates for heroin-assisted treatment,” Krykant says.
No silver bullet
Emmert Roberts, an addiction researcher at King’s College London, says that there has been “massive disinvestment” in drug and alcohol services since 2012. He thinks that, although DCRs would form a “useful part of a cohesive drug strategy in the UK”, they should not be looked at as “an isolated thing”.
We understand that it’s not a silver bullet — we need a range of different treatments
The key, Stevens argues, is a ‘person-centred approach’. He sees the role of DCRs as “providing an entry point into comprehensive treatment services”. Krykant agrees: “We understand that it’s not a silver bullet — we need a range of different treatments.”
Roberts, who has been heading up the London initiative to get the homeless off the streets during the coronavirus pandemic, believes that the pandemic itself may be providing an opportunity to get people into treatment. Anecdotally, he says, he and others have noticed that “people who probably haven’t been in treatment for 20 years are starting to come into treatment because they’ve had such a reduction in the supply of opiates”. This is because of a mixture of supply chain disruption and the economic impact of COVID-19. Of course, that does not mean that they will stay in treatment, especially since COVID-19 has forced some treatment online and limited numbers in other facilities.
Ultimately, no one disagrees that the UK, and especially Scotland, is doing a terrible job at preventing drug deaths. The question is what do we need to do differently. DCRs, if nothing else, are something we have not yet tried. And, despite a UK government spokesperson telling us there are “no plans to introduce drug consumption rooms”, Stevens says there are encouraging signs of political movement, citing the fact that members of both the UK Labour and Conservative parties have comes out in favour of DCRs.
Olsen, who has seen time and again how hard it is for countries to introduce DCRs, has some simple advice: “We’ve been doing the same stuff for 30 years. Let’s try something else.”
References
[1] National Records of Scotland. 2019. Available at: https://www.nrscotland.gov.uk/statistics-and-data/statistics/statistics-by-theme/vital-events/deaths/drug-related-deaths-in-scotland/2018 (accessed December 2020)
[2] European Monitoring Centre for Drugs and Drug Addiction. 2019. Available at: https://www.emcdda.europa.eu/system/files/publications/11485/20193286_TD0319444ENN_PDF.pdf (accessed December 2020)
[3] Poschadel S, Höger R, Schnitzler J & Schreckenberg D. 2003. Available at: https://d-nb.info/966605268/04 (accessed December 2020)
[4] Salmon AM, van Beek I, Amin J et al. Addiction 2010;105(4):676–683. doi: 10.1111/j.1360-0443.2009.02837.x
[5] Transform Drug Policy Foundation. 2017. Available at: https://transformdrugs.org/wp-content/uploads/2020/07/HAT-Briefing-2017.pdf (accessed December 2020)
You may also be interested in

London’s first drug-checking service could expand to more cities

Voice of the Voiceless: co-produced materials to help reduce stigma for people receiving opioid substitution treatment in pharmacies
