Shutterstock.com
Learning outcomes
At the end of this case study, you will be able to:
- Outline the pathophysiology, signs and symptoms, and diagnosis of bacterial conjunctivitis;
- Describe the treatment options available for bacterial conjunctivitis;
- Outline the chemistry and mechanism of action of antimicrobial drugs used to treat conjunctivitis;
- Describe the factors to be considered when formulating eyedrops;
- Outline the factors to consider when prescribing topical products for pregnant patients.
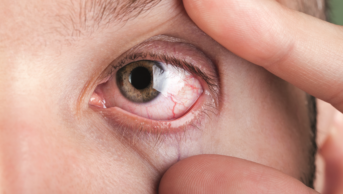
Mrs NC is 29 years old and 37 weeks’ pregnant. She is concerned about her left eye, which has been producing a yellow discharge that has stuck her eyelids together. She has been experiencing some discomfort in the affected eye but her vision is normal once the discharge has been blinked away. On observation, the entire conjunctival surface, including the tarsal plates (dense, fibrous tissues that give shape and support to the eyelids), appears red. Apart from the generalised redness there are no other abnormalities of the tarsal plates.
- What is conjunctivitis and what are the main causes?
- How can a bacterial cause of conjunctivitis be identified?
- Which patients or symptoms will necessitate referral to a GP?
Seven days later, Mrs NC returns to your pharmacy. She has a prescription for fusidic acid eyedrops, one drop twice daily, having phoned the GP to ask for some eyedrops because her condition persisted during the week.
- What treatment options are available for conjunctivitis?
- What are the formulation considerations for eyedrops?
- What additional factors have to be considered when treating pregnant women?
- Would chloramphenicol be safe to use in this patient?
Case discussion
Pathophysiology of conjunctivitis
Conjunctivitis is inflammation of the conjunctiva, the semi-transparent, highly vascularised mucous membrane that covers the globe of the eye, starting from the edge of the cornea (limbus), flowing back behind the eye, looping forward to form the inner surface of the eyelids (tarsal plates). The purpose of the conjunctiva is to decrease friction when blinking and to protect the sclera. The conjunctiva also prevents objects such as eyelashes or contact lenses sliding back behind the eye. As the conjunctiva is the final ocular layer, it is regularly exposed to the environment and hence subject to trauma, infection and allergic reactions, which can induce inflammation.
Establishing the cause of conjunctivitis
In cases of conjunctivitis, the whole of the conjunctiva will be involved (the globe and the tarsal plates) and so all surfaces should show redness. Where the redness is localised to just the limbus, another structure is affected and requires investigation. There will be generalised mild discomfort and ocular irritation; the presence of pain indicates involvement of the cornea and forms part of the differential diagnosis.
Discharge or increased lacrimation is generally the key to diagnosis for the most common causes of conjunctivitis. A thick yellow purulent discharge that can stick eyelids together in the morning indicates a bacterial origin. This cause is more common in infants and children than in adults. A more watery discharge is associated with viral conjunctivitis. Cases of viral conjunctivitis may also be distinguished by a recent flu-like illness, conjunctival follicles (small semi-translucent lymphatic swellings), lid oedema and excessive lacrimation. This type of conjunctivitis is more common in adults than in children. The most common causative agent is adenovirus; the others implicated to a much lesser extent are the Coxsackievirus and picornavirus. Viral conjunctivitis is very contagious and other people in close contact are likely to be affected. There can also be serious consequences with some patients developing keratoconjunctivitis, which affects vision.
Allergic conjunctivitis is not associated with any discharge, but will be associated with increased bilateral lacrimation. Itching will predominate with eyes appearing more pink than red. There may also be some degree of conjunctival swelling or ballooning (chemosis). Most patients presenting with allergic conjunctivitis at the pharmacy will do so with acute presentations and will have a history of contact with an allergen towards which the response is mounted, e.g. pollen, mite allergens. During the hay fever season it is termed ‘seasonal allergic conjunctivitis’. Chronic allergic conjunctivitis may be present all year long. It commonly affects boys with a history of atopy (genetic disposition towards allergic disease). The chronic nature of this condition means there may be more changes in the eye: follicles or white spots in the limbal region, papillary (raised, ‘bumpy’) lesions on the upper tarsal plate or punctate lesions (tiny white spots) on the corneal epithelium.
Chlamydial conjunctivitis caused by the obligate intracellular organism Chlamydia trachomatis is the least common type of conjunctivitis. Discharge can vary between watery and mucopurulent (containing mucus and pus), but the redness of the conjunctiva is deeper than seen with other causes. Raised follicles will be seen on the lower tarsal conjunctiva as well as symptoms of systemic infection. Patients are screened for chlamydial antigens to confirm diagnosis.
Bacterial cases requiring referral
Although most cases of bacterial conjunctivitis are easily diagnosable in the community pharmacy, not all patients will be candidates for over-the-counter (OTC) treatment. The following patients will need referral to a doctor:
- Patients who are producing copious amounts of purulent discharge that reaccumulates quickly when wiped away, or infection that is not localised to the eye, because this indicates severe infection.
- Patients experiencing pain within the eye, which indicates corneal involvement needing investigation.
- Patients with loss of vision, indicating severe infection or other structures affected.
- Patients who have had surgery or laser treatment in the last 6 months because they will require examination of the surgical site before treatment.
- Contact lens wearers who are more prone to eye infections and more likely to become infected with Pseudomonas aeruginosa, which can go on to cause corneal ulceration, endophthalmitis (inflammation of the interior of the eye) and even permanent blindness.
- Patients who have failed to respond to initial topical antibiotic treatment, indicating that the antibiotic was not active against the causative organism.
- If the patient is pregnant or breastfeeding because exposure of the child to medication must be considered.
Treatment options for conjunctivitis
Often, in bacterial conjunctivitis, no pharmacological treatment is necessary because the condition is usually self-limiting and will resolve within 7–10 days. Good hygiene is important to reduce transfer to the unaffected eye; this includes removing any possible contaminated eye makeup. The use of eye bathing or sterile wipes to refresh the eye and remove discharge can help to reduce some symptoms. Often, patients will want some treatment in the form of a topical antibiotic. In the case of children, treatment may be requested by the nursery or school in order for the child to return to interaction with other children and prevent spread.
As well as bacterial conjunctivitis being more common in infants and children than adults, there is a difference seen in the probable causative organism. In adults the causative organisms are Staphylococcus aureus (55%), Streptococcus pneumoniae (20%), Moraxella sp. (10%), Haemophilus influenzae (5%) and Pseudomonas aeruginosa (5%), whereas in infants and children the most common bacteria are S. pneumoniae, M. catarrhalis and H. influenzae. Despite the differences in organisms, both groups have Gram-positive and Gram-negative bacteria implicated, so, when treating bacterial conjunctivitis, agents with a broad spectrum of activity are used.
Chloramphenicol 0.5% eyedrops are considered to be first-line treatment for bacterial conjunctivitis because it is broad spectrum with activity against both Gram-positive and -negative bacteria. It exerts its bacteriostatic effect by selectively inhibiting protein synthesis in ribosomes. Although considered the gold standard and effective for almost all cases of bacterial conjunctivitis, it is not active against Pseudomonas aeruginosa or Chlamydia trachomatis, so those patients who have not responded to treatment require immediate referral. Despite its effectiveness, OTC supply is prohibited to those who are aged <2 years or already using products for glaucoma or dry eye syndrome, have a personal or family history of bone marrow problems (because of the link to aplastic anaemia) or take medication that may interact with chloramphenicol eyedrops.
In these patients, however, propamidine isetionate (isethionate) 0.1% eyedrops (Brolene eyedrops) could be supplied OTC. Propamidine is an aromatic diamidine (R-C[NH]NH2) antibacterial disinfectant that is active against Gram-positive bacteria, but less active against Gram-negative bacteria; it also has limited antifungal properties. It blocks the permease transport system that is responsible for the uptake of purine nucleotides. Bacteria are therefore unable to synthesise the precursors for DNA, RNA or protein metabolism. Other less well-known interactions add together to give its bacteriostatic effect.
Failure of OTC products necessitates referral to a doctor. Further investigation to determine the cause of the infection may be required and cultures taken. Before culture results are obtained, other broad-spectrum antibiotics would be prescribed such as ofloxacin (a fluoroquinolone), which can interfere with bacterial DNA replication, or fusidic acid (derived from the fungus Fusidium coccineum), a complex steroid-like molecule (no steroid activity), which acts by inhibiting bacterial protein synthesis.
Formulation of eyedrops
To ensure that topical ophthalmic preparations are non-irritant, they are formulated to have properties approximating to those of lacrimal fluids (tears), have the appropriate viscosity and include an antimicrobial preservative if a multi-dose presentation is required (to prevent growth of microorganisms accidently introduced into the product during use).
Isotonicity: hypotonic and hypertonic solutions are irritant to the eye and thus hypotonic ophthalmic solutions (similar to many injections) are made isotonic by the addition of tonicity agents, such as sodium chloride, dextrose and buffer salts.
pH: the pH of tears is approximately neutral. Tears have some buffering capacity, and weak acids and bases, pH range 3.5–9 can be tolerated in the eye. Buffers may be included, such as borate and phosphate buffers.
Viscosity: water-soluble, viscosity-enhancing polymers, such as methyl cellulose and hydroxypropyl methylcellulose, may be included in formulations to increase their viscosity, prolonging retention of the drug in the eye and thereby increasing drug absorption.
Antimicrobial preservatives: antimicrobial agents with a broad spectrum of activity against Gram-positive and -negative bacteria, yeasts and moulds, and with low toxicity to humans, are required for multiple-use eyedrops, which may be accidently contaminated during use. The number of antimicrobial agents suitable for ophthalmic use is very limited, with benzalkonium chloride being the most commonly employed.
Fusidic acid is formulated as viscous eyedrops (fucithalmic) in a preserved aqueous system containing the polymer carbomer. The viscous formulation is easy to administer, and the polymer-containing formulation, which liquefies and becomes transparent on contact with the tear fluid, gives an increased precorneal residence time and sustained levels of the drug, compared with a conventional eyedrop formulation.
The decision to include any excipient within the formulation must take into account compatibility with the drug and the container.
Ocular treatment in pregnancy
As with other minor ailments in patients who are pregnant, treatment initially will always tend towards conservative management with non-pharmacological therapies; this is to reduce the risk of exposing the unborn child to medicines and their metabolites. Despite the therapy in this case being topical, there is some systemic absorption of ocular products, hence their ability to cause systemic side effects. Medicines in ocular products penetrate the cornea, entering the aqueous fluid, which drains from the eye via the canal of Schlemm (circular canal at the sclerocorneal junction of the eye, draining aqueous humour from the anterior chamber into the conjunctival veins). In addition, some product will end up in the gastrointestinal tract because it may drain via the nasolacrimal duct into the nasopharynx. Pharmacokinetic data on the amount of systemic absorption from ocular products are lacking. This, coupled with the lack of human data on the exposure of fetuses to topical ocular products, means that there are few published data on the potential for fetotoxic events of topical ophthalmic medications.
Many ocular medications have also been used systemically to treat conditions in pregnant women and have not produced evidence of birth defects above the normal background rate. Therefore, if a medication is not known to produce defects systemically, then it is not likely to do so topically due to the smaller amounts administered. Careful consideration is needed when prescribing medication and each patient must still be considered on a case-by-case basis.
Even topical therapies will be subject to the same considerations: what is the severity of the infection? What are the potential consequences of not treating the mother? What is the potential toxicity to the fetus of the drugs under consideration?
Choice of treatment in this case
In this case, conservative treatment has failed, and not treating the mother may lead to further ocular involvement and invasive infection. Which agent should be used?
A broad-spectrum agent is be required, so chloramphenicol would be a good choice. However, despite there being no published data on any associated risk of congenital malformation, there have been concerns that use near term is associated with grey baby syndrome. Because of this concern, the UK teratology information service advises that the use of chloramphenicol in pregnancy should be avoided where possible. In selecting a therapy that is believed to be the safest, fusidic acid is a potential alternative, for which the manufacturers state that it can be used in pregnancy.
Extended learning
- How can the systemic absorption of ocular products be reduced?
- Outline how eyedrops are packaged and sterilised
- What is ophthalmia neonatorum?
- How should allergic conjunctivitis be treated?
- What considerations should be taken when advising on topical dermatological preparations for pregnant patients?
- What is grey baby syndrome?
- How would you counsel the patient to administer the eyedrop product?
- This article was adapted from Integrated Pharmacy Case Studies, published by Pharmaceutical Press.
You might also be interested in…
Identification and management of common eye disorders
Glaucoma: an overview