Science Photo Library
This is the first in a series of articles designed to help pharmacy teams support patients who are experiencing joint pain or patients who have been diagnosed with osteoarthritis (OA) and may benefit from recommendations for appropriate management strategies, including the wide range of products available in pharmacies.
More information on joint pain management can be found in our next guide in the series ‘Pharmacy guide to joint pain: management‘.
Read more about our joint pain partnership and find related content on our Pharmacy Learning Centre.
Joint pain
Joint pain is the main symptom of many different musculoskeletal conditions, including all types of arthritis, connective tissue disease and osteoarthritis (OA). Most joint pains are described as mechanical or activity-related, meaning they are associated with morning stiffness and the pain gets worse with increasing and continued use as the day goes on[1].
Mechanical pain of any joint that persists for at least three months, with or without loss of function of the joint, is defined as a chronic condition[1].
In the UK, the most common cause of mechanical joint pain is OA and it is estimated to affect a third of people aged 45 years and over[2].
Signs and symptoms of mechanical joint pain
Joints are dynamic environments and sites of continual growth, degeneration and repair. As part of normal daily activities, joints are exposed to a constant low level of damage. In most cases, the body is able to repair the damage itself and no symptoms are experienced[3,4]. However, when symptoms of joint pain are experienced, they include:
- Joint pain that is worse with exercise and is relieved by rest (often worse at the end of the day);
- Stiffness that persists for less than 30 minutes in the morning and is common after inactivity;
- Enlarged (bony) joints;
- Reduced range of joint movement;
- Crunching (also known as crepitus) of the joint when moving[4].
OA arises as a result of the failure of normal replacement and regrowth in the joints; the protective cartilage at the joint ends breaks down and bony growths can also develop, causing pain, swelling and problems with moving the joint[2]. It occurs most commonly in the hands, feet, knees and hip, but other joints can also be affected. OA can also occur in more than one joint at a time[3,4]. The most common site of joint pain encountered in community pharmacy is in the knee.
The impact of joint pain symptoms can go beyond physical health, and can include mental health problems and reduced quality of life. It is estimated that around 20% of patients with OA suffer from depression, and around 31–41% of patients with OA experience anxiety[5,6].
The impact of mechanical joint pain on daily activities varies between individuals and depends on the joint affected. For example, stairs can be problematic for those with knee or hip pain, while thumb pain can impact grip. Reduced joint movement may prevent an individual from working, which can lead to both financial difficulties and emotional stress. Joint pain may also lead the patient to experience sleep disturbances, which may impact on quality of life, contributing to, or worsening, symptoms, such as anxiety and depression[5,6].
Take note
Chronic pain is associated with anxiety and depression and these conditions can exacerbate the patient’s view of their symptoms.
Differential diagnosis
The symptoms of mechanical joint pain can occur in other conditions, which means that making a correct diagnosis can be challenging. Other conditions with similar symptoms include inflammatory arthritis (including gout and rheumatoid arthritis), fibromyalgia, neuropathic pain and malignancy[4].
However, inflammatory joint conditions are much less common, with gout and rheumatoid arthritis diagnosed in around 2.5% and 1.0% of the UK population, respectively[4]. For these conditions, the key to management is early detection and identifying any ‘red flag’ symptoms that would require referral to a GP or other specialist care.
If a patient presents to the pharmacy with symptoms of joint pain, there are several questions based on the WWHAM (see Box 1) and SOCRATES tools (see Box 2)[7,8], that pharmacy staff can ask to find out whether their symptoms may be related to mechanical joint pain.
Box 1: WWHAM — for use during initial conversations
W – Who is the patient?
W – What are the symptoms?
H – How long have the symptoms been present?
A – Action taken so far?
M – Medicines taken for anything else?
Box 2: SOCRATES — for evaluating the nature of symptoms
S – Site: Where exactly is the pain? What body part/joint is involved?
O – Onset: When did the pain start? Is it constant or intermittent? Gradual or sudden?
Progressive or regressive?
C – Character: What is the pain like? An ache? Stabbing? Sharp? Burning? Tight?
R – Radiation: Does the pain radiate or move elsewhere?
A – Associations: Are there any other signs or symptoms associated with the pain
(e.g. sweating, vomiting, temperature)?
T – Time course: Does the pain follow any pattern? Is it constant or does it happen at any time of
the day? How long does it last? When does he/she feel the most pain?
E – Exacerbating/relieving factors: Does anything change the pain? What makes the pain better
or worse? Sometimes, a specific physical position or medicine can relieve the pain.
S – Severity: How bad is the pain? The patient should be asked to give a number to describe the pain
on a scale of 0–10, where 0 is the lowest and 10 is the most severe pain experienced.
Pharmacy teams should be aware of symptoms and terms to listen out for when speaking to patients in order to correctly identify and classify the type of joint pain being experienced. The following questions, in addition to enquiring about the patient’s age, medications and allergies, are designed to help gather information related to joint pain symptoms[9,10]:
- When during the day do you experience joint pain and how long does it last?
Joint pain or stiffness experienced first thing after rising in the morning and persisting until the joints feel less stiff or ‘free up’ (generally fewer than 30 minutes in duration) indicates mechanical joint pain or OA. With OA, morning stiffness can typically last 5–10 minutes, while for tendonitis in the hands it may be 30 minutes. Any stiffness that persists longer than 30 minutes requires referral to a GP because it may be caused by inflammation.
Take note
If joint stiffness is present all day, this means there is no morning stiffness.
- How quickly has your joint pain or stiffness developed over time?
Gradual worsening of symptoms over a period of months does not warrant referral to a GP. However, rapidly worsening joint pain over days or weeks requires medical review.
- Do you have hot, swollen joints?
Presence of hot swollen joints indicates that inflammation may be present and requires referral to a GP (see Box 3).
- Have you experienced any fever or unexplained weight loss?
Any systemic upset experienced by the patient alongside their joint pain or stiffness is a red flag and the patient should be referred to a GP.
- Have you had a recent injury?
If a patient is experiencing pain or stiffness that occurs hours or a day after trauma, such as a sports injury or minor injury, the pain can usually be managed in the pharmacy with simple pain-relief medicines, rather than referring the patient for immediate medical review. For pain that occurs immediately after trauma, patients should be referred for immediate medical review, typically at a hospital and emergency department. If pain from an old trauma does not respond to simple pain relief, again patients should be referred for medical review.
- Do you have any other medical conditions?
Patients who have previously been diagnosed with cancer and are experiencing joint pain or stiffness should be referred promptly for medical review.
Box 3: Red flag symptoms
Some symptoms should be regarded as ‘red flag’ symptoms. In these cases, patients should be referred to a GP or acute NHS walk-in centre. These symptoms include:
- A joint or limb that looks deformed with associated pain;
- A joint that is too painful to move or cannot bear weight;
- Severe swelling, discolouration, red, hot joints or bleeding;
- Persistent joint pain, tenderness or swelling;
- Prolonged or severe morning stiffness;
- Tingling or numbness;
- Sudden or severe pain;
- Anyone who is taking any type of medication;
- A suspected fracture, dislocation, rupture or another serious injury;
- Hot, swollen joints;
- Rapid worsening of symptoms;
- Systemic upset and a history of trauma or cancer[9].
Using the questions above, pharmacy staff can determine whether symptoms are likely to be caused by mechanical joint pain or if the patient needs to be referred for another condition. If symptoms are mild and are likely to be caused by mechanical joint pain, pharmacy teams can provide patients with both lifestyle and pharmacological advice.
Take note
Pain is subjective and can be difficult to manage, therefore it is important to use a person-centred approach[10]. Patients may prefer to have an initial conversation in a consultation room, as this will give them privacy and a more relaxed environment in which to answer questions compared with the busy pharmacy shop floor[9].
Risk factors for mechanical or activity-related joint pain
The following factors may increase the risk of developing mechanical joint pain:
- Age — OA is more common in patients aged 45 years and over;
- Obesity;
- Smoking;
- Gender — OA is often more common and severe in women, especially in the knee and hand joints;
- Joint injury — repetitive movements or earlier injuries to joints can often lead to the development of OA in later life;
- Jobs that involve standing for long periods of time or heavy lifting;
- Family history/genetic factors[11].
How does mechanical joint pain affect specific joints?
Symptoms of mechanical joint pain can vary and often build up over time rather than appearing suddenly. The effect of symptoms on people’s lives depends on which joints are affected and how severely they are affected.
The ways in which OA may affect different parts of the body include:
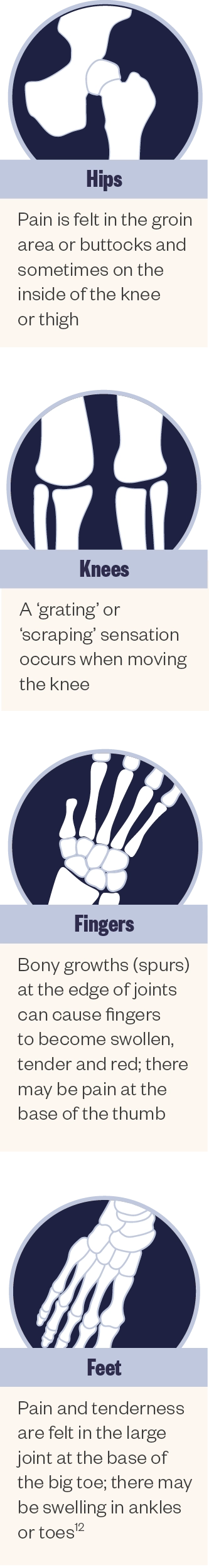
When can pharmacy staff help?
Community pharmacy teams may be able to help patients who come into the pharmacy in the following circumstances:
- If a patient has already received a diagnosis of OA and is looking for advice and relief of symptoms of joint pain;
- If a patient is experiencing the symptoms for the first time, they may require advice and temporary relief of symptoms;
- If a patient has experienced the symptoms before and has previously trialled over-the-counter preparations.
Since a diagnosis of OA is based on signs and symptoms and the elimination of any ‘red flag’ causes of pain, with enough information, community pharmacy teams can distinguish between this and possible inflammatory arthritis. X-rays are not required for a diagnosis of OA.
READ MORE: Pharmacy guide to joint pain: management
- 1Osteoarthritis: care and management in adults. National Clinical Guideline Centre, London 2014.
- 2Osteoarthritis in general practice. Versus Arthritis. http://www.arthritisresearchuk.org/arthritis-information/data-and-statistics/~/media/EFAEFCE432734F3AA5FB1C64329E02D1.ashx (accessed Feb 2019).
- 3Joint pain: pathology and treatment. The Pharmaceutical Journal Published Online First: 2019. doi:10.1211/pj.2019.20206108
- 4Clinical guideline – Osteoarthritis: care and management. National Institute for Health and Care Excellence. https://www.nice.org.uk/guidance/cg177/chapter/1-Recommendations#diagnosis-2 (accessed Feb 2019).
- 5Musculoskeletal conditions and multimorbidity. Versus Arthritis. https://www.arthritisresearchuk.org/policy-and-public-affairs/policy-reports/multimorbidity.aspx (accessed Feb 2019).
- 6State of musculoskeletal health 2018: arthritis and other musculoskeletal conditions in numbers. Versus Arthritis. 2018.https://www.arthritis researchuk.org/arthritis-information/data-and-statistics/state-of-musculoskeletal-health.aspx (accessed Feb 2019).
- 7Paul R. Community Pharmacy: symptoms, diagnosis and treatment. 4th ed. London: : Churchill Livingstone 2017.
- 8Macleod J, Munro J, Edwards C. SOCRATES. 14th ed. Edinburgh: : Churchill Livingstone 2017.
- 9How to conduct an effective joint pain management consultation in a community pharmacy setting. The Pharmaceutical Journal Published Online First: 2019. doi:10.1211/pj.2019.20205870
- 10Appropriate community pharmacy management and referral of patients with chronic peripheral joint pain. The Pharmaceutical Journal Published Online First: 2019. doi:10.1211/pj.2019.20205710
- 11Conditions: Osteoarthritis. Versus Arthritis. https://www.versusarthritis.org/about-arthritis/conditions/osteoarthritis (accessed Feb 2019).