Science Photo Library
Open access article
The Royal Pharmaceutical Society has made this article free to access in order to help healthcare professionals stay informed about an issue of national importance.
To learn more about coronavirus, please visit: https://www.rpharms.com/resources/pharmacy-guides/wuhan-novel-coronavirus
Convalescent plasma has no benefit for patients with COVID-19 who are severely ill and in intensive care, according to early findings from the ‘Randomised, Embedded, Multifactorial, Adaptive Platform trial for Community-Acquired Pneumonia’ (REMAP-CAP) trial.
So far, 912 severely ill trial participants in intensive care had received the treatment, but an initial analysis of trial data showed that, overall, convalescent plasma was unlikely to be beneficial, with a very low probability (2.2%) that it improved the chances of decreasing the number of days requiring intensive care support or death by more than 20%.
Although there was no evidence of harm associated with the administration of the treatment, enrolment of severely ill COVID-19 patients in intensive care to the convalescent plasma arm of the trial has been halted.
Hospitalised COVID-19 patients, who are moderately ill but do not require intensive care, will continue to be recruited to the trial as the initial analysis did not assess the effect of convalescent plasma in these patients.
“Although it is disappointing that all critically ill patients don’t appear to gain any benefit [from convalescent plasma], this is still vitally important to know,” said Anthony Gordon, professor of anaesthesia and critical care at Imperial College London and UK chief investigator of the REMAP-CAP trial.
“Convalescent plasma is a precious resource, and we can now continue to focus on identifying exactly which patients might benefit the most from treatment – maybe people earlier in their illness or those with weak immune systems,” he added.
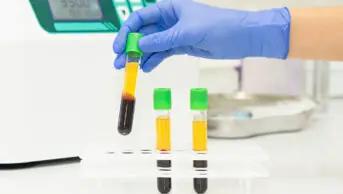
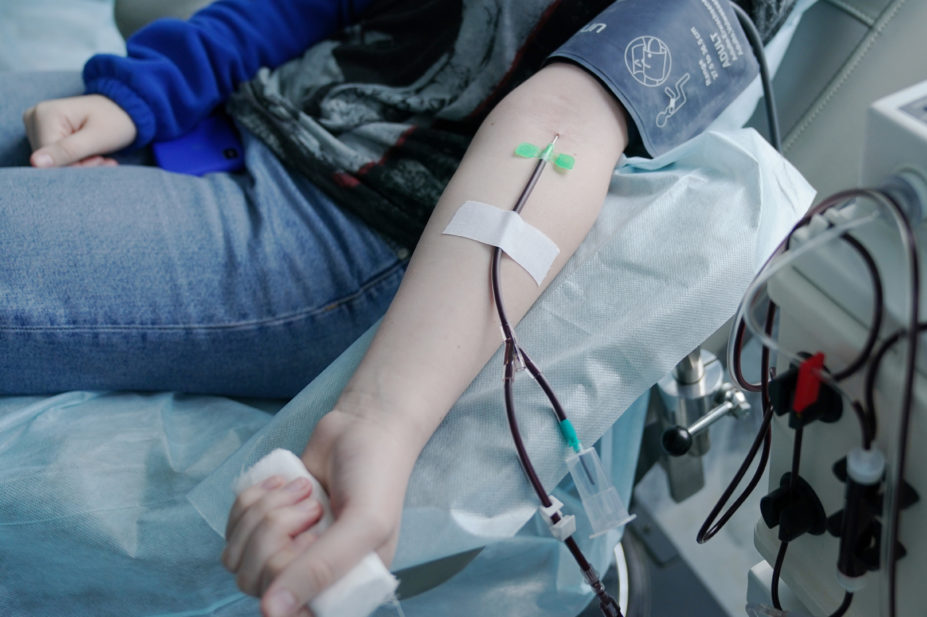
The underlying hypothesis for using convalescent plasma, which is taken from the blood of people who have recovered from COVID-19, is that the antibodies it contains could neutralise the virus, stopping it from replicating and halting tissue damage.
“Why convalescent plasma does not seem to improve outcomes in severely ill COVID-19 patients admitted to the ICU [intensive care unit] is not yet known. However, it may be because the lung damage is too advanced for convalescent plasma to make a difference,” said Alexis Turgeon, a critical care doctor and professor at Université Laval in Canada, who is also working on the trial.
The REMAP-CAP investigators now await a more complete analysis based on data from more than 2,000 severely ill patients recruited in the trial, including if any subgroups of patients derived benefit from this treatment.
“It is biologically plausible that patients who are not producing antibodies at the time of convalescent plasma therapy and those patients with excess virus may benefit more than others,” explained Manu Shankar-Hari, a clinician and professor of critical care medicine at Guy’s and St Thomas’ hospital, London, who is co-leading the trial. “Our additional analyses will explore this,” he added.
A randomised controlled trial published in the New England Journal of Medicine on 6 January 2021, suggested that early administration of convalescent plasma, with high titers of antibodies against SARS-CoV-2 (the virus that causes COVID-19 infection), to infected older adults — within 72 hours after the onset of mild symptoms — reduced the progression of COVID-19 to severe illness by 48%.
A total of 160 older adult patients underwent randomisation within 72 hours after the onset of mild COVID-19 symptoms. The researchers found that severe respiratory disease developed in 13 out of 80 patients (16%) who received convalescent plasma and 25 out of 80 patients (31%) who received placebo (relative risk, 0.52; 95% confidence interval, 0.29 to 0.94; P =0.03).