Shutterstock.com
After reading this article, you should be able to:
- Understand the epidemiology, pathophysiology and complications of chickenpox to counsel patients and prevent the spread of infection;
- Explain the signs and symptoms of chickenpox, including how to differentiate chickenpox from other skin conditions;
- Describe the current prevention and treatment options for chickenpox, including vaccination, antiviral medications and symptomatic relief measures.
Introduction
Chickenpox, also known as varicella, is a highly contagious viral infection that is caused by the varicella-zoster virus (VZV). Chickenpox is a common childhood illness; in the UK, approximately 90% of people have had chickenpox by the age of 15 years[1]. The chickenpox vaccine is not part of the routine childhood immunisation schedule in the UK, but it is available privately and recommended for those who are at risk of severe infection[1,2].
In the UK, there are around 300,000 cases of chickenpox each year, with the majority of cases occurring in children under the age of 10 years; it is most common in children aged 1–4 years[3]. Chickenpox is contracted through inhalation of airborne respiratory droplets from an infected individual[4]. Outbreaks are more common in the winter and spring months, and tend to occur in nurseries, schools and other close-knit settings. While chickenpox is usually a mild illness, it can lead to more serious complications in certain groups of people, such as pregnant women and people who are immunocompromised. Chickenpox can be contracted more than once, but this is rare.
Pharmacists play an important role in the management of chickenpox. They can provide advice on symptom relief, appropriate use of antiviral medications for those at risk, and vaccinations for those who have not had chickenpox or who are at risk of infection, such as people who are immunocompromised.
Signs and symptoms
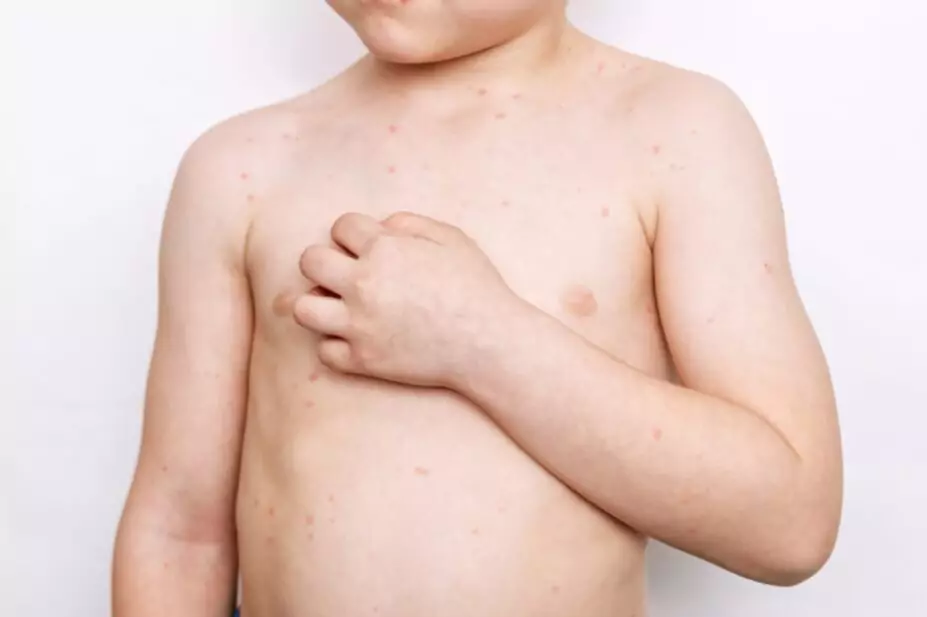
Chickenpox usually appears as a rash all over the body, starting with itchy, red bumps that turn into fluid-filled blisters, and finally scabs. The rash typically lasts 5–10 days, usually appearing 10–21 days after exposure to VZV[5]. New spots can appear while others are blistering or forming a scab[4]. The rash may appear more widespread in adults, and the fever may be prolonged in comparison with children.
Risk factors for severe disease and complications include pregnancy, immunosuppression and respiratory disease. Symptoms indicating complications include:
- Shortness of breath;
- Cough;
- Chest pain;
- Persistent or recurrent fever;
- Reduced urine output;
- Confusion;
- Reduced level of consciousness[6].
Red-flag symptoms include pneumonia, encephalitis, dehydration, high temperatures or severe secondary bacterial infection of the skin; patients experiencing these should be referred to hospital.
Pathophysiology
Stage 1
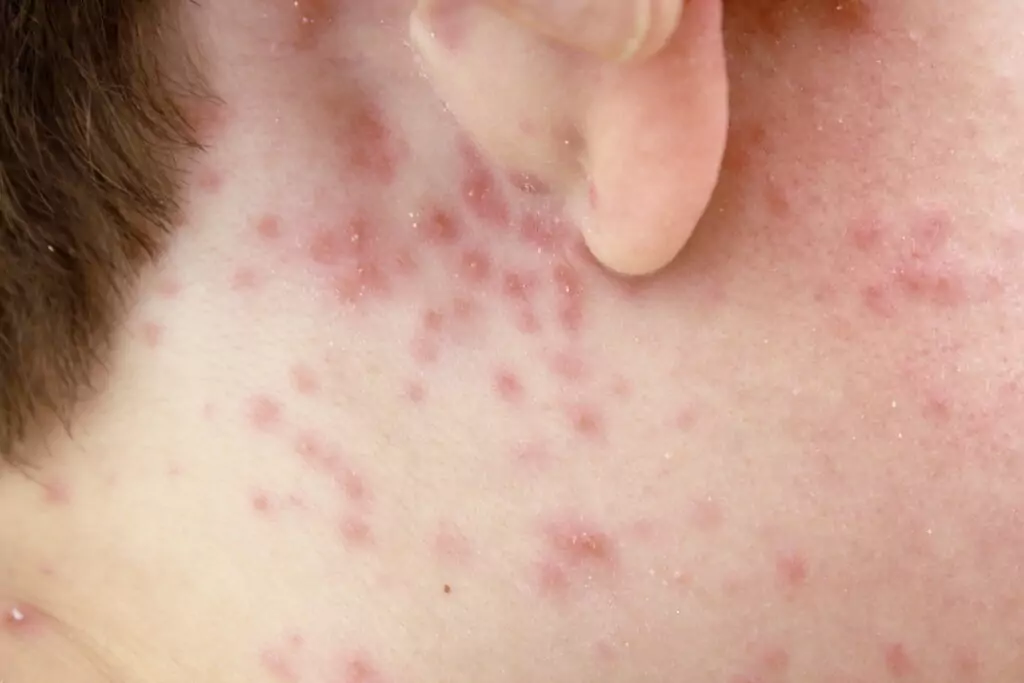
Small spots begin to appear on the skin and can spread or stay in a small area. They usually begin on the chest, back and face and can spread over the entire body, including the mouth, eyelids and genital areas[3,7]. The appearance of the spots can be red, pink, darker than, or the same colour, as the surrounding skin, depending on skin tone (see Figure 1). The redness seen in chickenpox can be less visible on darker skin tones[3].
Shutterstock.com
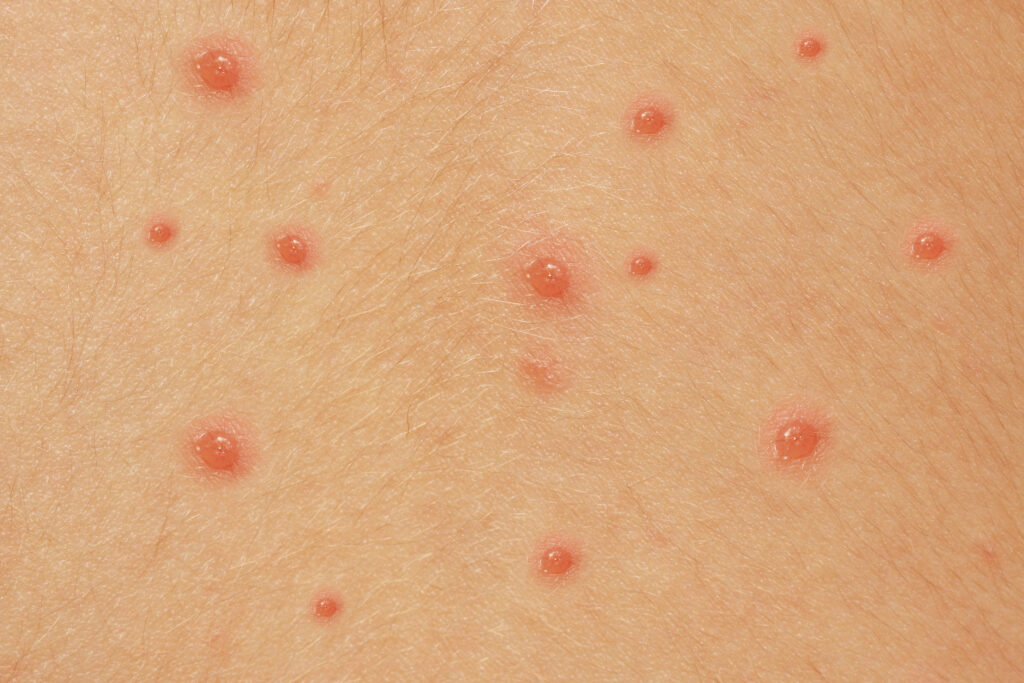
Stage 2
Spots become blisters that are very itchy and may burst (see Figure 2)[3]. These last about a day before they pop and start to leak[5].
Shutterstock.com
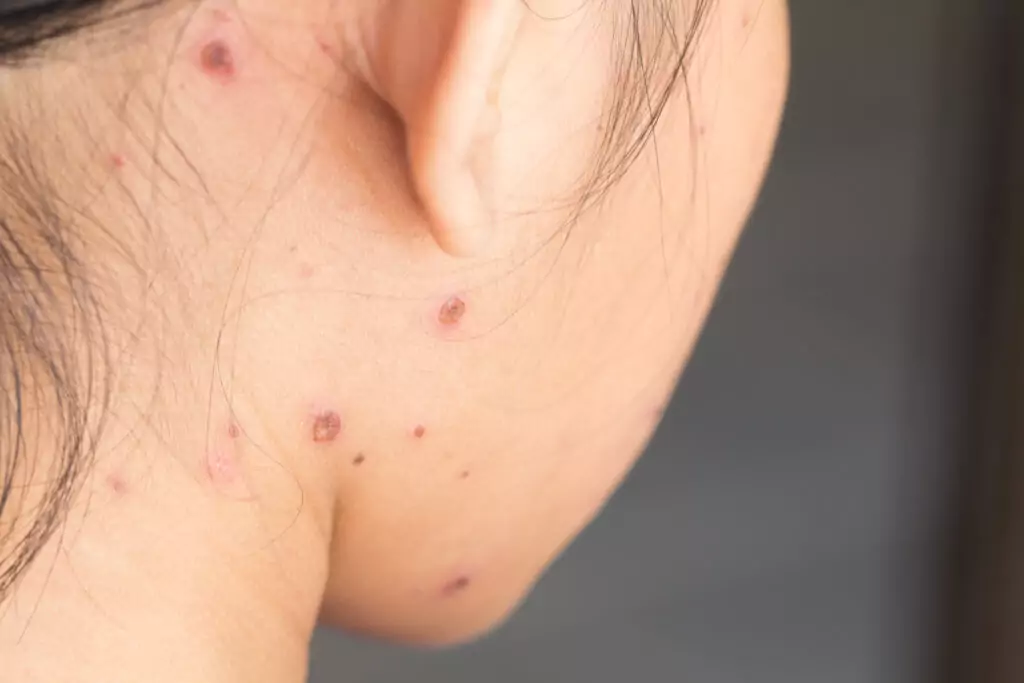
Stage 3
The blisters become scabs. Some may flake and still leak fluid (see Figure 3)[3].
Shutterstock.com
Diagnosis
Depending on the patient’s age and the severity of the symptoms, patients and their carers may seek help from a variety of healthcare settings. These can include the local community pharmacy for over-the-counter (OTC) remedies, general practice and urgent care or the emergency department. As chickenpox usually presents as a rash, a diagnosis can be made clinically from characteristic symptoms. When there is uncertainty about the diagnosis, in addition to the symptoms, other methods are used to confirm diagnosis, including:
- History — previous chickenpox infection, recent exposure to chickenpox or shingles or history of chickenpox vaccination;
- Laboratory testing — in severe cases or when diagnosis is uncertain, a sample from the blister is taken and tested for the presence of VZV[6,7].
Chickenpox is usually easy to distinguish. However, it can be confused with other viral rashes and infections, such as scabies, impetigo, and syphilis. It can also be mistaken for similar skin conditions, such as shingles, which is caused by the same virus as chickenpox. Although it looks very similar, shingles usually only presents on one side of the body.
Management
Chickenpox is usually self-limiting for adults and children, taking one to two weeks to clear from the body; therefore, drug treatment is not advised unless certain criteria are met. Symptoms can be alleviated with both OTC products and self-care options. OTC treatments include paracetamol for pain relief (if the patient is over two months of age), calamine lotion to soothe the skin, and oral antihistamines to reduce itchiness (if over one year of age)[8–10]. Ibuprofen is not recommended in chickenpox, as there is an increased risk of severe skin and soft-tissue infection[11,12].
Chickenpox can be worrying for parents; therefore, they should be advised on self-care management to help alleviate symptoms. Pharmacists can advise on the best OTC treatment options for individuals, depending on symptoms and age, and can educate parents to help distinguish between normal symptoms and red-flag symptoms (see the signs and symptoms section). The most infectious period is within 24 hours of rash onset and can last up to 5 days[6].
Box: Self-care for chickenpox: dos and don’ts
Dos:
- Do ensure plenty of fluids are given to avoid dehydration;
- Do dress in loose, cotton clothing to avoid overheating, shivering and skin irritation;
- Do keep nails short to minimise damage from scratching and secondary bacterial infection from scratching;
- Do bathe in cool water and pat the skin dry with a towel.
Don’ts:
- Don’t give aspirin to children aged under 16 years;
- Don’t have contact with newborn babies (aged four weeks and under), pregnant women and people with a weakened immune system, as chickenpox can be dangerous for them;
- Don’t scratch the spots, as this can cause scarring;
- Don’t go to school or work until all vesicles have crusted over to avoid spreading the infection;
- Don’t cold-sponge a child who has a fever as the blood vessels under the skin can constrict if the water is too cold, which reduces heat loss and can trap heat in deeper parts of the body, worsening the fever[7,13,14]
Treatment
Aciclovir is a synthetic nucleoside analogue that inhibits replication of VZV, reducing fever and chickenpox symptoms if started within 24 hours of onset[15]. Aciclovir shortens the duration and reduces the number of vesicles, and is most effective when started as soon as possible after the onset of the rash[15]. In immunocompromised individuals, treatment should begin within 24 hours of onset of the rash[15]. The UK Health Security Agency advises aciclovir can also be used for post-exposure prophylaxis of varicella zoster infection, but it is not licensed for this indication.
The recommended oral dose of aciclovir for adults and children aged 12 years and over is 800mg, 5 times per day for 7 days. In children aged under 12 years, the oral dose varies according to age. The recommended intravenous dose is 5mg/kg every 8 hours for adults and children aged 12 years and over, or 10mg/kg intravenously every 8 hours if these patients are immunocompromised[8,9]. For children aged under 12 years, prescribers should be aware that some intravenous doses are calculated either using mg/kg or mg/m2, depending on the age of the child[9].
Pharmacists should advise patients on adequate hydration, as aciclovir can cause severe dehydration. Common adverse effects include abdominal pain, nausea, skin reactions and vomiting[15]. Aciclovir should not be used for healthy individuals with uncomplicated chickenpox as these individuals will recover without treatment.
Special populations: pregnancy
Chickenpox in pregnancy is rare and only affects 3 in every 1,000 pregnant women; therefore, the likelihood of developing complications, such as pneumonia, hepatitis, maternal mortality, or serious morbidity, is very low. These complications are more likely and potentially more serious if the patient smokes, is immunocompromised or is more than 20 weeks pregnant[1,16].
There is also a risk to the baby, as chickenpox during pregnancy can lead to foetal varicella syndrome and varicella infection. The risks are greater the further into the pregnancy, particularly after 28 weeks[16].
Varicella zoster immunoglobulin (VZIG) is recommended for varicella zoster antibody-negative pregnant contacts exposed at any stage of pregnancy, providing VZIG can be given within ten days of contact[1]. Pregnant women and people with a positive history of chickenpox do not require VZIG[1]. Symptoms can be treated with paracetamol and calamine lotion, as these are licensed for use during pregnancy; however, chlorphenamine and ibuprofen should be avoided[17].
Special populations: immunocompromised patients
People who are immunocompromised are more at risk of severe, disseminated chickenpox with haemorrhagic complications, pneumonia, encephalitis, disseminated intravascular coagulopathy, and hepatitis[13]. The same self-care advice is recommended for this patient group; however, the dose of aciclovir for these adults is 10mg/kg intravenously every 8 hours, usually for 5 days[8].
Prevention advice
To prevent the transmission of chickenpox, the patient should stay away from school, nursery or work until all the spots have formed a scab. This is usually five days after the first spots appeared[1].
The chickenpox vaccination is available on the NHS only for people who are not immune to chickenpox and are in close contact with people at risk of becoming seriously ill if they catch it. Healthcare workers and laboratory workers who are not immune to chickenpox are also eligible for the vaccine. The vaccination is available privately in some community pharmacies. Of children vaccinated with a single dose, 90% will develop immunity against chickenpox; however, the vaccination is not as effective after childhood[1]. Only 75% of adolescences and adults become immune post vaccination[1].
There are currently two licensed chickenpox vaccines in the UK: Varilrix (GSK) and Varivax (Merck Sharp and Dohme)[1]. Both are live, attenuated vaccinations that should be taken four to eight weeks apart (two doses) for children aged over one year and adults. Although the vaccinations are usually well tolerated, some adverse effects can occur, such as pain, redness or a rash at the site of injection[8].
Prognosis
Most people who get chickenpox recover fully in one to two weeks; 90% of people recover completely and without any long-term consequences[7]. However, a person’s age and immune system can affect the severity of the illness[7,18]. Adults and those with compromised immune systems, for instance, tend to have more severe symptoms and a higher risk of complications[7].
Complications
Although complications from chickenpox are uncommon, they can be serious, especially in certain high-risk groups, such as pregnant women, newborn babies and people with compromised immune systems[7]. Bacterial skin infections are one of the most frequent complications of chickenpox[3,7]. If left untreated, bacterial infections can cause life-threatening conditions, such as necrotising fasciitis and cellulitis, as well as other serious health issues[19]. Chickenpox can progress to pneumonia, especially in adults or people with compromised immune systems[1,7].
Chickenpox can also cause permanent scarring and keloids, which is documented to occur in 7–18% of post-varicella patients[20]. There is anecdotal information that aloe vera, cocoa butter and oils can help with scarring, but there is no evidence to support this. Patients may chose to try non-invasive procedures, such as microdermabrasion and microneedling, or medical treaments, such as topical silicone gel sheeting, topical imiquimod, and topical tacrolimus and tretinoin cream[20]. Before the introduction of the chickenpox vaccine in the UK in 1995, an average of 20 deaths from chickenpox were reported annually[21]. The NHS reports that 347 hospital admissions for chickenpox occurred in 2018/2019, and one of those patients passed away[7]. The incidence of chickenpox has significantly decreased, and cases of the disease leading to death have become even more uncommon, since the vaccine was introduced[22].
Best practice tips for pharmacists:
- Counsel and advise patients and carers on appropriate use of over-the-counter medications, such as paracetamol and antihistamines, depending on the age of the patient and other relevant medical information (including pregnancy, other medications and medical history);
- Ensure that ibuprofen and/or aspirin are not used as part of the management of chickenpox unless advised by a medical professional;
- Advise individuals not to scratch, as this can cause bacterial infections and scarring. Itching can be reduced by keeping the skin clean, donning gloves or mittens, and taking cool baths or compresses.
- Ensure that individuals, families and carers know that the infected person should wash their hands regularly and avoid contact with people who are immunocompromised to stop the virus from spreading;
- Advise the individual to seek medical attention if symptoms are severe or persist for more than a week, or if there are any concerns with medication therapy.
- 1Varicella: the green book, chapter 34. UK Health Security Agency. 2019.https://www.gov.uk/government/publications/varicella-the-green-book-chapter-34 (accessed Jun 2023).
- 2Bedford H, Lingley-Heath N, Lai J, et al. 455 Varicella vaccine: acceptability and preferences for administration by UK parents. British Paediatric Allergy Immunity and Infection Group. 2022. doi:10.1136/archdischild-2022-rcpch.329
- 3Chickenpox. NHS. 2021.http://www.nhs.uk/conditions/chickenpox (accessed Jun 2023).
- 4Lopez A, Harrington T, Marin M. Varicella. Centers for Disease Control and Prevention. 2021.https://www.cdc.gov/vaccines/pubs/pinkbook/varicella.html (accessed Jun 2023).
- 5What is chickenpox? WebMD. 2022.https://www.webmd.com/children/what-is-chickenpox (accessed Jun 2023).
- 6Chickenpox. National Institute for Health and Care Excellence. 2023.https://cks.nice.org.uk/topics/chickenpox/ (accessed Jun 2023).
- 7Chickenpox (Varicella). Centers for Disease Control and Prevention. 2021.https://www.cdc.gov/chickenpox/ (accessed Jun 2023).
- 8British National Formulary. MedicinesComplete. 2023.http://www.medicinescomplete.com (accessed Jun 2023).
- 9British National Formulary for Children. MedicinesComplete. 2023.http://www.medicinescomplete.com (accessed Jun 2023).
- 10Calamine Lotion BP. Electronic medicines compendium. 2016.https://www.medicines.org.uk/emc/product/4822/smpc (accessed Jun 2023).
- 11Quaglietta L, Martinelli M, Staiano A. Serious infectious events and ibuprofen administration in pediatrics: a narrative review in the era of COVID-19 pandemic. Ital J Pediatr. 2021;47. doi:10.1186/s13052-021-00974-0
- 12How and when to give ibuprofen for children. NHS. 2022.https://www.nhs.uk/medicines/ibuprofen-for-children/how-and-when-to-give-ibuprofen-for-children/ (accessed Jun 2023).
- 13Fever in under 5s: assessment and initial management. National Institute for Health and Care Excellence. 2021.https://www.nice.org.uk/guidance/ng143 (accessed Jun 2023).
- 14Chickenpox. Healthier Together. 2023.https://www.what0-18.nhs.uk/parentscarers/worried-your-child-unwell/chickenpox-new (accessed Jun 2023).
- 15Aciclovir 200 mg Tablets. Electronic medicines compendium. 2022.https://www.medicines.org.uk/emc/product/4334/smpc (accessed Jun 2023).
- 16Chickenpox in pregnancy. Royal College of Obstetricians and Gynaecologists. 2015.https://rcog.org.uk/media/y3ajgkda/gtg13.pdf (accessed Jun 2023).
- 17Best Use of Medicines in Pregnancy. Best Use of Medicines in Pregnancy. 2023.https://www.medicinesinpregnancy.org/ (accessed Jun 2023).
- 18Gershon AA, Breuer J, Cohen JI, et al. Varicella zoster virus infection. Nat Rev Dis Primers. 2015;1. doi:10.1038/nrdp.2015.16
- 19Shaikh N, Amara U, Hussein M, et al. Varicella Zoster Viral Infection Complicating into Necrotizing Fasciitis: A Case Report. 2022. doi:10.22541/au.166062628.86544867/v1
- 20Pour Mohammad A, Ghassemi M. Varicella-Zoster Scar Treatments: A Tertiary Review. Med. J. Islam. Republ. Iran. 2021. doi:10.47176/mjiri.35.136
- 21Rawson H, Crampin A, Noah N. Deaths from chickenpox in England and Wales 1995-7: analysis of routine mortality data. BMJ. 2001;323:1091–3. doi:10.1136/bmj.323.7321.1091
- 22Rawson H, Crampin A, Noah N. Deaths from chickenpox in England and Wales 1995-7: analysis of routine mortality data. BMJ 2001;323:1091–3. doi:10.1136/bmj.323.7321.1091
1 comment
You must be logged in to post a comment.


Stating chickenpox is self limiting in adults suggests it is not a real problem. However in many cases it can be an extremely painful and unpleasant experience for many adults and Acyclovir would shorten the period of these symptoms. In my experience most patients do not receive this product in time. No figure for deaths in adults in the UK from chickenpox is available but the U.S estimates 100-150 deaths per annum.A vaccine in the Uk for those adults who have not had chickenpox would seem a worthwhile step forward.