MEDICIMAGE / SCIENCE PHOTO LIBRARY
More patients could be considered for statin therapy to prevent cardiovascular disease (CVD) under updated draft guidelines from the National Institute for Health and Care Excellence (NICE).
The draft guidance, which is an update to existing guidance on risk assessment and reduction in cardiovascular disease, includes a new recommendation that statins can now be considered for people who have yet not had a CVD event — also known as primary prevention — and have a ten-year CVD risk score (QRISK3) of less than 10%.
NICE estimates that, with this new recommendation, for every 1,000 people with a QRISK3 score of 5% over the next ten years who take a statin, an average of 20 fewer people will get heart disease or have a stroke.
QRISK3 is an algorithm that calculates a person’s risk of developing a heart attack or stroke over the next ten years based on clinical variables and a variety of risk factors, such as type 2 diabetes mellitus and chronic kidney disease.
NICE previously recommended that statins prescribed for the prevention of cardiovascular events should only be offered to people with a QRISK3 of 10% or higher.
However, new evidence considered by the NICE guideline committee on the side effects of statins, suggests a wider group of people could be given them to achieve a greater reduction in CVD events overall, NICE said in a statement on 12 January 2023.
In August 2022, a study published in The Lancet found that only 1 in 15 reports of muscle pain or weakness by people taking statins could be attributed to the medication.
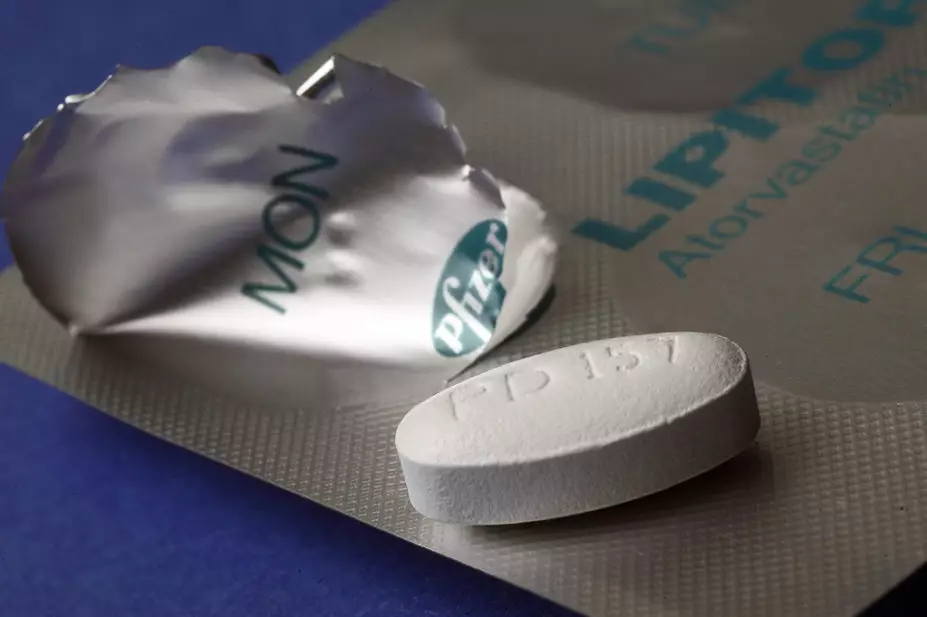
The draft guidance recommends that doctors consider atorvastatin 20mg for the primary prevention of CVD for people with a ten-year risk of less than 10% where there is “patient preference for taking a statin or concern that their risk may be underestimated”.
However, the guideline also says that, before offering statin treatment for primary prevention, prescribers should discuss the benefits of lifestyle changes and improve the management all other modifiable CVD risk factors, such as obesity and smoking.
The guidance adds that people at a higher risk should continue to be offered statins and more focus should be placed on increasing uptake among these people in order to have the most impact on CVD prevention.
Paul Wright, lead cardiac pharmacist for Barts Heart Centre at Barts Health NHS Trust, said the new recommendations were “great news” from a wider population perspective.
“It’s good to see cardiovascular disease prevention being looked at,” he said. “[However] it’s also very clear that this is not a ‘do’, this is an option.”
“It’s also clear that we need to consider, and be very mindful of, lifestyle changes, which will often have far greater impact than the addition of a statin — not smoking, reduced blood pressure and having a good, healthy, balanced diet.”
However, Wright said there was still a “massive gap” in the treatment of those at higher risk of CVD.
“For patients at high risk — with a QRISK3 over 10% — we already know that almost 50% of those are not on lipid therapy. What we should be doing is supporting and using resources to improve the QRISK3 of those over 10%, with the caveat that if you’re screening and they come up between 5% and 10%, you can have a conversation about considering to start the statin therapy.”
Paul Chrisp, director of the Centre for Guidelines at NICE, said there was clear evidence that “for people with a risk of 10% or less over 10 years, statins are an appropriate choice to reduce that risk”.
“We are not advocating that statins are used alone. The draft guideline continues to say that it is only if lifestyle changes on their own are not sufficient, and that other risk factors, such as hypertension, are also managed, that people who are still at risk can be offered the opportunity to use a statin, if they want to.”
Chrisp added that it was the responsibility of GPs to explain the ways in which people can reduce their risk of CVD, presenting all the options promoted by the draft guidance, including lifestyle changes, blood pressure control, avoidance of diabetes and cholesterol lowering, and allowing patients to make their own decisions.