Shutterstock.com
Open access article
The Royal Pharmaceutical Society has made this article free to access in order to help healthcare professionals stay informed about an issue of national importance.
To learn more about coronavirus, please visit: https://www.rpharms.com/resources/pharmacy-guides/wuhan-novel-coronavirus
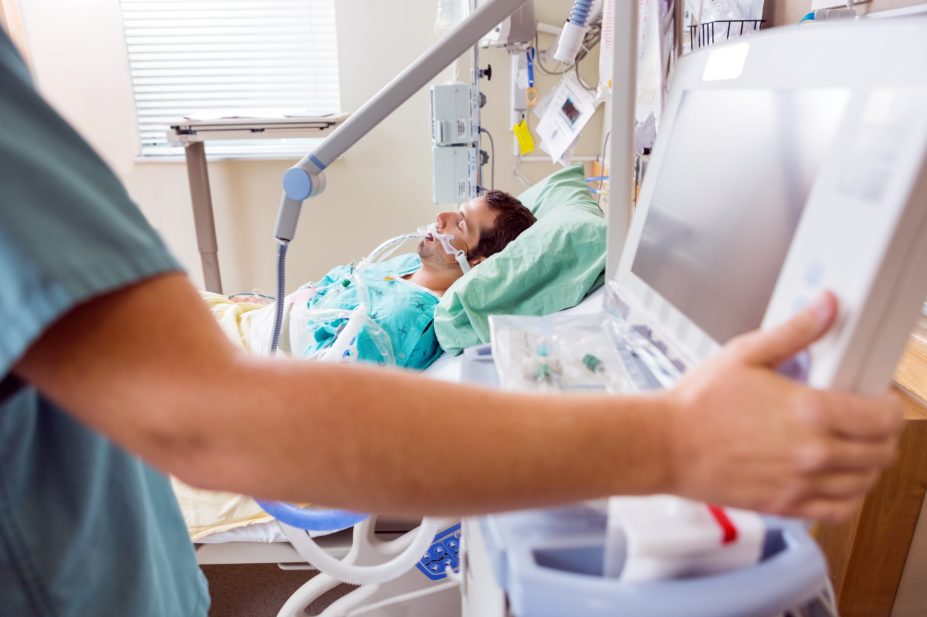
Source: Shutterstock.com
The drug tocilizumab could reduce mortality and time spent in intensive care for COVID-19 patients
The rheumatoid arthritis drug tocilizumab significantly improves outcomes for critically ill patients with severe COVID-19, potentially reducing mortality and time spent in intensive care, early findings from the Randomised, Embedded, Multi-factorial, Adaptive Platform Trial for Community-Acquired pneumonia (REMAP-CAP) have suggested.
Researchers on the trial said that they have released the findings ahead of peer review because of the clinical implications of the results for patients, but are looking to analyse and publish them as soon as possible.
The international REMAP-CAP platform trial, which started investigating potential COVID-19 treatments in March 2020, is being carried out in 15 countries across Europe and has involved more than 2,000 hospitalised patients with either moderate or severe COVID-19.
Using data from the first 303 patients randomised to receive either of the immune modulation treatments tocilizumab, sarilumab, anakinra, interferon or no immune modulator, researchers estimate that there is a 99.75% probability that tocilizumab is superior to no immune modulation, with an estimated odds ratio of 1.87.
The trial does not yet know the relative benefits of tocilizumab compared to the other immune modulators and further data are expected in the coming months.
The latest analysis was carried out by a statistical analysis committee separate from the trial investigators and reviewed by an independent Data and Safety Monitoring Board on 17 November 2020.
“These early findings show that treatment with this immune modulating drug is effective for critically ill COVID-19 patients in intensive care units,” said Anthony Gordon, chief investigator of the study.
“When we have the results available from all participants, we hope our findings will offer clear guidance to clinicians for improving the outcomes of the sickest COVID-19 patients.”
Lennie Derde, a consultant in intensive care medicine at the University Medical Center in Utrecht, described the results as “absolutely amazing”.
“To have a second effective therapy for critically ill patients within months of the start of the pandemic is unprecedented. Specific targeting of the immune response is theoretically attractive, and now we have shown it works.”
The analysis also suggested that lopinavir/ritonavir was ineffective and provided no additional benefit to critically ill COVID-19 patients, compared with those who did not receive the drug.
The latest findings on tocilizumab and lopinavir/ritonavir add to earlier REMAP-CAP findings, which found that hydrocortisone steroid treatment improved recovery among critically ill COVID-19 patients.
REMAP-CAP continues to evaluate other treatments, including therapeutic anticoagulation, antiplatelet agents, apremilast, eritoran, anakinra, sarilumab, vitamin C, simvastatin, convalescent plasma, macrolides and antibiotics.