FDA
The US Food and Drug Administration (FDA) has approved a treatment for leukaemia that uses a patient’s own genetically altered cells.
The therapy, known as CAR T-cell therapy and marketed as Kymriah by Novartis, is the first gene therapy to gain approval in the United States.
“Kymriah is a first-of-its-kind treatment approach that fills an important unmet need for children and young adults with this serious disease,” said Peter Marks, director of the FDA Center for Biologics Evaluation and Research.
“Not only does Kymriah provide these patients with a new treatment option where very limited options existed, but a treatment option that has shown promising remission and survival rates in clinical trials.”
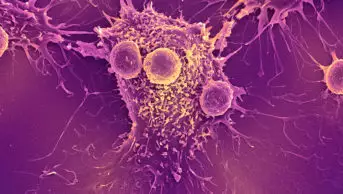
The therapy will be available to some children and adults up to the age of 25 with refractory or twice-relapsed B-cell precursor acute lymphoblastic leukaemia (ALL).
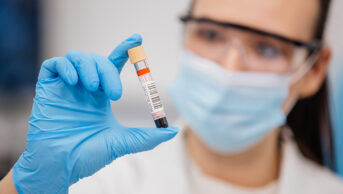
To create the therapy, T-cells are harvested from the patient, frozen and sent to a Novartis manufacturing centre. There the cells are genetically modified to incorporate a receptor gene that allows them to target an antigen found on leukaemia cells, known as CD19. The cells are then allowed to multiply before they are transferred back to the patient via a one-off infusion.
In clinical trials the treatment was tested in 63 paediatric and adult patients, where a complete remission rate of 83% at three months was observed. The probability of being relapse-free and survival at six months were 75% and 89%, respectively, during the 8.8-month median follow-up, but long-term survival and remission rates are unknown.
The treatment will be available only at certified medical centres owing to the risk of potentially life-threatening cytokine release syndrome (CRS) and medical staff must be trained to deal with these reactions. This includes administering tocilizumab, an immunosuppressive rheumatology drug that can treat the condition and in the trial led to 69% recovery rate from CRS within two weeks after one or two doses.
Fifteen percent of patients in the trial also experienced a severe neurological event.
Other side effects included serious infections, hypotension, acute kidney injury, fever, and hypoxia.