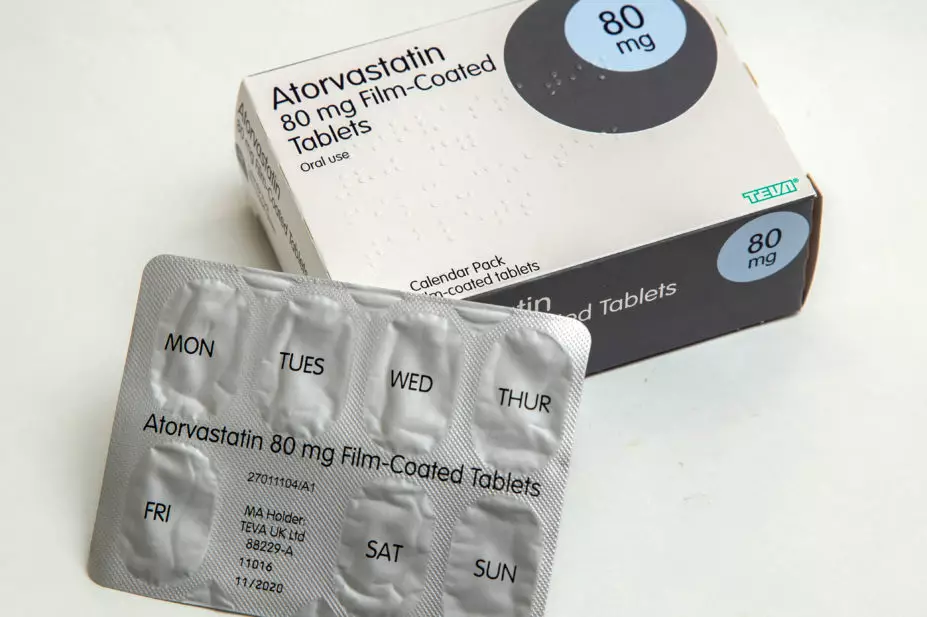
Photo Central / Alamy Stock Photo
NHS England and NHS Improvement (NHSE&I) is exploring three possible models for making high-dose statins available in community pharmacies without a prescription, including possible reclassification, The Pharmaceutical Journal has learned.
Meeting minutes, obtained via a freedom of information request, show that NHSE&I has been hosting discussions with bodies, including the Medicines and Healthcare products Regulatory Agency (MHRA) and National Pharmacy Association (NPA), to look at three different routes to making high-dose statins available in community pharmacies without a prescription.
These include a prescription-only medicine (POM) to pharmacy (P) medicine switch and use of patient group directions (PGDs).
In a meeting held with the NPA in September 2020, NHSE&I stated that a POM-to-P switch would increase accessibility for patients and support the initiation of statins. However, it highlighted that this would not necessarily be in keeping with long-term disease management, and raised concerns about testing and monitoring of patients.
The minutes said the PGD route could face problems because of pharmacist access to the summary care record and communication with GPs, but could fit in well after an NHS Health Check has been carried out.
A third model supports continuation and optimisation of statins, and would ensure pharmacists were working at “the top of their licence”, the minutes said.
The British Medical Association (BMA) was also involved in discussions, with minutes showing that it was generally positive about the proposals to make high-dose statins available in community pharmacies without a prescription, as long as it does not lead to an increase in GP referrals.
Representatives from the BMA said that there was a need for baseline blood tests before initiating statins and questioned whether community pharmacists would be responsible for doing this.
Ultimately, the BMA said that a “robust protocol” needed to be in place and that “if done well” the scheme could support GPs.
In discussions held with the Association of the British Pharmaceutical Industry (ABPI), the primary consideration for a POM-to-P switch was patient safety, and that the risk of harm increase the higher the dose.
The ABPI representatives said that the MHRA would need sufficient evidence of the benefit for patient populations and appropriate training should be put in place before agreeing to a classification change.
In an NHSE&I meeting with the MHRA in August 2020, it was suggested that the PGD route could be better as each company would be able to provide training material to help pharmacists “get up to speed” with the product.
“The biggest challenge of a P medicine is you can not enforce care record and training … if it becomes a P [medicine] it can be supplied from any pharmacy,” the MHRA representative said in the meeting, adding that safety was a “critical component” of switching from POM to P. “Cost saving would be secondary to this,” they added.
A spokesperson for NHSE&I said its review of high dose statins had been delayed by the COVID-19 pandemic and was still ongoing.
Read more: High dose statins could be supplied without a prescription through community pharmacies.


