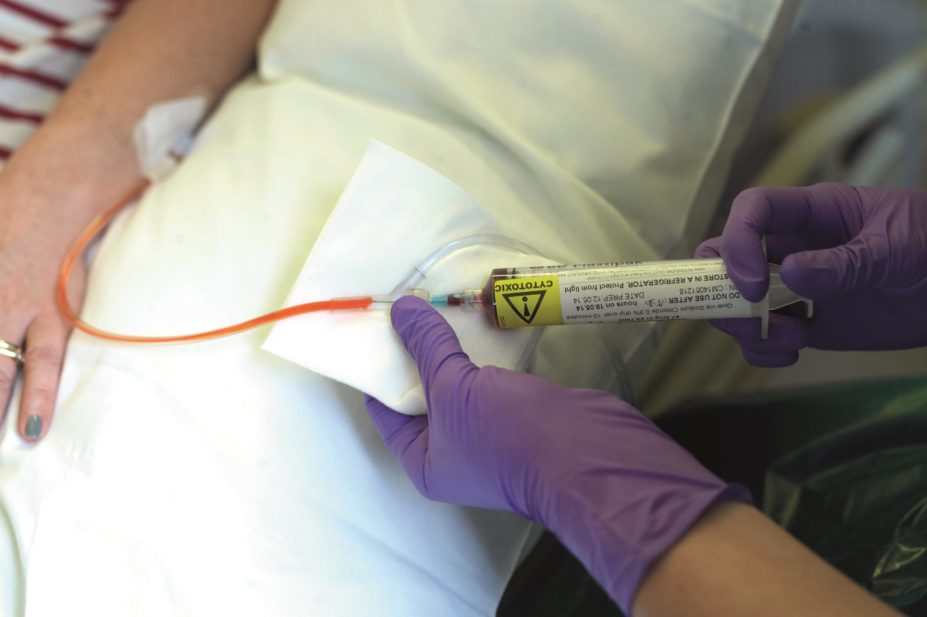
Lifestyle Photographer / Alamy Stock Photo
The Cancer Drugs Fund (CDF) has not been managed properly by NHS England and the Department of Health (DH), a committee of MPs says. The fund’s budget has been repeatedly overspent and there has been no assessment of what impact the fund has had on patient outcomes, according to the MPs.
The CDF was established in 2010 to improve access to cancer drugs not routinely available on the NHS because they had yet to be recommended by the National Institute for Health and Care Excellence (NICE), and to address geographical variations in the availability of specific cancer drugs.
However, in a report published on 5 February 2016 MPs on the Public Accounts Committee (PAC) say that while about 80,000 people have received drugs through the fund, the DH has not been able to assess the impact on patient outcomes, such as extending patients’ lives, or demonstrate whether the fund is a good use of taxpayers’ money.
The PAC says it is unclear how far regional variations in access have been reduced, adding that “there is no assurance that the DH and NHS England are using their buying power effectively to pay a fair price for cancer drugs”.
“Half of the patients supported by the fund received drugs that had previously been appraised but not recommended by NICE because they did not meet its clinical and/or cost-effectiveness thresholds,” the report says. “In this respect the fund has cut across, rather than complemented, the work of NICE.”
The fund’s budget grew from £175m in 2012–2013 to £416m in 2014–2015, an increase of 138% in two years, with the fund’s budget for 2013–2014 and 2014–2015 being overspent by a total of £167m, the report says. However, NHS England did not start to take action to control the cost of the fund until November 2014.
Burgeoning costs mean that the fund is not sustainable, so NHS England and NICE are currently consulting on proposals to reform the fund from April 2016. The consultation closes on 11 February 2016.
“We expect NHS England… to take account of our recommendations and apply the clear lessons from the last five years to ensure that the new fund is managed better in the future,” the report says.
These recommendations include setting clear objectives for what the reformed fund aims to achieve; for NHS England to “be prepared to take tough decisions to ensure that the fund does not overspend”; and for the DH to “set out how it ensures that it pays a fair price for drugs”.
In terms of assessing the impact of the fund, the report says that NHS England should report back to the PAC by June 2016 “on what the available data indicate about the impact of the fund on patient outcomes”.
The PAC adds that the issue of whether NICE has the capacity to appraise all new cancer drugs within the proposed timeframes also needs to be addressed “as a matter of urgency”.
Meg Hillier, chair of the PAC and MP for Hackney South and Shoreditch, says: “There must be confidence that public money is being spent on the right medication, and at a fair price. We will be closely monitoring the progress made by the department and NHS England in the months ahead.”

Source: NICE
Sir Andrew Dillon, chief executive at the National Institute for Health and Care Excellence (NICE), says NICE has considered the effect of proposals for a reformed cancer drugs fund on the institute’s workload and resources
Responding to the report, Sir Andrew Dillon, chief executive at NICE, says the proposals being consulted on set clear objectives about how the fund will be managed and that NICE has considered the effect of the proposed new arrangements on its workload and resources. “Funding has been agreed with NHS England,” he says. “When these proposals are finalised NICE and NHS England will work together to put in place a new system to provide patients with promising medicines at a fair price.”
A spokesperson for NHS England welcomed the committee’s support for a redesigned fund, but says: “We hope their explicit call for cuts to cancer drugs prices charged to the CDF will be borne in mind as complex decisions on its future are taken in the next few months.”
Cancer charities also welcomed the report’s recommendations. Sally Greenbrook, policy manager at Breast Cancer Now, says it is “particularly pleasing” to see the report’s focus on price negotiations.
“[This is] something we feel has been missing from the current NICE and NHS England proposals,” she says, adding that the current proposals do not go far enough.
Mark Flannagan, chief executive of the charity Beating Bowel Cancer, says opportunities have been missed to collect data to demonstrate the impact of individual treatments on patients’ lives. “It’s vital that this is fixed.”