Science Photo Library
Open access article
The Royal Pharmaceutical Society has made this article free to access in order to help healthcare professionals stay informed about an issue of national importance.
To learn more about coronavirus, please visit: https://www.rpharms.com/resources/pharmacy-guides/wuhan-novel-coronavirus
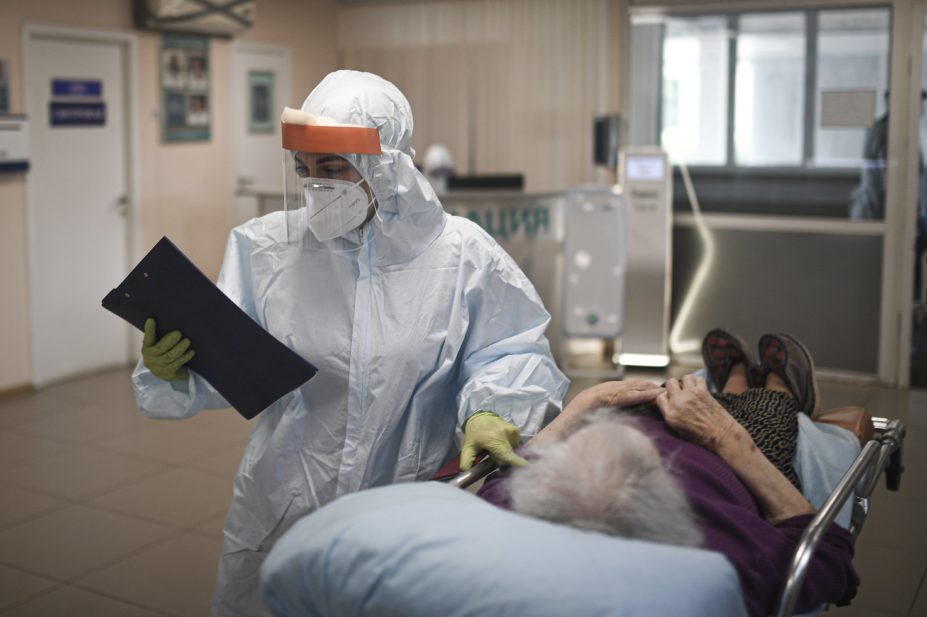
Source: Science Photo Library
Severly ill patients with COVID-19 are likely to see better outcomes when treated with hydrocortisone
Patients with severe COVID-19 who are treated intravenously with the steroid hydrocortisone are up to 93% more likely to have a better outcome compared with patients who are not given the drug, principal findings from a major COVID-19 trial published in Journal of the American Medical Association
have suggested.
The results, which were from the ongoing Randomized, Embedded, Multifactorial Adaptive Platform Trial for Community-Acquired Pneumonia (REMAP-CAP) trial, are one of three sets of results, published on 2 September 2020 in JAMA, that suggest steroids improve survival of the sickest COVID-19 patients.
As a result, the World Health Organisation has said it will be issuing new guidelines to include the use of steroids to treat critically ill COVID-19 patients.
Some 403 patients with suspected or confirmed COVID-19, who required respiratory or cardiovascular organ support, were enrolled in the hydrocortisone study between March 2020 and June 2020.
The patients, who were from the UK, Ireland, Australia, the US, the Netherlands, New Zealand, Canada and France, were randomly assigned to one of three different treatment regimes: 50mg hydrocortisone four times a day for seven days; shock-dependent dosing of hydrocortisone, if their blood pressure dropped; and no hydrocortisone.
The trial showed that using the fixed dose of hydrocortisone led to a 93% chance of a better outcome, including greater chance of survival and less need for organ support, than not using hydrocortisone.
In the group that were only given hydrocortisone when their blood pressure was low, the chance of a better outcome was 80%, compared with those who received no hydrocortisone.
However, the study was stopped early after results from the RECOVERY trial were released.
Gino Martini, chief scientist at the Royal Pharmaceutical Society, said that owing to the complexity of COVID-19 and its clinical manifestations, different drugs may be more or less useful at different stages of the disease and in different patient sub-groups.
“Hence the UK launched the RECOVERY [Randomised Evaluation of COVID-19 Therapy] and REMAP-CAP clinical trials, with the RECOVERY trial focusing on existing drug treatments, and REMAP-CAP aimed at identifying the best combination of treatments in critical care.
“So, today’s data is promising and very encouraging as the clinical trials have been conducted with appropriate controls and able to home in on the appropriate treatments and combinations,” he added.
Anthony Gordon, chair in anaesthesia and critical care at Imperial College London, consultant in intensive care medicine at Imperial College Healthcare NHS Trust, and lead of the UK arm of study, said: “At the beginning of the year at times it felt almost hopeless, knowing that we had no specific treatments.”
“Yet less than six months later, we’ve found clear, reliable evidence in high quality clinical trials of how we can tackle this devastating disease,” he added.
“The studies published today show that we now have more than one choice of treatment for those who need it most. Steroids are not a cure, but they help improve outcomes. Having a choice of different types of steroids, all of which seem to improve patient recovery, is great as it helps ease the problem of drug supply issues.”
A meta-analysis of seven randomised trials, including 1,703 patients, also published on 2 September 2020, concluded that 28-day all-cause mortality was lower among patients who received corticosteroids, including dexamethasone, hydrocortisone or methylprednisolone, compared with those who received usual care or placebo.
Overall, the researchers calculated that the risk ratio for all-cause mortality was reduced by 20% in those taking corticosteroids compared with those receiving usual care or placebo.
This, the researchers said, was equivalent to around 68% of patients surviving after treatment with corticosteroids, compared to around 60% surviving in the absence of corticosteroids.
Jonathan Sterne, professor of medical statistics and epidemiology at the University of Bristol and deputy director of the NIHR Bristol Biomedical Research Centre, said the meta-analysis was “good news”.
“Steroids are a cheap and readily available medication, and our analysis has confirmed that they are effective in reducing deaths among the people most severely affected by COVID-19. The results were consistent across the trials and show benefit regardless of age or sex.”
Martin Landray, professor of medicine and epidemiology at the University of Oxford and chief investigator of the RECOVERY trial, said: “The results are clear: among critically ill patients with COVID-19, low-dose corticosteroids such as dexamethasone significantly reduce the risk of death.”
“Since the emergence of COVID-19, the search has been on for treatments that can improve survival. Corticosteroids are inexpensive and widely available. This additional evidence of their efficacy is therefore particularly welcome as the treatments can be used to save lives worldwide.”