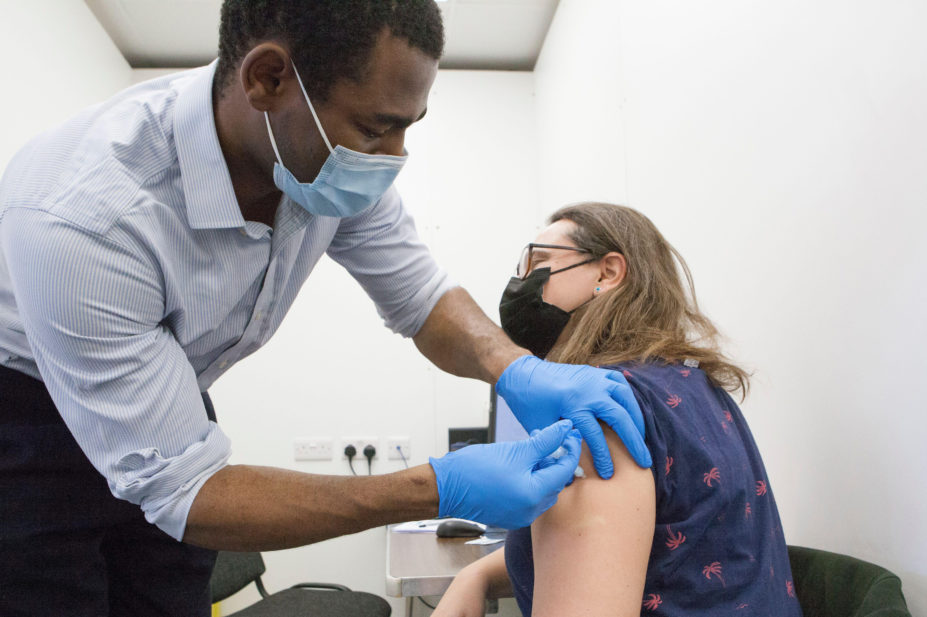
Anna Watson / Alamy Stock Photo
NHS England is allowing community pharmacies to provide “COVID-19 vaccinations only for a specified time” in an effort to maximise delivery of the vaccines through the sector, it has said.
In operational guidance dated 14 December 2021, seen by The Pharmaceutical Journal, NHS England said contractors leading COVID-19 vaccination sites must obtain approval to do this from their NHS England regional primary care commissioning team.
Requests to limit pharmaceutical services will receive “automatic agreement” if the contractor is proposing to implement this for “20% or less of the pharmacy contractors’ combined weekly core and supplementary hours and … at times of the day/week that will have the least impact on patients”.
“More than 20% of their combined weekly core and supplementary hours can be requested but this must be discussed and agreed with the regional commissioner in advance of the application being made,” the guidance says.
Contractors will need to give “at least 24 hours’ notice to limit pharmaceutical services” to receive automatic approval.
The guidance adds that pharmacy contractors must also “have a process in place to ensure that all patients retain access to their medicines, including provision of an emergency delivery service during hours of limited-service delivery”.
Pharmacy contractors will be able to claim £6 per delivery if a patient urgently needs medication “prior to the pharmacy contractor recommencing provision of full pharmaceutical services”.
This is the latest in a suite of measures to ease pressures on community pharmacy to facilitate an increase in COVID-19 vaccinations through the sector.
On 13 December 2021, NHS England advised all vaccination sites, including those led by community pharmacies, that they should remain open for 12 hours per day, 7 days per week to support plans “to offer every eligible adult over the age of 18 [years] a booster vaccination by 31 December [2021]”.
The new booster target was announced by prime minister Boris Johnson on 12 December 2021 in a prerecorded televised address, in light of the growing threat from the Omicron variant of COVID-19.
Pharmacy leaders subsequently said they were in “urgent talks” with the NHS on measures that could be implemented to help all contractors manage demand.
As a result of the talks, the Pharmaceutical Services Negotiating Committee (PSNC) announced on 15 December 2021 that it had reached an agreement with NHS England and the Department of Health and Social Care (DHSC) on several additional measures to help ease the immediate pressures on all community pharmacies, including those not delivering COVID-19 vaccines.
These include extending the deadline for meeting the requirements of the Pharmacy Quality Scheme from February 2022 to June 2022.
The DHSC also agreed to waive requirements for contractors to complete the Community Pharmacy Patient Questionnaire, the national audit and the required contractor-chosen clinical audit for 2021/2022.
This comes after pharmacy leaders called for ‘red tape’ to be cut to release time for COVID-19 booster jab delivery.
In response to the measures announced by the PSNC, Andrew Lane, chair of the National Pharmacy Association, said the changes were welcomed but added that “it’s very modest compared to the tremendous scale of the workload challenge posed by the Omicron wave”.
“NHS England should urgently consider a nationwide emergency supply scheme to reduce the time pharmacies spend chasing up prescriptions. This is already working in Cornwall as a local service and can be switched on elsewhere with minimal fuss,” he said.
“The requirement for pharmacies to check codes when people ask for lateral flow tests should also be suspended in light of the prevailing circumstances.”
Alastair Buxton, director of NHS Services at the PSNC, said he was “pleased to have agreed these measures which should help to reduce some of the workload for contractors in the coming weeks”.
“We know that for many community pharmacies they will not go far enough, and we are continuing to highlight to the NHS and government the huge amount of critical work going on in pharmacies — this is having a very positive impact on patients, the public and the NHS, but it is taking its toll on already exhausted pharmacy teams.”
Read more: COVID-19 booster campaign — everything we know so far


