Shutterstock.com
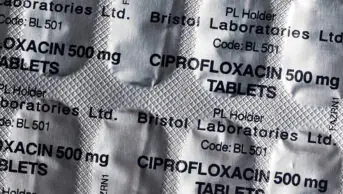
Efforts to reduce hospital prescribing of broad-spectrum antibiotics have been hindered by the COVID-19 pandemic, NHS England’s antimicrobial resistance (AMR) lead has said.
Kieran Hand, the national pharmacy and prescribing clinical lead for AMR at NHS England and Improvement, said that between 2017 and 2019, prescribing per hospital admission of certain broader-spectrum antibiotics fell by 5.5%.
However, speaking at the Clinical Pharmacy Congress on 13 May 2021, he said that this trend reversed between 2019 and 2020, when prescribing of these antibiotics increased by 3.6%, owing to increased use during the first and second waves of the pandemic.
Hand said that the prescribing trends relate to antibiotics included in the World Health Organization’s (WHO’s) ‘Watch’ and ‘Reserve’ lists, which were first drawn up in 2017 to help ensure the right antibiotics are used for the right infections.
Antibiotics on the ‘Watch’ list include those that are recommended as first- or second-line treatments for a small number of infections, while the ‘Reserve’ category includes those that should only be used in severe circumstances, when other options have failed.
The initial downward trend in hospital prescribing was counterbalanced by a 2.1% increase in prescribing from the ‘Access’ category of antibiotics, which the WHO says should be available at all times.
Hand said this was often owing to two narrow-spectrum agents being used to replace one broad-spectrum agent.
In January 2019, the UK government announced a five-year national action plan for AMR, which set a target for a 10% reduction in the use of Watch and Reserve antibiotics in hospitals from a 2017 baseline.
The increase in their use between 2019 and 2020 places the current reduction at around 2%; 8% away from the 2024 target.
Although Hand said the increased use of these antibiotics during the first and second waves of the pandemic was “of concern”, he added that the trend was expected to reverse as COVID-19 case numbers subsided.
In contrast, Hand said that the pandemic had accelerated progress to reduce antibiotic prescribing in primary care.
He explained that antibiotic prescribing in primary care has reduced by 30% since the baseline year of 2013–2014 — 5% ahead of the 2024 national action plan target of 25%.
The reductions in GP antibiotic prescribing during the pandemic had been made possible by a drop in the number of patients going to see their family doctor during this period, he said, particularly for conditions such as urinary and respiratory tract infections.
He added that before the pandemic, however, the downward trend had been achieved by various means, including the National Institute for Health and Care Excellence guidelines for managing common infections; public awareness campaigns; and the school influenza vaccination programme, which had led to a drop in respiratory infections and, consequently, amoxicillin prescribing.
Read more – Secrets of success: the hospitals slashing their antibiotic use