Dr P Marazzi / Science Photo Library
A study of more than 6 million people has revealed that repeated courses of antibiotics increase the risk of being diagnosed with inflammatory bowel disease (IBD), especially for people aged over 40 years.
The research, published on 9 January 2023, used Danish national databases, which included 6.1 million people aged over ten years without an IBD diagnosis. It revealed that having any course of antibiotics at any age increased the subsequent risk of being diagnosed with IBD.
People aged over 60 years, who had received five or more courses of antibiotics between January 2000 and December 2018, had an almost doubled risk of ulcerative colitis or Crohn’s disease (incidence rate ratio [IRR] 1.95, 95% confidence interval [CI] 1.85–2.04).
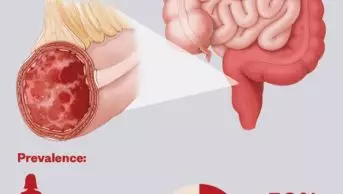
During the study, 52,898 cases of IBD were diagnosed, giving an overall prevalence of 0.9% in this population.
The study — initial results of which were first presented at the Digestive Disease Week 2022 conference — is the latest to look at whether antibiotics are a potential triggering factor for IBD, in part because they are known to change the gut microbiota.
The study results showed that, compared to people who had not been prescribed antibiotics, people aged 10 to 40 years had a 28% increased risk of IBD (IRR 1.28, 95% CI 1.25–1.32); people aged 40 to 60 years had a 48% increased risk (IRR 1.48, 95% CI 1.43–1.54); and people aged 60 years and over had a 47% increased risk (IRR 1.47, 95% CI 1.42–1.53).
The risk seemed to be cumulative, the researchers said, with each successive course of antibiotics increasing the risk by 11% to 14%, depending on age. The risk was time-linked, with each antibiotic course raising the risk for one to two years, after which risk declined again.
Commenting on the paper, Mohammed Allah-Ditta, advanced gastroenterology pharmacist with an interest in IBD medicines management at Calderdale and Huddersfield NHS Foundation Trust, said: “[This study] reinforces our knowledge that the microbiome is one of the factors in the development of IBD.”
He said that antibiotic stewardship is clearly important, but that the study raised questions about whether practice needed to change.
“One thing I would be thinking about is whether a patient has a family history of IBD — would that change practice about how liberally we prescribe antibiotics?” he asked.
When evaluating by antibiotic type, nitrofurantoin was the only class of antibiotics not found to be associated with the development of IBD across all age groups. The classes with the highest risk of IBD, across various age categories, were nitroimidazoles and fluoroquinolones, which are commonly used to target gastrointestinal pathogens.
Nominate an early-careers researcher today for the OPERA23 award
Help us in our search for outstanding early-career researchers who are accomplishing great things in pharmacy and pharmaceutical science.
For entry criteria and details on how to nominate a colleague, click here.