Oleg Elkov / Alamy Stock Photo
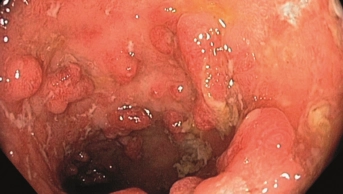
Use of antibiotics in older patients may be linked with the development of inflammatory bowel disease (IBD), according to a study due to be presented at the Digestive Disease Week 2022 conference.
An analysis of prescribing records from Denmark’s national medical records database suggested that the more antibiotics given in those aged 60 years and older, the greater the risk of an IBD diagnosis.
After one prescription, patients were 27% more likely to have a diagnosis, and with each additional course the risk grew, with those who had received five or more courses of antibiotics within five years being 2.3 times more likely to have new IBD recorded.
The analysis, which looked at new diagnoses in older patients between 2000 and 2018, found the risk was highest when the antibiotics were prescribed in the previous one to two years, but remained high even when going back two to five years.
All types of antibiotics showed the link with IBD, with the exception of nitrofurantoin, the US researchers reported. But those antibiotics usually prescribed for gastrointestinal infections were the most likely to be associated with a new IBD diagnosis, they added.
Lead researcher Adam Faye, assistant professor of medicine and population health at New York University Grossman School of Medicine, said the link they had found with antibiotic use could explain some of the growth in rates of Crohn’s disease and ulcerative colitis in older people.
“When you look at younger patients with new diagnoses of Crohn’s disease and ulcerative colitis, there’s generally a strong family history. But that is not the case in older adults, so it’s really something in the environment that is triggering it.”
He said that IBD can easily be overlooked in this age group when patients present with gastroenterological symptoms, but it should be considered, especially when there is a history of antibiotic prescriptions.
Faye added there were implications for judicious use of the drugs. “Antibiotic stewardship is important; but avoiding antibiotics at all costs is not the right answer either.
“If you’re not sure what you are treating, I would be cautious. If patients are coming in with clear infections, and they need antibiotics, they should not be withheld because of these findings.”
Commenting on the paper, Mohammed Allah-Ditta, advanced gastroenterology pharmacist with an interest in IBD medicines management at Calderdale and Huddersfield NHS Foundation Trust, said other work had shown a link between antibiotics in the first few years of life and later IBD.
“We know that if the microbiome in the gut is altered that plays a role in the onset of IBD and this is showing that in the elderly cohort.”
But he added it was difficult to take firm conclusions from a study that was looking at pre-diagnosis.
“It does enforce the message about the importance of antibiotic stewardship,” he said.
The paper is due to be presented at the Digestive Disease Week conference on 22 May 2022 in San Diego, California.
Read more: Inflammatory bowel disease: treatment and management