Shutterstock.com
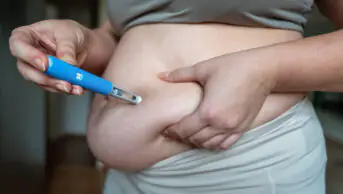
The type 2 diabetes mellitus (T2DM) drug semaglutide is effective for weight loss in non-diabetic, overweight or obese adults, when taken alongside a reduced-calorie diet and exercise, researchers have found.
A randomised controlled trial published in the New England Journal of Medicine on 10 February 2021, which was sponsored by Novo Nordisk, was conducted across 129 sites in 16 countries in Asia, Europe, and North and South America.
Researchers randomised 1,961 non-diabetic adults with either a body mass index (BMI) of 30 or greater, or a BMI of 27 or greater, with one or more weight-related coexisting conditions, in a 2:1 ratio to either 68 weeks of treatment with a weekly semaglutide injection (2.4mg) or placebo, plus lifestyle intervention.
All participants received individual counselling sessions every four weeks to help them adhere to a reduced-calorie diet and increased physical activity.
Overall, they found that participants who received semaglutide alongside lifestyle interventions had a mean weight loss of 14.9% from baseline, compared with a mean weight loss of 2.4% in the placebo group.
In addition, 86% of participants who received semaglutide, compared with 32% of those who received placebo, lost 5% or more of their baseline body weight, which the researchers said was a “widely used criterion of clinically meaningful response”.
“Weight loss with semaglutide stems from a reduction in energy intake owing to decreased appetite, which is thought to result from direct and indirect effects on the brain,” the researchers wrote.
“Weight loss with semaglutide was accompanied by greater improvements than placebo with respect to cardiometabolic risk factors, including reductions in waist circumference, blood pressure, glycated haemoglobin levels, and lipid levels; a greater decrease from baseline in C-reactive protein, a marker of inflammation; and a greater proportion of participants with normoglycemia,” they added.
They also highlighted that semaglutide improved physical functioning, which they said was “notable” given that being overweight or obese “significantly” impairs health-related quality of life.
Semaglutide is a glucagon-like peptide-1 (GLP-1) analogue that is approved for the treatment of T2DM in adults and for reducing the risk of cardiovascular events in persons with T2DM and cardiovascular disease.
Victoria Ruszala, a specialist diabetes pharmacist at North Bristol NHS Trust, said the results were to be expected considering the effectiveness of other GLP-1 drugs.
“Liraglutide has shown the same efficacy in its obesity trial and has just had a published NICE TAG [National Institute for Health and Care Excellence technology appraisal guidance] for this indication. Semaglutide is a more potent GLP-1 and therefore we would expect to see the same,” she said.
However, she said that semaglutide was the first drug to be seen to result in such a marked weight loss in participants.
“No other drug (including liraglutide) has been able to show anywhere near this. In practice, we often see slightly lower numbers as patients don’t receive the same psychological and dietetic support; however, even 10kg is a game changer. The DIRECT [Diabetes Remission Clinical Trial] trial showed that a weight loss of only 5kg had the ability to prevent development of T2DM, and those that lost 10kg were predominantly still in the non-diabetes range two years later.”
Ruszala said that her main question about the trial would be about the gastrointestinal side effects experienced by the participants.
“Due to the potency of semaglutide, we often find patients with T2DM struggle with this and need to be titrated much more slowly to avoid it. We only go up to a dose of 1mg in T2DM, so to see a 2.4mg dose — is there a much greater risk?”