Marina Demidiuk/Shutterstock.com
Amid ongoing measles outbreaks in London and the West Midlands, NHS England and the UK Health Security Agency (UKHSA) launched ‘Stay strong, get vaccinated’ on 16 February 2026 — a national campaign to encourage parents to get their children vaccinated.
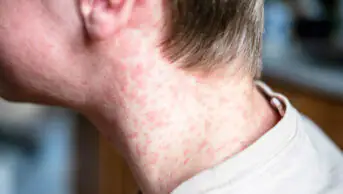
Childhood immunisation rates have been falling year on year for the past decade and in the case of measles — with around 1,000 cases in both 2024 and 2025 — it has resulted in the UK losing its elimination status again. In Enfield, north London, the vaccination rate for children aged under five years who received two MMR doses in 2024/2025 was 64% — well below the 95% threshold to suppress the measles virus and protect everyone from infection.
While parts of the current vaccination approach are effective, others are falling short. Without major reform of the current vaccination systems, healthcare professionals are fighting a losing battle, despite their best efforts.
Workforce pressures across the NHS have been particularly evident in primary care and, with GP surgeries overstretched, it is understandable there is less time to spend on prevention work, so it makes sense to look at other options. With further outbreaks inevitable, it is high time that community pharmacies are empowered to fully play their part.
There is plenty of evidence to show that community pharmacies improve vaccine uptake
Combating low vaccine uptake not only means addressing vaccine hesitancy and online misinformation, but also the reduced trust in scientific information and authorities that was fuelled by the COVID-19 pandemic. The factors behind low vaccine uptake are further confounded by health inequalities, deprivation and the make-up of the local population.
A report published by the Company Chemists’ Association (CCA) on behalf of the Pharmacy Vaccinations Development Group in February 2026 acknowledged that the variation in vaccine uptake nationwide can be explained by “poor access to healthcare” and “insufficient capacity in the healthcare system”, among other factors.
There is plenty of evidence to show that community pharmacies improve vaccine uptake. They are accessible, trusted by the public and have vast experience in delivering flu and COVID-19 vaccinations, among others.
It has already been highlighted that the current approach for MMRV is falling short of expectations. Ben Coleman, Labour MP for Chelsea and Fulham and member of the Commons Health and Social Care Select Committee, said during an oral evidence session on vaccination on 11 February 2026: “I keep coming back to the basic fact that [MMR vaccination programmes are] not working well enough.”
However, funding, contracting and regulatory aspects must be addressed, as radical reform is needed for progress to be made.
The contractual “element” was described by Mary Ramsay, director of public health programmes at the UKHSA, in the same session with the Health and Social Care Committee.
“One problem is that there are already contracts to give”, she explained, further admitting that opposition among GPs towards community pharmacies being paid to perform a similar role has complicated things.
“GPs might be annoyed if pharmacies can do it?” Coleman asked, to which Ramsay replied: “That is an element.”
Community pharmacy has been here before. In August 2025, a GP practice told groups of patients to avoid getting their vaccinations at pharmacies. At the time, The Pharmaceutical Journal described this as “actively discouraging the public to seek protection in any way they can”, subsequently putting public health and prevention “at serious risk”.
However, a leaked letter from the British Medical Association (BMA) to chief medical officer Chris Whitty on 19 February 2026 suggested GPs felt providing flu jabs was “no longer a financially viable option”. In response, Malcolm Harrison, chief executive of the CCA, warned that the programme still “urgently needs additional funding”.
Organisations such as The King’s Fund have called for national contracts for general practice and community pharmacy that are, at the very least, “coherent and complementary” to encourage collaboration, which can be further supplemented by the ‘single and multi-neighbourhood providers’ contracts promised under the NHS ten-year health plan. On 22 February 2026, it was announced that the new GP contract will provide financial incentives that recognise practices making progress on vaccination. Will a similar offer be made for pharmacy as part of current contract negotiations? Only time will tell.
It is essential that patients and public health are prioritised and the system fully redesigned
On regulation, in its response to a consultation on proposals to amend the Human Medicines Regulations 2012, published on 20 January 2026, the government announced that community pharmacies will be allowed to offer vaccination services outside registered premises. It will also allow NHS service providers to redistribute vaccine stock without the need for a wholesale dealer’s licence when clinically essential and if the vaccine is kept in its original packaging.
At the same time, the government announced plans to introduce a new legal mechanism of vaccine group directions, which will replace national protocols in allowing an expanded workforce to deliver vaccinations. These changes will certainly act as enablers for pharmacists to deliver more vital vaccination outreach services.
With further outbreaks inevitable, the time has now come to enact a different approach to public health that fully includes pharmacy. There is no time for complacency — it is essential that patients and public health are prioritised and the system fully redesigned to remove competition and provide incentives for closer ‘neighbourhood working’.
Mobilising community pharmacies to administer essential vaccines in response to outbreaks is a sensible approach that utilises their expertise to successfully supplement existing programmes, and one that can be built on to fully tackle misinformation. However, this responsibility must come with fair funding and an acknowledgement that community pharmacy’s involvement is central to turning the tide on vaccine hesitancy. PJ