Adisha Pramod / Alamy Stock Photo
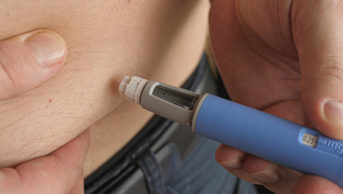
Semaglutide, in its latest incarnation — Wegovy (Novo Nordisk) — has been heralded in a tidal wave of articles and social media posts as the “game-changing” “skinny jab” that will help people lose weight when all else has failed.
Such is the media hype that, at this year’s Academy Awards in March 2023, host Jimmy Kimmel joked: “Everybody looks so great. When I look around this room, I can’t help but wonder ‘Is Ozempic right for me?’”
Ozempic is Novo Nordisk’s other semaglutide product, licensed for use in type 2 diabetes mellitus (T2DM), which is already being prescribed off-label for weight loss to such an extent that there are global shortages.
While supplies of Wegovy are yet to hit the UK, in March 2023, the National Institute for Health and Clinical Excellence (NICE) approved its use for people with obesity with at least one risk factor, through specialist NHS services[1].
With around a quarter of adults in the UK living with obesity, demand is expected to be high. Several community pharmacies have already indicated that they plan to offer the once-a-week treatment privately through their online dispensing doctor arms, with some setting up waiting lists for interested patients. However, there is little detail on how ongoing support for healthy lifestyle changes as well as mental health support will be provided, leading some experts to question whether the drug should be made available in this way.
Effective treatment
Weight loss drugs have a difficult history: either they worked very well but had dangerous side effects, or were safer but not that effective, says Duane Mellor, registered dietitian and senior lecturer at Aston University Medical School in Birmingham, UK.
When used in accordance with prescribed guidelines, it promotes weight loss in a safe and effective way for most people
Stephen Lawrence, associate clinical professor at Warwick Medical School
Semaglutide seems to be a welcome step forward. As Stephen Lawrence, associate clinical professor at Warwick Medical School in Coventry, UK, points out “when used in accordance with prescribed guidelines, it promotes weight loss in a safe and effective way for most people”, and the treatment has already been used in T2DM.
The medicine is from a class of drugs known as glucagon-like peptide-1 (GLP-1) agonists, which mimic the naturally occurring hormone GLP-1, stimulating the production of insulin. But this class of drugs also reduces appetite, hence their newfound fame.
The evidence for weight loss comes from the STEP 1 randomised double-blind trial, which compared a once weekly semaglutide injection with placebo[2]. During the study, both patient groups had counselling and support for adopting a reduced calorie diet (500 calories per day deficit) and doing more physical activity (150 minutes per week).
In the trial of 1,961 adults without TD2M, who had either a body mass index (BMI) of 30 or more, or a BMI of 27–29 and at least one comorbidity, those taking semaglutide achieved an average of 14.9% body weight loss at 68 weeks, compared with 2.4% in those who received placebo.
Semaglutide also shifted a larger proportion of people from non-diabetic hyperglycaemia to normoglycaemia — 79% of those taking semaglutide and 39% of those on placebo.
An indirect comparison of data by Novo Nordisk from the STEP 1 trial and the SCALE trial of daily GLP-1 agonist liraglutide suggested 5.81% more weight loss with semaglutide than liraglutide at 68 weeks, and this was backed up by data from the STEP 8 trial, which directly compared the two treatments[1,3,4].
The weight loss resulting from semaglutide is “far more than we’ve seen before”, says Mellor, and seems to be enough to reduce the risk of developing T2DM in addition to its action of helping to manage glucose levels.
Limited options
NICE points out that, until now, people with obesity have had limited treatment options and there is a large unmet need in this population.
“Overweight and obesity can be physically debilitating and may lead to severe and potentially life-limiting conditions, as well as fertility issues and symptoms such as skin infections,” the committee said in its guidance on semaglutide[1].
Liraglutide (Saxenda; Novo Nordisk) is limited to a specific population who have non-diabetic hyperglycaemia and a risk factor for cardiovascular disease, and obesity drug orlistat is poorly tolerated and therefore rarely used[5]. Even after bariatric surgery, maintaining weight loss is challenging.
NICE is not — and rightly so — recommending this as a lifestyle medication
Duane Mellor, registered dietitian and senior lecturer at Aston University Medical School
NICE wants semaglutide to be an option for those with the highest risk: people with at least one weight-related comorbidity and a BMI of 35 or more, or people with a BMI of 30–34 who meet the criteria for referral to specialist weight management services. It specifies that semaglutide should be used for a maximum of two years within multidisciplinary specialist weight management services, including “but not limited to” NHS tier 3 and 4 services.
Lower BMI thresholds (usually reduced by 2.5) should be used for people from South Asian, Chinese, other Asian, Middle Eastern, black African or African-Caribbean backgrounds.
Mellor adds: “NICE is not — and rightly so — recommending this as a lifestyle medication. Some of the media hype is unfortunate, because we need to focus on [semaglutide] to improve health.”
Patchy access
But NHS access may be difficult, with very few people with a BMI of 30–34 currently referred to tier 3 services, as well as long waiting lists and patchy availability around the country.
Experts say this is likely to be only the start of the use of this class of drugs in helping those with obesity lose weight. The next to come down the track is tirzepatide (Eli Lilly), which studies suggest has an even more impressive impact on weight loss[6]. The NHS may well struggle to manage this demand.
Making semaglutide available privately via community pharmacies will open access to more people than will be able to obtain it on the NHS, since private providers do not need to follow NICE guidance, only the licensed indication, which is as an adjunct to a reduced-calorie diet and increased physical activity for those with a BMI over 30, or a BMI over 27 with at least one weight-related comorbidity.
Multiples, including Boots, Lloydspharmacy and Superdrug, say they already have experience of providing safe and effective weight loss services, with several different treatment options, including Saxenda.
A spokesperson for LloydsPharmacy Online Doctor says it will be incorporating Wegovy into its GP-led weight loss service when it becomes available.
Patients will first have to complete a questionnaire, which includes information about their BMI, as well as submit photos of themselves on a scale
Spokesperson for Superdrug
“Once launched, LloydsPharmacy Online Doctor’s clinicians may prescribe Wegovy if medically appropriate. Patients taking Wegovy should also make healthy lifestyle changes, such as taking increased exercise and following a healthier diet. Ongoing patient supervision and support for making healthier lifestyle choices are part of the LloydsPharmacy Online Doctor service.”
Patients can currently choose between an in-store or online medicated weight loss service to access Saxenda from LloydsPharmacy, but they must have their BMI checked in store.
A spokesperson for Superdrug says: “Patients will first have to complete a questionnaire, which includes information about their BMI, as well as submit photos of themselves on a scale.
“Our doctors will then review and ensure the treatment is suitable for the patient before prescribing. The patient must collect the treatment from one of our Superdrug pharmacies, where our pharmacists will provide further advice and guidance, where needed.”
Boots also has an online doctor weight loss treatment service, which it says provides an option for people who are worried that their weight is impacting their health.
A spokesperson for Boots says: “Patients are required to complete an online consultation, which is reviewed by one of the Boots Online Doctor clinicians to determine if treatment is appropriate. Those who are prescribed treatment will receive follow up support from the team and can access advice and support from our pharmacy teams in stores.”
In addition to follow-up care from the Boots Online Doctor team, Boots offers a range of weight loss resources and webinars, including a free, ten-week weight loss programme, which can be accessed regardless of whether treatment has been prescribed.
Specialist service
“I don’t necessarily think that pharmacy is a bad place to offer this kind of stuff. It’s just a question of what that looks like,” says Mellor, who is among those who want to see more detail on how long-term appropriate support for patients would be offered through private providers.
NICE believes that provision of semaglutide should be part of a package of care provided in a specialist weight management service. The NICE guideline committee emphasised that NHS tier 3 and 4 services “are the only appropriate setting for semaglutide treatment given the marketing authorisation”[1].
These services provide care for long periods of time (up to two years), including comprehensive multidisciplinary team assessment and interventions, such as dietary, lifestyle and behaviour modification advice, with or without medicines, as well as psychological support.
Providing semaglutide alongside a short-term weight loss programme without the necessary psychological support, could end up doing more damage to people in the long run, says Hannah Beba, consultant pharmacist in diabetes at West Yorkshire Health and Care Partnership.
Beba says there may also be side effects that, in her experience, people do not always admit to, because they are so desperate to continue taking it.
We are walking a very fine line with this drug and we need to be very cautious with it as a profession
Hannah Beba, consultant pharmacist in diabetes at West Yorkshire Health and Care Partnership
NICE specifically notes that standard 12-week weight loss programmes do not offer enough support, especially given that semaglutide has an initial 16-week dose escalation period.
Beba says that if there are not clear checks for those trying to access the drug (and some may be more rigorous than others) with a consultation of at least one hour, it can easily move from being something people use to improve their health to becoming something people take for cosmetic reasons.
“We are walking a very fine line with this drug and we need to be very cautious with it as a profession. We could end up doing ourselves a lot of damage and we need to treat this drug with the respect that it deserves.”
Mellor adds that some private providers of the drug may struggle to support people in the longer term. “How can we prioritise this being a health thing rather than a money-making thing?”
Not a quick fix
NICE chose a two-year maximum window for a person to take semaglutide for weight loss for two reasons — first, because that fits with NHS tier 3 and 4 services and, second, because that was the model Novo Nordisk presented in line with current trial evidence.
The goal is to give people time to make the lifestyle changes to maintain weight loss. However, in reality, obesity is a lifelong condition. The position may change as more evidence is collected on the clinical benefits of longer-term use, says NICE.
You need more than 12 weeks of support to get back to having a healthy relationship with food
Duane Mellor, registered dietitian and senior lecturer at Aston University Medical School
But it is important to note that this medicine is “not a quick fix”, says Lawrence.
Weight loss is not a “temporary journey”, Mellor points out, although he says online weight management services can be very helpful for some people — when done well.
“You need more than 12 weeks of support to get back to having a healthy relationship with food.”
Evidence from the STEP 1 extension trial suggests that once people stop taking semaglutide, they will put the weight back on[7]. Novo Nordisk’s own model assumes that, three years after stopping a two-year course of semaglutide, the weight advantage over those who did not receive it would be lost[1].
Beba would like to see a cautious, staged introduction to the use of semaglutide, focusing on NHS specialist services and collecting real-world data, while acknowledging there will be issues with access.
“My concern is that we do it all at once, and we can’t learn from any of it because it’s just going to be chaos.” It is a whole different ball game from Saxenda and the demand is going to be huge, she adds.
For those paying for semaglutide, this could be a very long-term commitment, both financially and practically. The cost of Wegovy is not yet clear but the NHS list price of Ozempic is £73 for a pack of four syringes. Community pharmacies currently charge around £240 per month for Saxenda.
Health inequalities
A real concern is that those who could benefit most would never be able to afford a private prescription through an online pharmacy and may also struggle to access NHS services.
“We know health inequalities are a problem and they’re not getting any better,” says Mellor. And those from more deprived backgrounds may actually need more support in their family environment, taking into account their living and financial situation, which is challenging, he adds.
Beba shares his concerns. “This is almost definitely going to drive some inequalities,” she adds. She also questions whether the screening processes employed by community pharmacies will include questions about ethnicity, taking into account the lower threshold for treatment.
‘Black cloud’
The whole landscape is further complicated by the fact that Novo Nordisk recently received a two-year suspension from membership of the Association of the British Pharmaceutical Industry (ABPI), following serious breaches of its code.
The suspension came after an investigation into concerns about the pharmaceutical company’s sponsorship of a weight management course aimed at training healthcare professionals to set up a weight loss service, which offered delegates a one-year patient group direction for liraglutide.
The Disclosure UK database shows that Boots and LloydsPharmacy received event sponsorship from Novo Nordisk in 2021, although there is no suggestion of any wrongdoing.
A spokesperson from Boots says: “Like other pharmacies, we sometimes work with pharmaceutical manufacturers to provide education for our pharmacy team members, in line with ABPI Code of Practice.”
LloydsPharmacy failed to respond to a request for comment.
“The fact [Wegovy] has got quite a black cloud kind of hanging over it now, despite it being a good drug when used in the right way” is concerning, says Beba.
“We need a measured approach because we know the evidence for it is so good in the right populations. There is a reason why people are excited about it. It’s just getting that balance right.”
Beba would prefer community pharmacy to become part of NHS provision down the line.
“This will be a really great opportunity for community pharmacy to join with the rest of the healthcare system.”
- 1Semaglutide for managing overweight and obesity. National Institute for Health and Care Excellence. 2023.https://www.nice.org.uk/guidance/ta875/chapter/1-Recommendations (accessed 4 Apr 2023).
- 2Wilding JPH, Batterham RL, Calanna S, et al. Once-Weekly Semaglutide in Adults with Overweight or Obesity. N Engl J Med. 2021;384:989–1002. doi:10.1056/nejmoa2032183
- 3Pi-Sunyer X, Astrup A, Fujioka K, et al. A Randomized, Controlled Trial of 3.0 mg of Liraglutide in Weight Management. N Engl J Med. 2015;373:11–22. doi:10.1056/nejmoa1411892
- 4Rubino DM, Greenway FL, Khalid U, et al. Effect of Weekly Subcutaneous Semaglutide vs Daily Liraglutide on Body Weight in Adults With Overweight or Obesity Without Diabetes. JAMA. 2022;327:138. doi:10.1001/jama.2021.23619
- 5Liraglutide for managing overweight and obesity. National Institute for Health and Care Excellence . 2020.https://www.nice.org.uk/guidance/ta664 (accessed 4 Apr 2023).
- 6Jastreboff AM, Aronne LJ, Ahmad NN, et al. Tirzepatide Once Weekly for the Treatment of Obesity. N Engl J Med. 2022;387:205–16. doi:10.1056/nejmoa2206038
- 7Wilding JPH, Batterham RL, Davies M, et al. Weight regain and cardiometabolic effects after withdrawal of semaglutide: The <scp>STEP</scp> 1 trial extension. Diabetes Obesity Metabolism. 2022;24:1553–64. doi:10.1111/dom.14725