Sansea2 / Wikimedia Commons
Spironolactone, used to treat fluid retention in patients with oedema, heart failure and hypertension, can also alleviate side effects from corticosteroid-based creams used for certain skin conditions, according to research published in the Journal of Investigative Dermatology
[1]
.
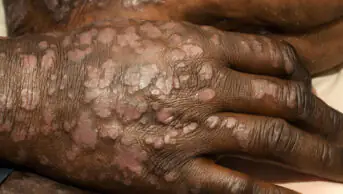
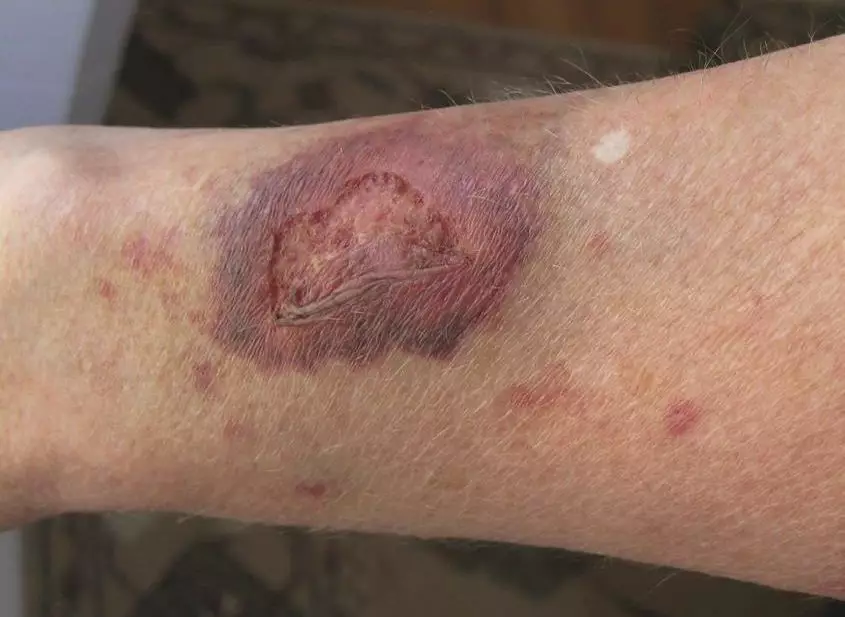
Corticosteroid creams, used to treat inflammatory skin diseases such as atopic dermatitis and psoriasis, can lead to adverse effects ranging from a slight burning sensation to a thinning of the skin.
The investigators, from the Institut National de la Santé et de la Recherche Médicale (INSERM) in Paris, hypothesised that the creams might be activating mineralocorticoid receptors (MRs) located in the epidermis. These receptors, which are also present in other parts of the body, such as the kidney, heart and eye, interact with aldosterone, a hormone that regulates blood pressure.
Nicolette Farman, director of research at INSERM, says the group started by considering whether adding specific antagonists to aldosterone would block the receptors and restore proliferation of the epidermal cells.
In a randomised double-blind controlled trial, the researchers applied gels containing the topical glucocorticoid (GC) clobetasol, the MR antagonist spironolactone, both compounds together or a placebo to the forearms of 23 healthy volunteers for 28 days.
Topical application of clobetasol resulted in noticeable skin thinning at day 29 compared with the placebo (P=0.0002), as the researchers had predicted. Spironolactone alone did not affect the thickness of the epidermis, but the combination of spironolactone and clobetasol significantly increased epidermal thickness (P=0.04), compared with clobetasol alone.
The researchers note that three volunteers had almost no change in epidermal thickness, while another three presented with thicker epidermis after the application of clobetasol, leading the researchers to classify them as GC-resistant. In an analysis of the 17 clobetasol responders, those in whom clobetasol induced epidermal atrophy, the combined effect of spironolactone and clobetasol was even more pronounced, the researchers found.
“This is potentially very exciting research,” says Emma Wedgeworth, a consultant dermatologist and spokesperson for the British Skin Foundation, who was not involved in the research. “The underlying mechanism of [skin] atrophy is poorly understood and the authors’ theory that this may be mediated through the mineralocorticoid receptor is interesting.”
Wedgeworth points out that the research is in its preliminary stage and that the volunteers were all in good health.
“While the mineralocorticoid antagonist may reduce the skin thinning effect of topical glucocorticoids, it may also reduce the anti-inflammatory effect thus making the topical steroid less clinically effective,” she says, adding that little is known about possible side effects of long term use of a topical mineralocorticoid.
Farman acknowledges that the trial’s use of healthy volunteers makes it “difficult to extrapolate results”. She says the group would need to test their findings in clinical situations to evaluate the efficacy of the combined compounds in conditions such as psoriasis and eczema, and that this process was likely to take an additional five to ten years.
“We need a better formulation for spironolactone,” she adds. “It’s highly impermeable, so very little spironolactone currently gets into the skin. But if it is absorbed too much, this can have effects on the kidneys.”
References
[1] Maubec E, Laouenan C, Deschamps L et al. Topical mineralocorticoid receptor blockage limits glucocorticoid-induced epidermal atrophy in human skin. Journal of Investigative Dermatology 2015. doi:10.1038/jid.2015.44.