Shutterstock.com
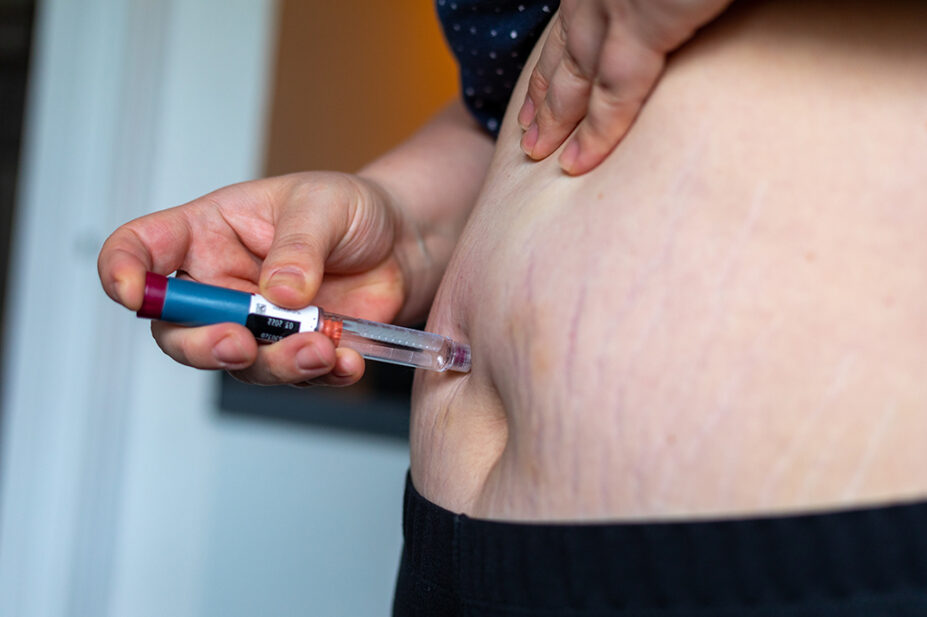
The UK government has announced that GPs will be able to prescribe weight loss injections as part of a £40m pilot to test if they can be initiated in non-hospital settings.
The pilot will look at GPs prescribing Wegovy (Novo Nordisk), a once-weekly injectable treatment of the glucagon-like peptide-1 receptor agonist semaglutide.
Wegovy has not been launched yet in the UK, but has already been recommended by the National Institute for Health and Care Excellence (NICE) for a maximum of two years in people with obesity with one weight-related comorbidity, such as type 2 diabetes mellitus (T2DM) or hypertension.
The NICE guidance states it can only be used as part of tier 3 or 4 NHS weight loss services, which offer comprehensive dietary, lifestyle and behaviour modification support.
However, the government said on 6 June 2023 that the GP-prescribing pilot will “explore how approved drugs can be made safely available to more people by expanding specialist weight management services outside of hospital settings”.
“This includes looking at how GPs could safely prescribe these drugs and how the NHS can provide support in the community or digitally — contributing to the government’s wider ambition to reduce pressure on hospitals and give people access to the care they need where it is most convenient for them,” it added.
Some community pharmacies have already said that they will offer private Wegovy services as soon as the drug becomes available in the UK, which is expected to be soon.
However, experts have warned that a community pharmacy setting may be inappropriate because patients require long-term multidisciplinary support, including counselling, to change their approach to food.
The cost of Wegovy in the UK has not yet been confirmed; however, the NHS list price of Ozempic — Novo Nordisk’s other semaglutide product licensed for use in T2DM — is £73 for a pack of four syringes.
The government also said that obesity — one of the leading causes of severe health conditions, including cardiovascular disease, diabetes and cancer, in the UK — costs the NHS £6.5bn per year.
Figures showed there were more than 1 million admissions to NHS hospitals in 2019/2020 where obesity was a factor.
In a statement, Steve Barclay, health and social care secretary, said: “This next generation of obesity drugs has the potential to help people lose significant amounts of weight, when prescribed with exercise, diet and behavioural support.
“Tackling obesity will help to reduce pressure on the NHS and cut waiting times, one of the government’s five priorities, and this pilot will help people live longer, healthier lives.”
The government added that NICE was also looking at the potential NHS use of the diabetes drug tirzepatide (Mounjaro; Lilly), which may also be able to help with weight loss if it is licensed for treating obesity in the coming months.
“NHS England is already working to ensure recommendations from NICE on offering this new class of treatment to patients, through established specialist weight management services, subject to negotiating a secure long-term supply of the products at prices that represent value for money taxpayers,” it said.
A statement from Sir Stephen Powis, medical director at the NHS, said: “Pharmaceutical treatments offer a new way of helping people with obesity gain a healthier weight and this new pilot will help determine if these medicines can be used safely and effectively in non-hospital settings, as well as a range of other interventions we have in place.”
1 comment
You must be logged in to post a comment.


Hi PJ team. The NICE guidance actually says "including, but not limited to tiers 3 and 4", so from the outset it was viewed as something potentially suitable for Primary Care initiation.