Shutterstock.com
Packs of topical corticosteroid will now include information about potential withdrawal reactions, following a review by the Medicines and Healthcare products Regulatory Agency (MHRA).
The MHRA’s comprehensive evidence review, which looked at the risk of topical steroid withdrawal reactions, was triggered by an enquiry from a patient representative to the Yellow Card scheme.
Having considered evidence from patients, healthcare professionals and the literature, as well as Yellow Cards reported between 1963 and 2020, the MHRA review concluded that there was a risk — albeit “very infrequent” — that long-term or incorrect use of topical corticosteroids, particularly those of “moderate to high-potency”, could lead to withdrawal symptoms.
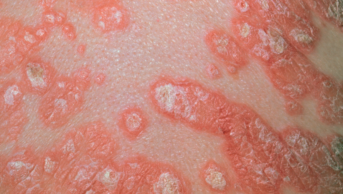
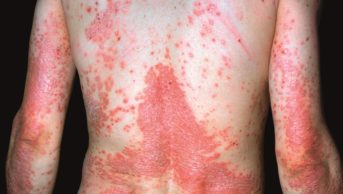
Topical corticosteroids are used to treat skin disorders, such as eczema, psoriasis and contact dermatitis. Some, such as hydrocortisone, are classed as pharmacy medicines while others, such as betamethasone, are only available on prescription.
The review says withdrawal symptoms include redness of the skin; a burning sensation; and itchiness, which may be followed by skin peeling distinct from the condition that caused the patient to use corticosteroids in the first place.
The MHRA has requested that marketing authorisation holders update the patient information leaflet (PIL) for both prescription-only and pharmacy medicines to include details of possible withdrawal reactions that may occur if the product is used continuously for long periods, usually over 12 months.
A patient safety leaflet, which provides guidance to patients and healthcare professionals, has been published to cover the interim period while PILs are updated.
An accompanying drug safety article advises prescribers to “consider the lowest potency needed”, and to be “vigilant for the signs and symptoms of topical steroid withdrawal reactions”.
Andrew Proctor, chief executive of the National Eczema Society, said that many children and adults rely on topical corticosteroids to manage eczema inflammation.
“[The National Eczema Society urges] people who are affected to read the newly published patient safety leaflet and to speak to their doctor or other prescriber if they have questions and concerns,” he added.
Jane Harvey, pharmacist and research assistant at the Centre of Evidence-Based Dermatology at the University of Nottingham, said it provided an “ideal opportunity” for pharmacists to be involved in reviewing repeat issues of potent topical corticosteroids to ensure that patients are not using these medications continually for such long periods without being referred to a specialist.
However, she expressed concerns that patients who see the warning may only read the first part of the text, regarding withdrawal reactions, “if you have a flare-up or your skin condition returns shortly after stopping treatment”, and may not go on to read that this is only the case if the patient has used the product continuously for over 12 months.
“Nearly everyone with moderate to severe eczema will flare at some stage after a burst of topical corticosteroids treatment; this is because of the disease activity, not a treatment effect,” she explained.
“Underuse of appropriate topical corticosteroids is already a major problem resulting in poor eczema control especially in children — so there is a danger that a message conveying that a flare on stopping could be due to topical corticosteroids withdrawal might worsen the situation and lead to lots of children suffering poor quality of life.
“Therefore it may be useful for pharmacists to be aware of this context, and pass this information on to patients”.
READ MORE: Managing childhood eczema: a visual guide
- This article was amended on 20 September 2021 to clarify that the guidance is around dangers of continual long-term use of topical corticosteroids, as opposed to start/stop long-term use