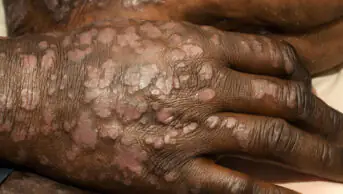
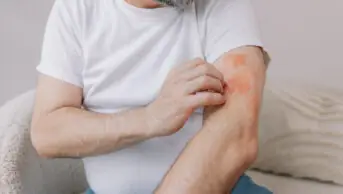
Courtesy of Julia Newton-Bishop
Patients with malignant melanoma should not be advised to stay out of the sun without taking measures to ensure healthy levels of vitamin D, according to Julia Newton-Bishop, professor of dermatology at the University of Leeds.
Speaking at the British Association of Dermatologists annual meeting held in Birmingham on 5-7 July 2016, Newton-Bishop said that health agencies often advocate sun avoidance for melanoma patients in order to prevent more tumours but vitamin D can be important in determining the aggressiveness of melanomas.
Melanoma patients tend to be fair-skinned people who cover up in the sun to minimise the risk of burning but as a result they also have lower levels of vitamin D, which are associated with thicker (worse) tumours and poorer survival. A lack of sun exposure after diagnosis could depress vitamin D levels further, explained Newton-Bishop.
When a melanoma is diagnosed, a patient’s vitamin D levels should be checked and supplements offered if levels are low, in accordance with guidance from the National Institute for Health and Care Excellence (NICE).
“Patients often ask, ‘Can I get enough sun to make the required vitamin D without getting burned?’ I think the safest approach is to wear sunblock and take supplements,” said Newton-Bishop, who recommends using doses of 400iu vitamin D3 per day, as per advice from the Scientific Advisory Committee on Nutrition (SACN). High doses of Vitamin D can in theory be immunosuppressive so it is probably better to rectify a deficiency slowly, she explained, starting with 800iu per day, reducing to 400iu per day when levels reach 60nmol/L.
Melanoma patients should still avoid intense sun exposure (when the UV index is at or above 3) and should ensure they do not get sunburnt.
The metabolic role of vitamin D has been extensively investigated in recent years. It has an antiproliferative action on cells, reduces oxidative stress, stimulates innate immunity, and inhibits angiogenesis. Emerging findings suggest that high grade tumours (melanomas) are associated with low vitamin D levels. “There is mounting evidence of causality,” said Newton-Bishop. Vitamin D may also be important for survival after diagnosis of melanoma, she added.
Vitamin D is made by the action of sunlight (UVB) on skin and the optimal serum level is thought to be around 60nmol/L (although some experts say 75nmol/L), explained Newton-Bishop. However, after an average weekend of sun exposure (six hours in the sun), most people still fail to reach the 60nmol/L level, according to a study conducted in Yorkshire. “It appears that you need rather a lot of sun exposure in Yorkshire to have enough vitamin D,” concluded Newton-Bishop.
Further information about melanomas and vitamin D for healthcare professionals and patients is available on the Genomel (Melanoma Genetics Consortium) website: www.genomel.org.