Shutterstock.com
Open access article
The Royal Pharmaceutical Society has made this article free to access in order to help healthcare professionals stay informed about an issue of national importance.
To learn more about coronavirus, please visit:https://www.rpharms.com/resources/pharmacy-guides/wuhan-novel-coronavirus

Source: Shutterstock.com
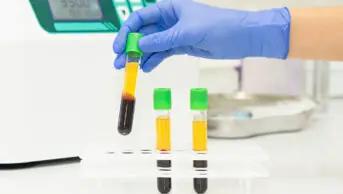
We wrote back in April 2020 that the general public may have to wait a while before they were able to buy a kit off the shelf to see if they had been infected with SARS-CoV-2, which causes COVID-19. This was prescient.
Since then, there have been several laboratory-based tests evaluated for use in the NHS by Public Health England. But these tests are only given to NHS and care staff, as well as some hospital patients and care home residents.
As of 22 July 2020, 1.3 million antibody tests have been carried out; however, these are no ‘get out of jail free’ cards. Even if you have a confirmed antibody test, the advice on social distancing remains exactly the same as if you had a negative one.
Although the tests may provide some peace of mind to those who have a confirmed result, there is very little evidence yet about whether these tests show any level of immunity to reinfection. Until we know what antibody profile relates to protective immunity, the detection of antibodies means little: a person may have confirmed antibodies and be susceptible to illness or be infectious.
In fact, one recent study has suggested that for those with a milder SARS-CoV-2 infection, the response of antibodies may disappear within 60 days.
And concerns have been raised about their level of accuracy. The government’s Scientific Advisory Group for Emergencies expressed concern in April that regulators were using a specificity — the ability to correctly identify samples without antibodies — threshold of 98%. This would mean that if 5% of a population had COVID-19, 28% with a confirmed result for antibodies may not have ever been infected.
This brings the risk that these tests give false confidence to those who have a confirmed result, meaning they take greater risks with their health and spread infection unwittingly.
We are still waiting for a point-of-care antibody test to be developed. Matt Hancock, the health and social care secretary, said the government was looking at “immunity passports” in March 2020, and hopes were raised further in May, when its COVID-19 testing strategy said that once laboratory antibody tests were approved, eventually testing could potentially be done at home with a finger prick, delivering results “maybe in as little as 20 minutes”.
There appears to have been some progress recently. In July 2020, it was revealed that a government-backed test developed by the UK Rapid Test Consortium, a partnership between the University of Oxford and UK diagnostics firms, is being considered by regulators for home use.
Reports appeared in the media in July 2020 describing the AbC-19 lateral flow test as “truly amazing”. However, there are no published results of clinical trials in the public domain yet and it is wise to be sceptical of claims made by manufacturers. A consignment of millions of tests procured by the government and described as a “game changer” in March 2020 by prime minister Boris Johnson were later found to be completely useless.
And — despite being a “target setting” for antibody testing — the role of community pharmacy has yet to be defined. In May 2020, Superdrug was the first pharmacy to offer a CE-marked COVID-19 antibody test, manufactured by Abbott, to the public for £69 through its online store. However, a day after the test was listed for sale, Abbott said in a statement that the test was “not intended for home use” and the Medicines and Healthcare products Regulatory Agency asked for the sale of the tests to be halted “until the regulatory and safety concerns have been resolved”.
On 15 July 2020, The Pharmaceutical Journal revealed that 470 community pharmacies were offering a finger-prick point-of-care antibody test supplied by Pharmadoctor. However, the General Pharmaceutical Council later wrote to all pharmacies saying they should not supply such tests.
What once looked like a “game-changer” is proving a much harder nut to crack than perhaps ministers first appreciated.
Read more: Everything you need to know about COVID-19 antibody tests