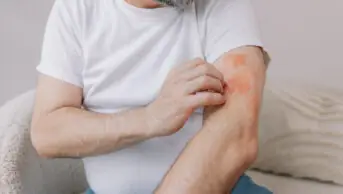
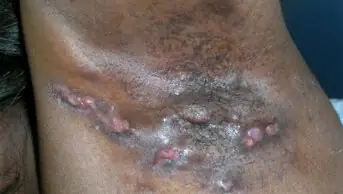
Emollients are prescribed extensively for skin conditions such as atopic eczema, contact dermatitis and psoriasis. These conditions account for a large proportion of dermatological consultations and their prevalence is increasing.1 Although dry skin conditions are not fatal, eczema that affects the hands is far from trivial and is a major cause of lost productivity.2
Emollients are the obvious treatment for dry skin and a wide range of branded and generic products is available. Unfortunately, many health care professionals and patients overlook the importance of emollients and these products are not popularly perceived as being “active treatments”. Recent findings, together with advances in the understanding of skin structure and function, suggest that emollients may be very effective, if used appropriately.
Emollients may appear to be ineffective because they are often used in small quantities. This may be because of the belief that they are not “active”, because they are uncomfortable or unpleasant to use, or because small amounts are prescribed, thereby reinforcing the view that they should be used in small amounts. Incorrect use may also reflect a lack of information or understanding about the place of emollients in an overall treatment package.
The epidermal barrier
The epidermis is composed of layers of densely-packed keratinocytes (see Figure 1). These are formed in the stratum basale (germinative layer) and gradually migrate upwards to the surface layer — the stratum corneum (horny layer). The stratum corneum contains corneocytes — flattened, dead cells that have lost their nuclei — which are gradually shed. In between the stratum basale and the stratum corneum there is considerable activity, as keratinocytes differentiate and mature into corneocytes. The secretion of extracellular lipids plays an important part in this process. In the stratum granulosum (granular layer), a lipid substance is formed and stored in the lamellar bodies. At the interface between the stratum granulosum and the stratum corneum, lipids are extruded from the cells into the inter-corneocyte space. These “barrier lipids” then form highly organised, multilamellar bilayers.
Although cells are continuously shed from the upper surface of the stratum corneum, the deeper layers are firmly bonded together. The integrity of this layer is important as it prevents water loss from the skin. It is held together by the lamellar lipids. The corneocytes themselves contain a water-retaining substance called natural moisturising factor, which ensures that water is held in the cells. Cells with a high water content swell and press tightly against one another, with no cracks or fissures. The healthy stratum corneum has a relatively high water content and is elastic and pliable.
Abnormal barrier function
Dry skin is the result of abnormal water loss. In normal, healthy skin, the epidermal barrier prevents excessive water loss. It is believed that defective epidermal barrier function, resulting from genetic changes, plays a central role in atopic eczema, contact dermatitis, psoriasis and ichthyoses.
In atopic eczema, there is a defect in the lipid extrusion process and, as a result, barrier lipids in the lower part of the stratum corneum are not formed normally.3 The absence of effective cellular “cement” results in impaired barrier function and increased water loss from the stratum corneum. As water is lost, the cells of the stratum corneum shrink and cracks open up between them. The result is dry skin, which can neither retain water effectively nor prevent the ingress of irritants or allergens. These changes can be seen in normal skin when some of the epidermal lipids are removed by repeated use of surfactants or solvents. The use of soap on eczematous skin removes more lipid and reduces barrier function further, eventually resulting in the appearance of lesions. Individuals with eczema are more sensitive to the effects of soap and surfactants than is usual, and even their apparently normal skin has a lower threshold for irritation than that of non-sufferers.
Healing the epidermal barrier
Emollients are believed to restore the integrity of the epidermal barrier in two ways. First, they form an oily layer over the skin that prevents the evaporation of water. Consequently, the water trapped in the stratum corneum passes into the corneocytes, which swell, and fissures reduce. Secondly, emollients may penetrate deep into the stratum corneum and mimic the barrier effects of the deficient lipids. This, in turn, prevents penetration of irritants and allergens. Allergens are recognised triggers for eczema in atopic individuals4 and provoke local inflammatory reactions resulting in the characteristic red, swollen and extremely itchy lesions of eczema.
Recently, there has been speculation that emollients might have indirect anti-inflammatory actions. This has arisen from the observation that, when the epidermal barrier is disrupted experimentally, the pro-inflammatory cytokine interleukin-1alpha (IL-1a) is released.3 It is thought that IL-1a is released in response to trauma, to promote repair of the epidermis but that excessive or inappropriate release might be involved in the pathogenesis of eczema. In skin diseases in which the epidermal barrier is impaired, it is possible that even minor trauma, such as that caused by scratching, may release IL-1a.
The release of IL-1a can be prevented by occlusion of the skin with polythene, which increases water retention in the skin. Emollients also increase water retention in skin and their apparent anti-pruritic and anti-inflammatory effects might be the result of reduced production and release of IL-1a, although this has yet to be demonstrated experimentally.
Practical considerations when using emollients
- Use of a combination of the three main types of emollient (lotions, creams and ointments) gives the best hydration and restores the skin’s barrier function. A lighter cream might be preferred during the day and a heavier ointment at night. Lotions are particularly good for weeping or &”wet” eczema
- Continuing to use the emollient, even when the eczema has improved, can help prevent flare-ups
- Shampoo can exacerbate eczema. Washing hair over the sink or bath to avoid exposing affected areas of the body to shampoo can help, as can wearing rubber gloves with a cotton lining to protect the hands. Shampoos are available from health food stores that do not contain sodium lauryl sulfate
- Sweating can aggravate eczema, so wearing light cotton clothing can help. Gently wiping sweat from the skin with a cotton cloth while exercising, having a cool shower afterwards and applying plenty of emollients can reduce irritation from sweat
- Carrying some emollient in a small container, such as a camera film container, encourages its use. (Wash, rinse and dry the container thoroughly before filling it.)
- Laundry — high temperature washes are needed to remove grease from clothing and bedding but biological powders and fabric softeners should be avoided. The washing machine should be run empty at high temperature, with washing powder, to clear any greasy residue
- Skin irrritation can be avoided by wiping excess emollient from the bath after bathing. The bath should then be cleanedwith a standard cleaner and rinsed thoroughly
Emollient products
Emollient products include creams, ointments, lotions, bath oils and soap substitutes. Finding the most suitable emollient for an individual may be a matter of trial and error. In general, greasier, oil-based products are more efficacious but they are less acceptable to patients. There is often a trade-off between efficacy and cosmetic acceptability (smell, consistency, etc). A patient may require different emollients for different areas of the body, for example, a heavy emollient for dry skin on the limbs and a lighter product for the face.
Some dermatologists encourage patients to try out a number of emollients (much as women test moisturisers at cosmetic counters) and choose the one they like best. This consumer-friendly approach has much to commend it.
There is a lack of good quality clinical trial evidence concerning the use of emollients5 and there is wide interpatient variation in response to their use. It is essential to find the cheapest emollient that is cosmetically acceptable to each patient to ensure that it is used on a regular basis. An emollient that is unacceptable will not be used.
Some emollients contain potential allergens that can exacerbate eczema. Creams and lotions, being oil-in-water emulsions, usually contain preservatives, such as benzyl alcohol and hydroxybenzoates (parabens) to prevent bacterial growth. Some products, notably aqueous cream, contain the surfactant sodium lauryl sulfate — a common cause of reactions, particularly in people with eczema.
The efficacy of emollients may be increased by the addition of a humectant, such as urea, and there are several such products available. However, the humectant itself can, occasionally, be irritant. Applying a simple emollient first can sometimes reduce this. Creams and ointments containing local anaesthetics are not suitable for the treatment of eczema because they may cause sensitisation. In addition, products containing antibiotics are also not suitable for routine use, although they may be required occasionally if eczema becomes infected.
Effective emollient use
As with so many treatments, clinical effectiveness depends not only on the correct choice of agent but also on its correct use. The British National Formulary notes that the effects of emollients “are short-lived and they should be applied frequently, even after improvement occurs”.6 It follows, therefore, that the choice of emollient and treatment regimen should be discussed with the patient, to explain the objective of the treatment and to find a workable treatment plan.
Complete emollient therapy7
Product: Emollient cream/ointment
Average prescription for two weeks: 1,000g
Correct use: Use liberally (500g per week is not unusual). Apply with clean hands after a bath to which bath oil has been added. Leave at least half an hour between emollient application and any topical steroid application to avoid dilution of the steroid or its spread to unaffected areas. Warm the emollient (eg, by standing it in the airing cupboard beforehand) so that itcan be applied more easily. If itching is a major problem, cool the emollient by storing it in the fridge). Apply extra product as frequently as possible in extreme weather (ideally three to four times a day, but at least twice a day). Apply gently in the direction of hair growth to prevent folliculitis.
Product: Emollient bath oil
Average prescription for two weeks: 210ml (ie, 500ml per month)
Correct use: The bath should be warm but no too hot, as this exacerbates itching. Use a bath mat to prevent slipping. Use 15ml of oil for an adult bath and 5ml for a baby bath. Pat skin dry, do not rub, as this may also exacerbate itching.
Product: Emollient soap substitute
Average prescription for two weeks: 150ml
Correct use: Use emollient soap substitute whenever washing hands and before getting into a bath or shower. Apply to dry skin then rinse off with water. Never use ordinary soap, “moisturising” soap or bubble bath.
Complete emollient therapy
Many dermatologists recommend “complete emollient therapy” in order to get the best effects from emollients. This therapy is based on the premise that the patient’s skin should be protected from soap and detergents as far as possible and treated with emollients as frequently as possible. It involves the use of an emollient cream or ointment, bath oil and soap substitute, backed up with education on how to use them (see panel above). Soaps and detergents, including so-called “moisturising soaps” and bubble baths, must be avoided at all times.
Topical steroid-sparing effects
By using emollients correctly, the quantity of topical steroid preparation used can be reduced. The topical steroid-sparing effects of emollient therapy have been reported in several trials.
In one double-blind study,8 four different treatment regimens were compared — daily topical steroid alone or topical steroid on two days out of either three, four or five days. The last three groups used emollient only on the non-steroid days. The four treatment regimens produced the same improvement in clinical signs of eczema over 21 days. However, there was a 75 per cent reduction in the amount of topical steroid used in the last group (topical steroids on two days out of five), compared with the daily topical steroid group. This may be a useful point to make to patients, as many are concerned about the long-term effects of using topical steroids. One survey of 200 dermatology outpatient clinics found that patients were concerned about the potential for side effects but were often unsure about the potency of the different products.9 About a quarter admitted to not using prescribed topical steroids because they were worried about side-effects.
Compliance
It is worth asking patients to demonstrate how they use their emollients, if they do not appear to be getting any benefit from them. Patients frequently do not use sufficient quantities of emollient and rarely receive any advice or explanation about how to use them.
An audit of the effects of explaining and demonstrating topical therapy for atopic eczema by specialist nurses showed that topical steroid use declined markedly during the study and the six sign atopic dermatitis severity score declined from 33 to 4.10 The study involved new patients, all of whom were children with eczema, who had not previously consulted a dermatologist. At baseline, none of the parents recalled having been shown how to use the products. The mean weekly emollient usage at the beginning of the 12-week study was 85g, while that at the end was 590g.
Conclusion
A survey of members of the National Eczema Society, carried out in 1993, showed that 40 per cent of adult patients and 65 per cent of parents of children with eczema wanted advice on how to use prescribed treatments.11 Many patients with skin complaints prefer to consult a community pharmacist rather than their general practitioner. Community pharmacists could make a major contribution in this area by actively encouraging effective emollient use.