Shutterstock.com
After reading this learning article you should be able to:
- Understand why skin of colour may be more prone to certain dermatological conditions;
- Identify dermatological conditions that are more common in skin of colour;
- Understand the treatment options available for these conditions.
Skin colour is mainly dependent on the presence of melanin, the pigment that protects the skin from ultraviolet (UV) radiation from the sun[1]. There are two types of melanin: eumelanin, a brown-black pigment; and pheomelanin, a yellow-red pigment[1]. Darker skin possesses more eumelanin than pheomelanin, whereas the reverse is true for lighter skin[1].
Melanin is produced by specialised skin cells called melanocytes and packaged into melanosomes[2]. The number of melanocytes does not vary between individuals of different races; however, the amount of melanin produced by the melanocytes is larger in darker skin[2]. As melanin provides protection from UV radiation, darker skin has greater protection against skin cancer and ageing, although it is not immune[2].
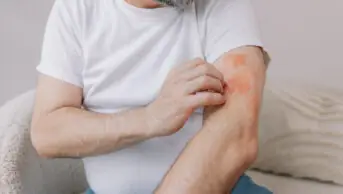
The terms ‘skin of colour’ and ‘people of colour’ can be used to describe individuals with skin tones darker than Caucasians, such as those of African, Asian, Middle Eastern or Hispanic/Latino descent[2]. People of colour may experience distinctive dermatological disorders, such as melasma, post-inflammatory hyperpigmentation, keloids, pseudofolliculitis barbae, central centrifugal cicatricial alopecia, and/or specific reaction patterns to skin disorders (e.g. follicular and discoid eczema)[2–4]. This may be partly owing to biological and structural differences observed in skin of colour, such as increased melanocyte activity and melanin content, increased fibroblast density and the curly nature of afro-textured hair[2]. Moreover, people of colour may partake in diverse cultural habits and practices that may impact the skin and hair (e.g. hair grooming practices, skin lightening, hair coverings, traditional Chinese medicine, homeopathy and ayurvedic medicine)[2].
This article outlines the presentation and management options for dermatological conditions more commonly observed in skin of colour to help pharmacists in deciding when to refer for medical review, and when to offer advice or over-the-counter (OTC) treatment. It is important that pharmacists can recognise these conditions in skin of colour so that their services and expertise can be tailored appropriately to serve a diverse population.
Melasma
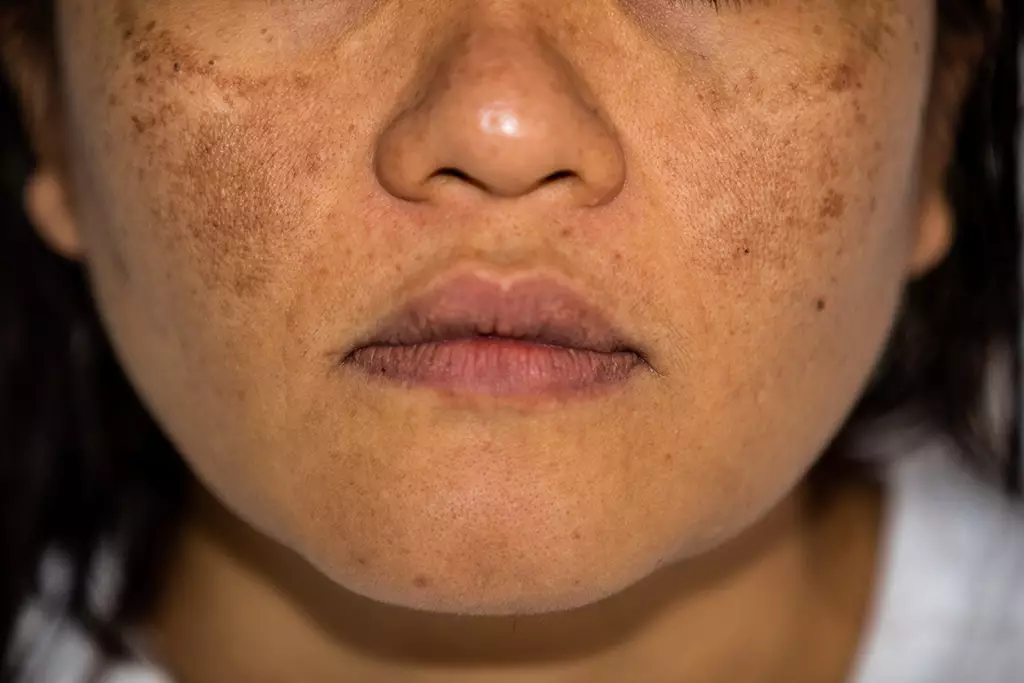
A chronic recurring pigmentary disorder, melasma occurs symmetrically on sun exposed areas of the body, particularly on the face (see Figure 1)[1]. The condition occurs most often in females of childbearing age with darker skin[1]. It can be classified as: centrofacial, where pigmentation occurs on the forehead, nose, and upper lip; malar, where pigmentation occurs on the cheeks; or mandibular, where pigmentation occurs on the jawline and chin[1]. Extra-facial sites are less common[5]. UV radiation, genetics (as evidenced by family history) and female sex hormones all play a role in the development of melasma, as a result of the over-production of melanin, which is deposited in the epidermis, dermis or both[1,6]. Oestrogen, associated with pregnancy, oral contraceptive pills or hormone replacement therapy, induces the release of melanocyte-stimulating hormone[7].
Diagnosis
Epidermal melasma appears as brown, macular (flat), patchy and well-defined discolouration with irregular borders, and usually responds to topical treatment[7]. Dermal melasma lies deeper in the skin, appears lighter brown to grey and is less well-defined[7]. Patients often have a combination of discolouration[1]. Differential diagnoses include pigmented contact dermatitis, minocycline-induced pigmentation, post-inflammatory hyperpigmentation and solar lentigines[7]. Melasma can be differentiated from other causes of discolouration by obtaining a good clinical history (e.g. relating to hormones, sun exposure etc.), supported by clinical examination findings.
Shutterstock.com
Management
There is no cure for melasma; in most cases, a multimodality approach is required. It usually takes three to six months before improvement is observed in response to treatment and there is a high risk of recurrence thereafter[8]. Patient counselling on the long-term prognosis of the condition, adherence to treatment and the need for maintenance therapy is essential[8].
General measures include stringent use of a broad-spectrum UVA and UVB protective sunscreen with a sun protective factor (SPF) of at least 30 — particularly those containing titanium oxide, zinc oxide or iron oxide to provide additional protection from visible light, which can be pigment-inducing in skin of colour[8]. Stopping any hormonal therapies (e.g. the contraceptive pill) may also be considered if thought to be implicated[9].
Treatment includes use of skin lightening agents, such as topical retinoids, hydroquinone, kojic acid, azelaic acid, arbutin, ascorbic acid and cysteamine[10]. Hydroquinone, a tyrosinase inhibitor, is the ‘gold standard’ treatment for hyperpigmentation[1,10]. It is used in varied concentrations, either as monotherapy or in combination with a retinoid and a fluorinated corticosteroid[1,9]. Such treatment should only be prescribed (once to twice daily for up to six months) by a dermatologist or doctor that is familiar with its use[4]. For moderate to severe melasma, a triple combination preparation (hydroquinone 5% w/w, hydrocortisone 1% w/w and tretinoin 0.1% w/w in a non-aqueous gel 0.3% w/v) can be prescribed in the UK as a private prescription or on the NHS as a ‘special’ recommended by the British Association of Dermatologists[11]. Second-line treatments of melasma include superficial chemical peels, laser treatment and oral tranexamic acid[10].
Many of the above options are not available on the NHS and patients may often find themselves forced to seek private treatment. It is important to be aware that patients may also purchase illegal hydroquinone, mercury or potent steroid-containing skin lightening products from the internet or beauty supply shops, which may lead to mercury poisoning or cutaneous side effects, such as exogenous ochronosis (paradoxical blue-black deposits in the skin owing to prolonged hydroquinone use), skin irritation and skin thinning[12,13]. Azelaic acid, topical retinoids and hydroquinone 5% w/w, hydrocortisone 1% w/w and tretinoin 0.1% w/w in a non-aqueous gel 0.3% w/v (in selected trusts) are the only skin lightening treatments available for prescription on the NHS[14]. Patients can be referred to their GP or a dermatologist who can prescribe these treatments.
Box: Counselling on skin lightening products
Skin lightening among people of colour is a sensitive and complex subject[13]. Although skin lightening agents are prescribed, when indicated, by dermatologists, some patients may purchase and misuse illegally sold agents, such as hydroquinone, corticosteroids and even mercury-containing products[13]. This should be advised against owing to the aforementioned potential side effects. Cultural factors may be strongly implicated; therefore, cultural sensitivity should be exercised should pharmacists wish to approach patients about skin lightening products. Patients seeking treatment for cutaneous side effects of skin lightening should be referred to a dermatologist.
When skin lightening products, such as hydroquinone, retinoids or azelaic acid are prescribed, it may be useful to recommend the following to mitigate potential skin irritation:
- Start at lower concentrations and titrate up, as tolerated;
- Combine hydroquinone with a topical steroid;
- Avoid prolonged use (more than six months) of hydroquinone;
- Use creams instead of gels, as they are thought to be less irritating;
- Apply two to three times per week initially and build up slowly (over four to six weeks) to daily use, as tolerated;
- Apply with a light moisturiser as a ‘buffer’;
- Apply a pea-sized amount initially, building up to a fingertip amount when tolerated;
- Use as ‘monotherapy’ initially or until tolerated, before considering combining other potentially irritating over-the-counter actives, such salicylic acid, glycolic acid, retinoids or ascorbic acid;
- Maintain a good skincare regimen with gentle cleansing and moisturising[15,16].
Post-inflammatory hyperpigmentation
Temporary hyperpigmentation that occurs during or after a period of injury to the skin is referred to as post-inflammatory hyperpigmentation (PIH)[7]. This injury could be the result of trauma, infection, allergic or irritant reactions, phototoxic eruptions and inflammatory conditions, such as acne, eczema or psoriasis[7]. The inflammation leads to activation of melanocytes, causing increased production of melanin, which is then taken up by surrounding cells in the epidermis and dermis[7].
Diagnosis
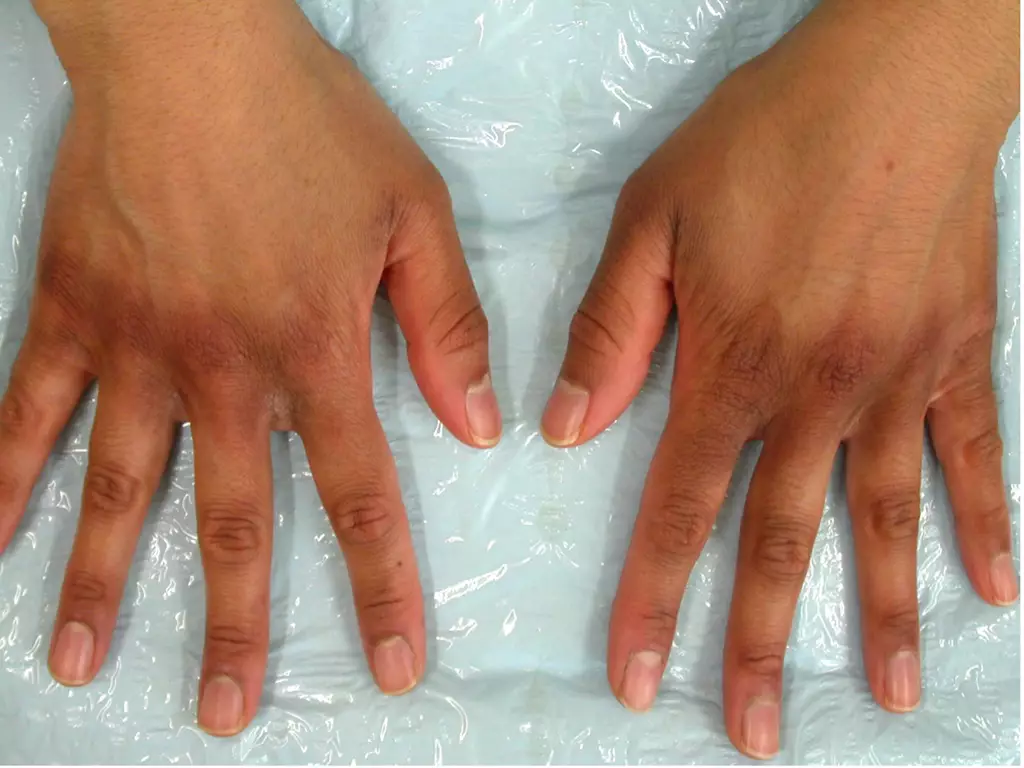
PIH is more likely to occur and persist for longer in people of colour. It usually presents as dark brown patches; however, grey or blue-grey discolouration can also occur and may take longer to fade (see Figure 2)[16]. Patients often describe a history of preceding inflammation, itching, redness or infection to the affected sites. This helps to differentiate PIH from many primary pigmentary disorders, such as melasma or lichen planus pigmentosus[7]. A skin biopsy is seldom needed but may be required in cases of diagnostic uncertainty[17].
DermNet New Zealand
Management
The most important measure against PIH is to treat the underlying inflammatory condition and consider stopping any medication that may induce pigmentation (e.g. minocycline, a tetracycline antibiotic)[16,18]. Topical treatments include retinoids, such as tretinoin or adapalene, azelaic acid, cysteamine and hydroquinone[7]. Adjunctive treatments, which are not available on the NHS, include superficial chemical peels (e.g. glycolic acid and salicylic acid), other topical treatments (e.g. ascorbic acid and kojic acid) and laser therapy[7]. Laser therapy should be used with caution in skin of colour by a practitioner who is familiar with treating darker skin types, owing to risks of scarring and hyperpigmentation[10].
As sun exposure can lead to the progression and persistence of PIH, it is also essential to apply a broad-spectrum UVA, UVB and visible light protective sunscreen with an SPF of at least 30. Photoprotective clothing and accessories should also be advised[7,19].
Generally, PIH is temporary and will gradually fade on its own. However, PIH can impact self-esteem and quality of life; therefore, patients may want to speed up the process of resolution[17]. Referral to a specialist is indicated for medical treatment or the treatment of the underlying inflammatory condition if this persists.
Traction alopecia
Hair loss that results from excessive pulling of the hair is referred to as traction alopecia (TA)[1]. It is induced by tight hair styles or hair coverings, and can affect people of different ages, genders and ethnicities[2]. It is commonly observed in women of colour with Afro-textured hair, owing to cultural hair styling practices[1].
Diagnosis
The clinical features of TA are seen in areas that have been placed under the most tension, commonly the fronto-temporal scalp (see Figure 3)[20]. In these areas, papules, pustules, pain and erythema may be observed acutely[19,20]. Tenting and dimpling of the scalp may also be noted[21]. As TA progresses, miniaturisation of the hair follicles occurs; this is illustrated by thinner and shortened hairs[5].
It is important that the correct diagnosis of TA is made through careful history-taking and examination, as differential diagnoses include conditions such as trichotillomania and frontal fibrosing alopecia[20]. If identified early, TA is typically reversible; however, if there has been sufficient progression, the hair loss becomes irreversible[20].
As with all hair loss patients, it is important that a correct diagnosis is sought before treatment or advice is given. Patients should therefore be advised to see a GP or dermatologist — preferably an individual who regularly treats hair loss.
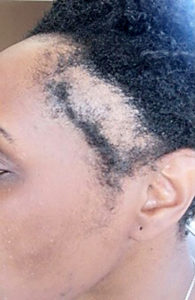
Sharon Belmo
Management
Addressing the causative practices and encouraging patients to adopt methods that will avoid placing the hair under further tension is central to the management of TA[20]. People with early-stage TA may benefit from camouflage techniques, such as hair fibres, paints/powders and scalp micropigmentation (a cosmetic non-surgical procedure whereby natural pigment is applied to the scalp), which help to provide an illusion of increased volume and hair density[1].
The literature on the medical management of TA is lacking; however, use of corticosteroids (topical and intralesional) and antibiotics (topical and oral), and minoxidil have been mentioned for their anti-inflammatory properties and stimulation of hair growth, respectively[20,22]. For some patients, hair transplantation may be a suitable option, particularly if the source of traction has been removed and there is no ongoing inflammation[23]. This option, as well as other suitability factors, can be assessed by a dermatologist or hair transplant surgeon.
Finally, the role of education in prevention and management should not be forgotten, and all healthcare professionals are well placed to advise against high tension, painful, traction-associated hairstyles, such as tight ponytails, buns, braids, wigs and weaves[1]. Patients can be signposted to resources, such as those produced by the British Association of Dermatologists.
Central centrifugal cicatricial alopecia
A common cause of hair loss that is found almost exclusively in women of African descent is central centrifugal cicatricial alopecia (CCCA)[1]. It is a scarring alopecia, which means that the hair loss is irreversible[24]. Such hair loss can be devastating to women of colour and cause substantial psychological distress. The cause of CCCA remains unclear. However, a combination of genetic factors and hair care practices are thought to be implicated[1].
Diagnosis
CCCA often presents with a circular patch of hair loss on the vertex of the scalp which expands peripherally, usually sparing the lateral and posterior scalp (see Figure 4)[1]. It may be associated with broken hairs and itching, soreness and burning owing to inflammation[1]. Advanced disease shows a smooth and shiny scalp indicating total and irreversible loss of hair follicles[24]. Patients often present at a late stage for several reasons, including late referral to dermatology and unawareness of hair loss owing to site and lack of symptoms[25]. Differential diagnoses include female pattern hair loss and lichen planopilaris[26]. Although both of these conditions can present with hair loss predominantly affecting the crown area, female pattern hair loss is generally asymptomatic and non-scarring, while lichen planopilaris may display clinical features, such as perifollicular scaling, redness or hyperpigmentation, in addition to scarring[27]. In cases of diagnostic uncertainty, biopsies may be performed, which can aid diagnosis by providing histological features that are characteristic of the disease[24].
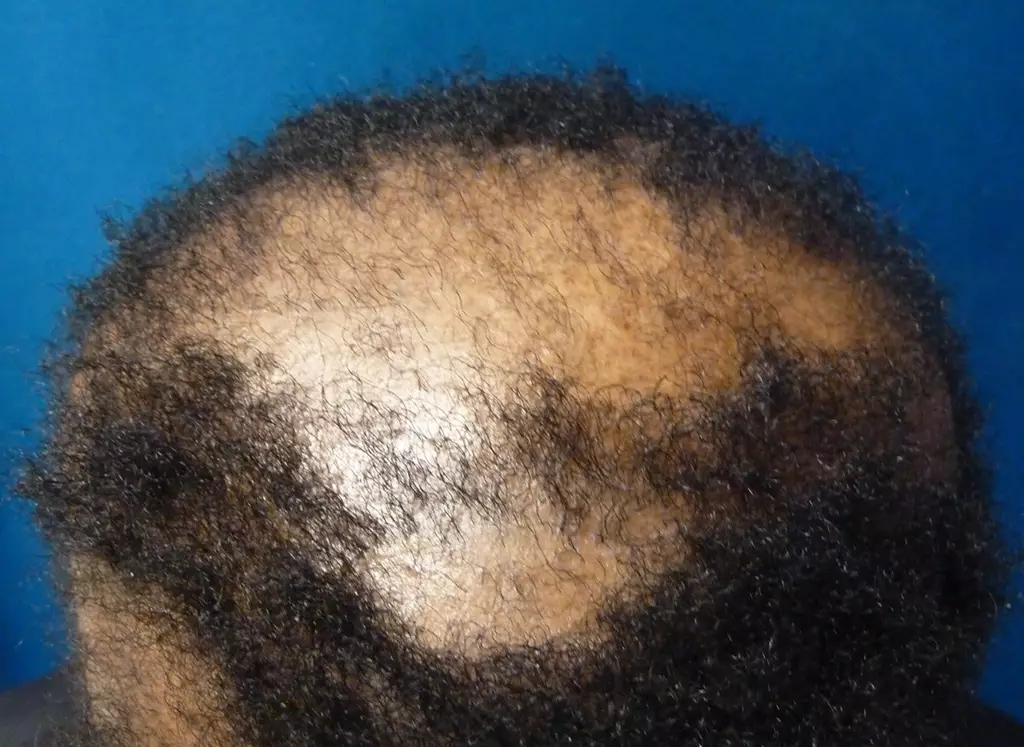
DermNet New Zealand
Management
Early diagnosis and treatment of CCCA is essential to try and limit scarring and salvage hair follicles before they are completely lost[26]. In advanced disease, the potential for any hair regrowth is minimal; therefore, the aim of treatment is to reduce symptoms and prevent further progression[25]. Topical or intralesional steroids are usually the first line of treatment[26,27]. Oral tetracyclines or hydroxychloroquine may also be used to try and halt inflammation[26]. Alternative or adjunctive therapies include topical calcineurin inhibitors, such as tacrolimus and pimecrolimus, topical minoxidil, cyclosporin and mycophenolate mofetil[24]. There are no licensed therapies for CCCA. The aforementioned treatments are used by dermatologists, particularly those with specialist interests in skin of colour or hair/afro-textured hair.
As hair care practices are thought to be implicated, as with TA, women should be encouraged to embrace their natural afro-textured hair, refrain from wearing tight hair styles and reduce or stop chemical relaxing and heat[26]. Permanent hair loss can be distressing, particularly in women. Patients should therefore be offered psychological support and signposted to support groups, such as the UK CCCA group[24,28].
Tinea capitis
Scalp ringworm, or tinea capitis, is a dermatophyte (fungal) infection of the hair on the scalp[29]. It is most common in pre-adolescent children, particularly those of African descent[30]. The most common pathogen causing the condition in the UK is Trichophyton tonsurans, accounting for more than 90% of cases[31]. This can be spread by contact with household members and/or exposure to contaminated clothing or grooming implements[32]. Less than 10% of cases are caused by Microsporum canis, acquired from puppies and kittens and, less commonly, Trichophyton verrucosum, which is acquired from cattle[29,33].
Diagnosis
Diagnosis is based on clinical presentation, which ranges from scaly patches reminiscent of seborrheic dermatitis (dandruff) to more commonly occurring localised patches of alopecia with scaling (see Figure 4)[29]. To help guide treatment or, in the case of diagnostic uncertainty, fungal culture of scalp scale and/or an affected hair shaft can be carried out [34].
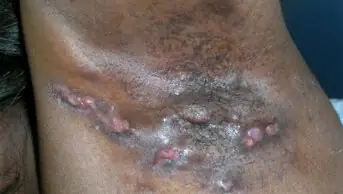
Kerion is a severe inflammatory variant of tinea capitis, which presents as a boggy pustular swelling with associated hair loss (see Figure 5)[34]. It may be accompanied by systemic upset with enlarged cervical lymph nodes and is more common in advanced disease or zoophilic transmission[29].
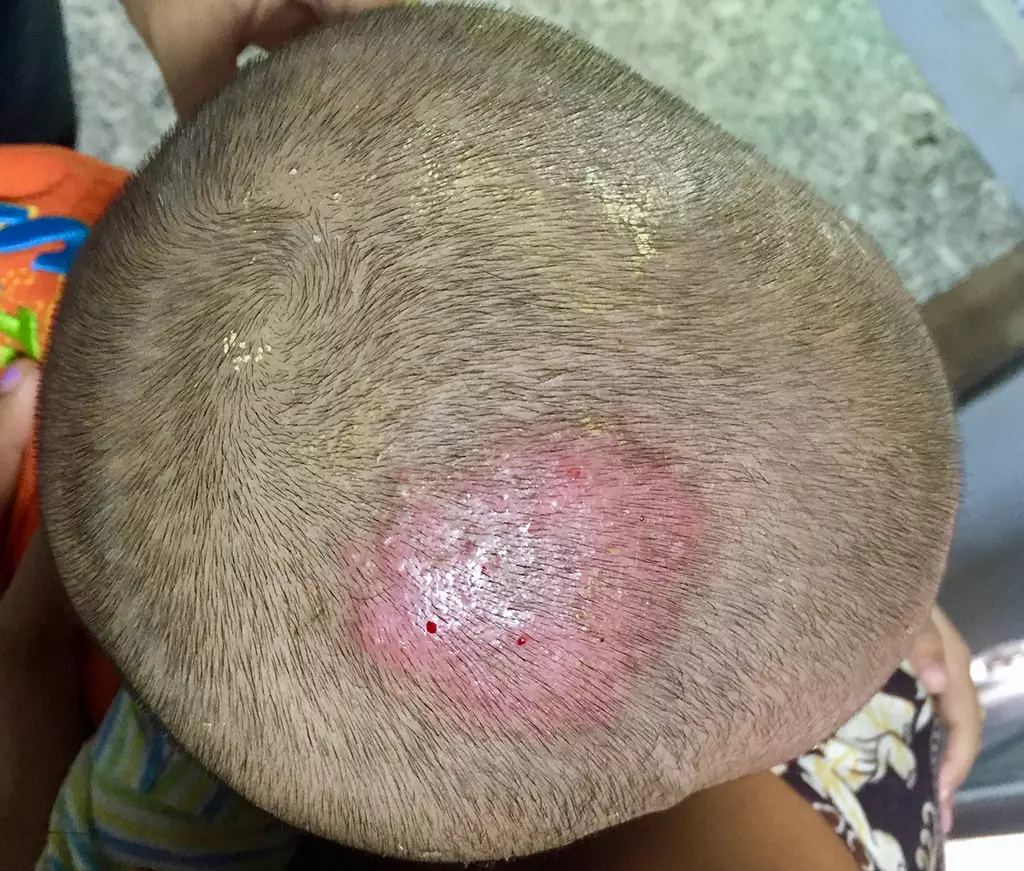
Shutterstock.com
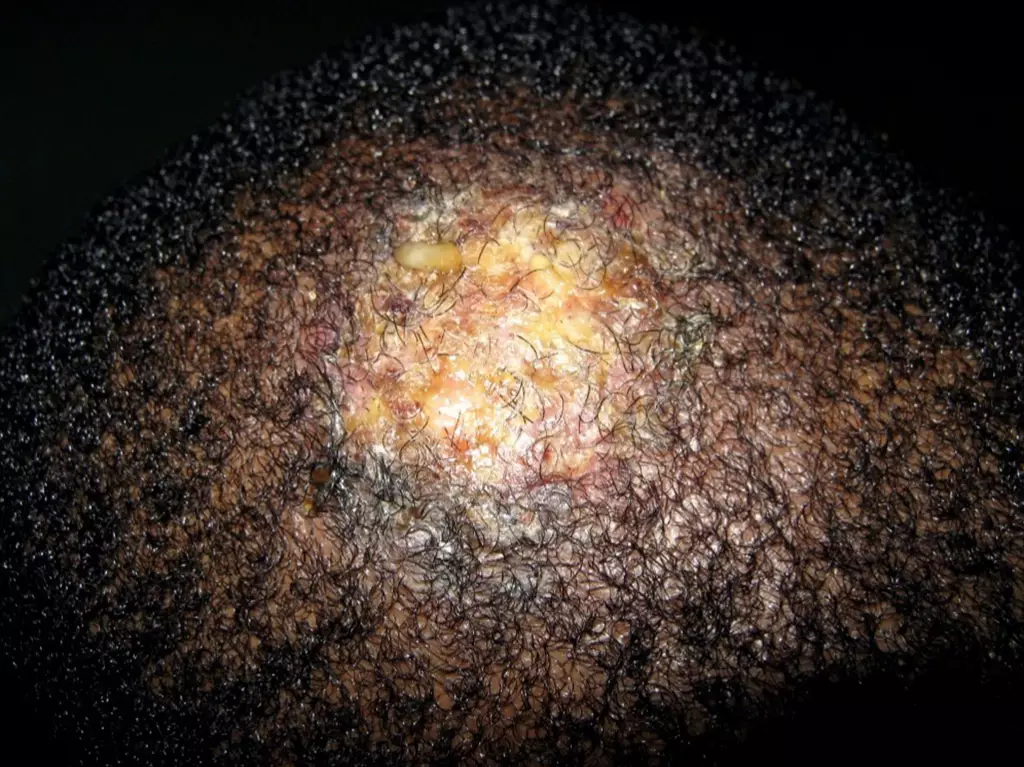
en.wikipedia.org
Management
Systemic treatment is required for the management of tinea capitis[35]. Oral griseofulvin is commonly used and is the only licensed treatment for tinea capitis in the UK[36]. The recommended dose for children aged over 1 month is 10mg/kg per day, but up to 25mg/kg may be required, and 1g for adults or children >50kg[34]. The duration of treatment depends on the organism (e.g. T. tonsurans infections may require prolonged treatment schedules) and varies between eight and ten weeks[34]. Shorter courses may lead to higher relapse rates[33].
Although unlicensed in the UK, oral terbinafine may also be used, as it is effective against all dermatophytes, including T tonsurans[37]. Dosage ranges from 3–6mg/kg per day in children, and 250mg per day in adults, for 3–4 weeks[33]. The shorter treatment course, compared with griseofulvin, may improve compliance[38]. Oral itraconazole, also unlicensed, is the agent of choice in many European countries for the treatment of tinea capitis in children at a dose of 50mg–100mg per day for 4 weeks or 5mg per kg for 2–4 weeks[34].
Topical antifungal agents are considered adjunct only and may help to reduce the risk of transmission to others[39]. Practical measures, such as washing contaminated clothing with bleach and/or disposal of items, is recommended for the reduction of infections[40]. Referral to secondary care (dermatology) is indicated if initial treatment is unsuccessful, kerion is present, or if there is diagnostic uncertainty caused by a subtle clinical presentation[41].
Delay in effective treatment of inflammatory tinea capitis can result in permanent scarring alopecia[42].

Health inequalities
The Royal Pharmaceutical Society’s policy on health inequalities was drawn up in January 2023 following a presentation by Michael Marmot, director of the Institute for Health Equity, at the RPS annual conference in November 2022. The presentation highlighted the stark health inequalities across Britain.
While community pharmacies are most frequently located in areas of high deprivation, people living in these areas do not access the full range of services that are available. To mitigate this, the policy calls on pharmacies to not only think about the services it provides but also how it provides them by considering three actions:
- Deepening understanding of health inequalities
- This means developing an insight into the demographics of the population served by pharmacies using population health statistics and by engaging with patients directly through local community or faith groups.
- Understanding and improving pharmacy culture
- This calls on the whole pharmacy team to create a welcoming culture for all patients, empowering them to take an active role in their own care, and improving communication skills within the team and with patients.
- Improving structural barriers
- This calls for improving accessibility of patient information resources and incorporating health inequalities into pharmacy training and education to tackle wider barriers to care.
- 1Lawson CN, Hollinger J, Sethi S, et al. Updates in the understanding and treatments of skin & hair disorders in women of color. International Journal of Women’s Dermatology 2017;3:S21–37. doi:10.1016/j.ijwd.2017.02.006
- 2Kelly A, Taylor S, Lim H, et al. Taylor and Kelly’s Dermatology for Skin of Color. 2nd ed. New York: : McGraw-Hill Medical 2015.
- 3Kundu R, Patterson S. Dermatologic conditions in skin of color: part I. Special considerations for common skin disorders. Am Fam Physician 2013;87:850–6.https://www.ncbi.nlm.nih.gov/pubmed/23939567
- 4Kundu R, Patterson S. Dermatologic conditions in skin of color: part II. Disorders occurring predominately in skin of color. Am Fam Physician 2013;87:859–65.https://www.ncbi.nlm.nih.gov/pubmed/23939568
- 5Handel AC, Miot LDB, Miot HA. Melasma: a clinical and epidemiological review. An Bras Dermatol 2014;89:771–82. doi:10.1590/abd1806-4841.20143063
- 6Rajanala S, Maymone M, Vashi N. Melasma pathogenesis: a review of the latest research, pathological findings, and investigational therapies. Dermatol Online J 2019;25.https://www.ncbi.nlm.nih.gov/pubmed/31735001
- 7Sofen B, Prado G, Emer J. Melasma and Post Inflammatory Hyperpigmentation: Management Update and Expert Opinion. Skin Therapy Lett 2016;21:1–7.https://www.ncbi.nlm.nih.gov/pubmed/27224897
- 8Balogun M. Skin of colour: disorders of pigmentation and hair and scalp conditions learning plan. MIMS Learning. 2021.https://www.mimslearning.co.uk/learning-paths/skin-of-colour-disorders-of-pigmentation-and-hair-and-scalp-conditions (accessed Jun 2021).
- 9Grimes P. Melasma: epidemiology, pathogenesis, clinical presentation, and diagnosis. UpToDate. 2019.https://www.uptodate.com/contents/melasma-epidemiology-pathogenesis-clinical-presentation-and-diagnosis (accessed Jun 2021).
- 10Melasma. DermNet NZ. 2020.https://dermnetnz.org/topics/melasma/ (accessed Jun 2021).
- 11Grimes PE, Ijaz S, Nashawati R, et al. New oral and topical approaches for the treatment of melasma. International Journal of Women’s Dermatology 2019;5:30–6. doi:10.1016/j.ijwd.2018.09.004
- 12Buckley D, Root T, Bath S. Specials recommended by the British Association of Dermatologists for skin disease. British Association of Dermatologists. 2018.www.bad.org.uk/specials (accessed Jun 2021).
- 13Benn EKT, Deshpande R, Dotson-Newman O, et al. Skin Bleaching Among African and Afro-Caribbean Women in New York City: Primary Findings from a P30 Pilot Study. Dermatol Ther (Heidelb) 2019;9:355–67. doi:10.1007/s13555-019-0297-y
- 14Pollock S, Taylor S, Oyerinde O, et al. The dark side of skin lightening: An international collaboration and review of a public health issue affecting dermatology. International Journal of Women’s Dermatology 2021;7:158–64. doi:10.1016/j.ijwd.2020.09.006
- 15Melasma (syn. chloasma). Primary Care Dermatology Society. 2019.http://www.pcds.org.uk/clinical-guidance/melasma-syn.-chloasma1 (accessed Jun 2021).
- 16Callender VD. Acne in ethnic skin: special considerations for therapy. Dermatol Ther 2004;17:184–95. doi:10.1111/j.1396-0296.2004.04019.x
- 17Davis E, Callender V. Postinflammatory hyperpigmentation: a review of the epidemiology, clinical features, and treatment options in skin of color. J Clin Aesthet Dermatol 2010;3:20–31.https://www.ncbi.nlm.nih.gov/pubmed/20725554
- 18Lawrence E, Al Aboud K. Postinflammatory hyperpigmentation. NCBI. 2020.https://www.ncbi.nlm.nih.gov/books/NBK559150/ (accessed Jun 2021).
- 19Fiscus V, Hankinson A, Alweis R. Minocycline-induced hyperpigmentation. Journal of Community Hospital Internal Medicine Perspectives 2014;4:24063. doi:10.3402/jchimp.v4.24063
- 20Saedi N. Post-inflammatory hyperpigmentation. UpToDate. 2021.https://www.uptodate.com/contents/postinflammatory-hyperpigmentation (accessed Jun 2021).
- 21Billero V, Miteva M. Traction alopecia: the root of the problem. CCID 2018;Volume 11:149–59. doi:10.2147/ccid.s137296
- 22Uzuncakmak TK, Kayıran MA, Tekin B, et al. Trichotillomania and Traction Alopecia. In: Hair and Scalp Disorders. InTech 2017. doi:10.5772/66746
- 23Mirmirani P, Khumalo NP. Traction Alopecia. Dermatologic Clinics 2014;32:153–61. doi:10.1016/j.det.2013.12.003
- 24Okereke UR, Simmons A, Callender VD. Current and emerging treatment strategies for hair loss in women of color. International Journal of Women’s Dermatology 2019;5:37–45. doi:10.1016/j.ijwd.2018.10.021
- 25Miteva M, Herskovitz I. Central centrifugal cicatricial alopecia: challenges and solutions. CCID 2016;Volume 9:175–81. doi:10.2147/ccid.s100816
- 26Akintilo L, Hahn E, Yu J, et al. Health care barriers and quality of life in central centrifugal cicatricial alopecia patients. Cutis 2018;102:427–32.https://www.ncbi.nlm.nih.gov/pubmed/30657802
- 27Gabros S, Masood S. Central centrifugal cicatricial alopecia. NCBI. 2021.https://www.ncbi.nlm.nih.gov/books/NBK559187/ (accessed Jun 2021).
- 28Eginli A, Dothard E, Bagayoko C, et al. A Retrospective Review of Treatment Results for Patients With Central Centrifugal Cicatrical Alopecia. J Drugs Dermatol 2017;16:317–20.https://www.ncbi.nlm.nih.gov/pubmed/28403264
- 29Support & Meetings. Cicatricial Alopecia Research Foundation. 2021.https://www.carfintl.org/support/support-and-meetings/ (accessed Jun 2021).
- 30Browning J. Dermatology Edited by Jean L.Bolognia Julie V.Schaffer LorenzoCerroni Fourth edition China: Elsevier, 2018, ISBN 978-0-7020-6275-9. Pediatr Dermatol 2018;35:289–289. doi:10.1111/pde.13439
- 31Abdel-Rahman SM, Farrand N, Schuenemann E, et al. The Prevalence of Infections With Trichophyton tonsurans in Schoolchildren: the CAPITIS Study. Pediatrics 2010;125:966–73. doi:10.1542/peds.2009-2522
- 32Borman AM, Campbell CK, Fraser M, et al. Analysis of the dermatophyte species isolated in the British Isles between 1980 and 2005 and review of worldwide dermatophyte trends over the last three decades. Med Mycol 2007;45:131–41. doi:10.1080/13693780601070107
- 33KAWACHI Y, IKEGAMI M, TAKASE T, et al. Chronically Recurrent and Disseminated Tinea Faciei/Corporis-Autoinoculation from Asymptomatic Tinea Capitis Carriage. Pediatric Dermatology 2010;27:527–8. doi:10.1111/j.1525-1470.2010.01270.x
- 34Higgins EM, Fuller LC, Smith CH. Guidelines for the management of tinea capitis. British Journal of Dermatology 2000;143:53–8. doi:10.1046/j.1365-2133.2000.03530.x
- 35Fuller LC, Barton RC, Mohd Mustapa MF, et al. British A ssociation of D ermatologists’ guidelines for the management of tinea capitis 2014. Br J Dermatol 2014;171:454–63. doi:10.1111/bjd.13196
- 36Managing scalp ringworm in children. Drug and Therapeutics Bulletin 2007;45:89–92. doi:10.1136/dtb.2007.11.0004
- 37González U, Seaton T, Bergus G, et al. Systemic antifungal therapy for tinea capitis in children. Cochrane Database of Systematic Reviews. 2007. doi:10.1002/14651858.cd004685.pub2
- 38Ghannoum MA, Wraith LA, Cai B, et al. Susceptibility of dermatophyte isolates obtained from a large worldwide terbinafine tinea capitis clinical trial. British Journal of Dermatology 2008;159:711–3. doi:10.1111/j.1365-2133.2008.08648.x
- 39Kakourou T, Uksal U. Guidelines for the Management of Tinea Capitis in Children. Pediatric Dermatology 2010;27:226–8. doi:10.1111/j.1525-1470.2010.01137.x
- 40Chen C, Koch LH, Dice JE, et al. A Randomized, Double-Blind Study Comparing the Efficacy of Selenium Sulfide Shampoo 1% and Ciclopirox Shampoo 1% as Adjunctive Treatments for Tinea Capitis in Children. Pediatric Dermatology 2010;27:459–62. doi:10.1111/j.1525-1470.2010.01093.x
- 41Mackenzie DWR. ‘Hairbrush Diagnosis’ in Detection and Eradication of Non-fluorescent Scalp Ringworm. BMJ 1963;2:363–5. doi:10.1136/bmj.2.5353.363
- 42Zaraa I, Hawilo A, Aounallah A, et al. InflammatoryTinea capitis: a 12-year study and a review of the literature. Mycoses 2012;56:110–6. doi:10.1111/j.1439-0507.2012.02219.x